Fig. 19.1
Clustered crusts of lower eyelid and forehead in impetigo. One pustule is also noted on the forehead
Two to 3 mm superficial pustules centered around follicular openings are noted in folliculitis. Folliculitis tends to be concentrated in occluded areas.” Hot tub folliculitis” is a particular type of folliculitis which occurs following being seated in a hot tub. Typically, the causative organism in “hot tub folliculitis” will be Pseudomonas aeruginosa [5, 6]. The pustules may be arranged in a linear pattern corresponding to the hot tub water levels or concentrated in areas of occlusion, such as under a tight bathing suit.
Skin and soft tissue infections due to Methicillin-resistant Staphylococcus aureus (MRSA) tend to form abscesses. These lesions are termed furuncles (one hair follicle involved) or carbuncles (more than one hair follicle involved). The lesions are erythematous and are often painful. A purulent cavity can develop which will result in an area of fluctuance (Fig. 19.2).
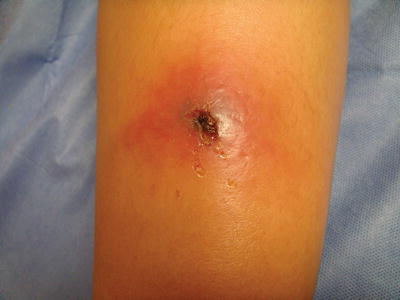

Fig. 19.2
Carbuncle due to MRSA with a central area of fluctuance
Clinical Presentation
Flaccid bullae rupture easily
Folliculitis shows small pustules
MRSA tends to form abscesses
Limited areas of impetigo can be treated topically
Institute measures in the household to limit spread
Treatment
Treatment of impetigo can be accomplished with oral or topical anti-infectives.
Incision and drainage, bleach baths, and decolonization using nasal mupirocin are all potential adjunctive therapies.
Impetigo which is confined to a limited area can be treated topically with mupirocin or retapamulin twice daily for 5–7 days. If the lesions are more extensive, oral antibiotics are prescribed for 7–10 days. The choice of the antibiotic depends on the particular organisms and sensitivities of the region in which a patient lives.
Folliculitis can be treated with antibacterial soaps, avoidance of occlusion, and, if needed, topical antibiotics. Recurrence of “hot tub folliculitis” can also be minimized by avoidance of the offending hot tub, by increasing the chlorination of the hot tub water, and/or by changing the water frequently [7]. In addition, topical clindamycin or mupirocin may help speed resolution in this variety of folliculitis.
MRSA furuncles and carbuncles are best treated with incision and drainage (I&D) [8]. Systemic antibiotics may or may not be necessary depending on the ability to adequately drain the lesions and depending on the host’s immune status. When more than one individual in a household is affected, instructions are provided to limit spread among household members, including good hand washing, keep draining wounds covered, and avoid reusing or sharing personal items [2]. Student athletes should be instructed to clean any shared equipment [4]. After the active infection is treated, decolonization with nasal mupirocin and bleach baths can be attempted [9].
Prognosis
Gutierrez et al. [1] found that black children had a higher risk for hospitalization for bacterial skin infections than white or Hispanic children. In immunocompetent children, superficial bacterial infections have a good prognosis and will generally resolve completely.
MRSA infections which spread systemically can be associated with serious complications.
Ongoing Research
Periodic microbiologic cultures in communities will assist in data collection regarding regional antibiotic sensitivities.
Conclusion
Proper diagnosis of bacterial infections of the skin will allow practitioners to initiate therapy promptly and improve patient outcomes.
Tinea Corporis
Introduction
Tinea corporis lesions result from an inoculation of dermatophyte organisms into the skin when there has been a disruption of the skin barrier. Dermatophytes are fungi that digest keratin and therefore can live in keratinized skin and scalp hairs at or above the beginning of keratinization in Adamson’s fringe.
Epidemiology
Not increased in skin of color
Trichophyton rubrum most common cause worldwide
Incidence is increased in wrestlers
Tinea corporis is a ubiquitous dermatophyte infection
Spread occurs through close contacts and fomites
Tinea corporis occurs with the same incidence in children of color as the general population. Tinea corporis is seen more frequently in the summer when there tends to be a higher incidence of insect bites, cuts, and erosions. Spread can occur with skin-to-skin contact, from tinea capitis or from fomites in households, or on common play surfaces. Tinea corporis is another one of the infections which is more common in children who engage in the sport of wrestling. The most common organism which causes dermatophytosis worldwide is Trichophyton rubrum [10, 11]. Specifically for tinea corporis, the most common causative organism in North America is also Trichophyton rubrum. In the United States and Mexico, other causes are Trichophyton mentagrophytes, Trichophyton tonsurans, Microsporum canis, and Epidermophyton floccosum.
Clinical Presentation
May develop into pustules and/or vesicles
Seen most often on exposed areas
Annular lesions with a collarette of scale are typical.
Involvement of the hair can occur in areas of dense body hair.
Lesions of tinea corporis are typically circular or annular erythematous raised lesions with scale (Fig. 19.3). More significant cases may develop a vesicular or pustular component. A deeper follicular component may be noted in areas of dense body hair, e.g., Majocchi’s granuloma. Tinea corporis lesions are most often located on exposed areas of the body. Pruritus may be noted.
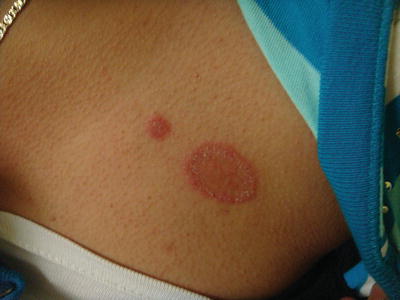

