Perioperative Care
Desmond B. Henry
The term perioperative care refers to all the clinical activities that take place around a surgical intervention, from the preoperative assessment to the postoperative discharge.1-3 In modern institutions, perioperative care is performed in a defined physical area that usually accommodates scheduling, admission, preoperative preparation, the procedure itself (the operating room or a procedural suite), recovery from the procedure (phase I and II), and discharge. Support services—including sterile processing, materials management, the pharmacy, the laboratory, pathology, diagnostic imaging—are frequently adjacent. The success and subsequent demand for new procedures such as cardiac catheterization or endoscopy, which are not strictly surgical but require expertise and equipment similar to surgery, have created a need to duplicate existing perioperative resources in other areas. The same principles that are detailed here for surgical procedures apply to these procedural areas.
PREOPERATIVE ASSESSMENT AND CARE
Anxiety is experienced by nearly all parents and children at the prospect of surgery and anesthesia. Preparing children for their surgical and operating room experience should begin before the patient ever makes contact with their anesthesiologist. The surgeon or primary care provider should be the first ones to ensure that the child receives the best perioperative care possible and to assure the child’s family that this will be the case, answering their questions or facilitating access to someone who can answer them.
Many institutions arrange orientation and preoperative tour days before surgery to instruct and educate the child and parent on what to expect. As part of the preoperative program, most of these institutions have developed “child-friendly” environments, with coloring books, tours, videos, and the invaluable help of a child-life specialist to help reduce the level of anxiety. Allowing children to take a favorite toy or blanket into the operating room provides great comfort to many children.1,4
The primary goal of preoperative assessment and care is preparing a patient for surgery. This involves (1) screening for conditions that may require consultation workup or treatment, (2) optimizing any preexisting medical problems, and (3) counseling patients and parents about the expected course of anesthesia and surgery. The anesthesiologists should make every effort to see the child and the family to understand their needs and expectations and to perform a complete preoperative evaluation. The anesthetic, postoperative pain management, and discharge plans can be all be explained to the child, if appropriate, and to the family at this time. This is also a good opportunity to obtain informed consent.
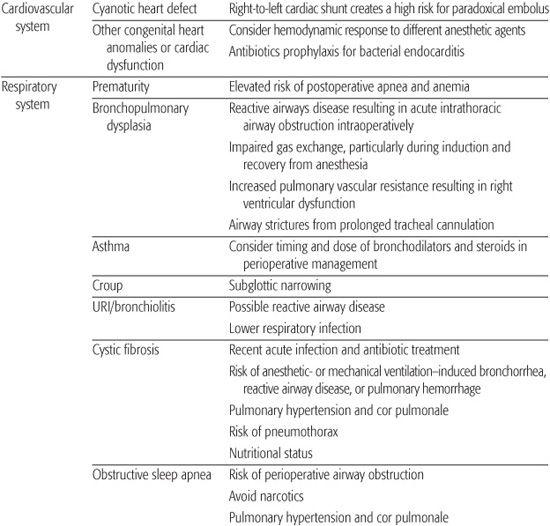
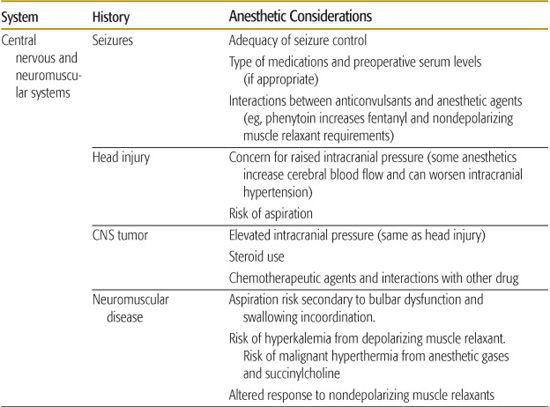
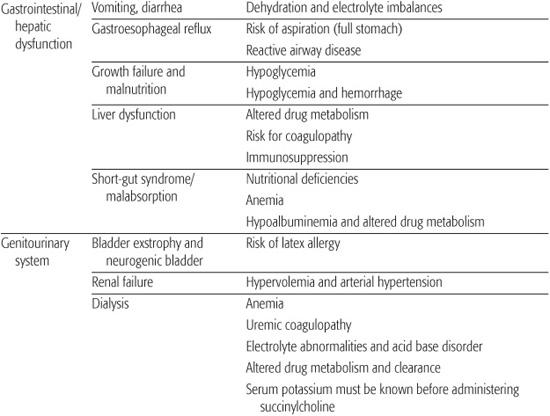