Fig. 19.3
Tinea corporis in a Hispanic adolescent
Treatment
Use topical antifungal agents for 48–96 h after clinically resolved
Topical antifungals can be used to clear tinea corporis
Oral antifungals can be required in specific settings, including hair involvement
Topical antifungals (azoles or allylamines) are applied to the lesions and to 2 cm of surrounding skin [10] twice daily for approximately 2 weeks continuing for 48–96 h after lesions appear resolved. If the lesions are more infiltrated, are located in an area with increased hair (eyelashes, beard areas in adolescents, legs or arms in some patients), or are very widespread, systemic antifungal therapy may be needed.
Prognosis
The lesions may eventually resolve spontaneously; however, treatment is recommended to hasten resolution and to avoid continued self-inoculation. In skin of color, postinflammatory dyspigmentation may present unique challenges (Fig. 19.4). Patients who are diagnosed with tinea corporis should be cautioned to avoid contact with individuals, fomites, or pets that may carry the organisms to decrease the incidence of reinfection. Topical corticosteroids should be avoided as they may cause enlargement of the lesion and poor response to antifungals.
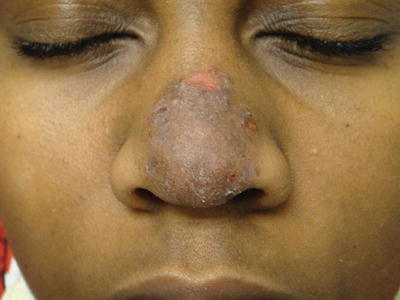

Fig. 19.4
Postinflammatory hyperpigmentation noted in a healing lesion of tinea corporis
Ongoing Research
Ongoing studies to determine the etiologic agents of tinea corporis provide useful information regarding the incidence of each organism and can direct therapeutic options.
Conclusion
Tinea corporis is a benign cutaneous infection which clears with azole antifungals; however, in skin of color the postinflammatory changes can cause parental concern. Reduction in transmission of disease is important in households to contain the spread of the infection.
Pityriasis Versicolor
Introduction
Pityriasis versicolor aka tinea versicolor (TV) is a superficial yeast infection of the skin. The causative organism is the yeast form of the dimorphic fungus of the Malassezia genus. The organisms have also been known as Pityrosporum orbiculare or ovale. The organism is lipophilic and tends to be concentrated in areas with increased sebaceous glands.
Epidemiology
No consensus as to whether incidence is increased in skin of color
Increased incidence in summer and in tropical climates
Increased in pregnancy, diabetes, and immunosuppression
Tinea versicolor is a common cutaneous yeast overgrowth
Evidence regarding whether the incidence is different in skin of color is not conclusive [12]. However, it is clear that the pigmentary changes can alter the clinical presentation. The incidence of pityriasis versicolor is increased in the summer, in tropical climates, during pregnancy, and in association with diabetes and immunosuppression.
Clinical Presentation
Lesions have powdery scale
Facial involvement noted in prepubertal children
Scale may be hypopigmented or hyperpigmented
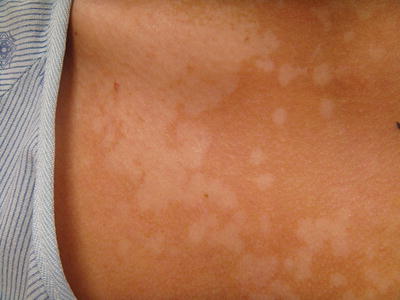
Hypopigmented annular plaques of the head, upper chest, and back are typical for Black or African-American patients.
Hyperpigmented to pink plaques with minimal scale are noted in many patients with Fitzpatrick phototypes I–V
TV lesions are macules with powdery scale which may coalesce into patches. The usual locations are the upper back and upper chest (Fig. 19.5). However, in prepubertal children, the lesions may be present on the face [10]. The lesions may be hypopigmented or have a brownish coloration. In more richly pigmented skin, the lesions may have a follicular orientation [13] and be more obviously hypopigmented. The Malassezia organism is difficult to culture; thus diagnosis is made based on the clinical appearance and/or potassium hydroxide preparations [14]. Wood’s lamp examination in some instances shows pale yellow fluorescence [10]. Biopsy of pityriasis versicolor in skin of color shows a thicker stratum corneum, more tonofilaments in the granulosum, and more sequestered melanosomes [12].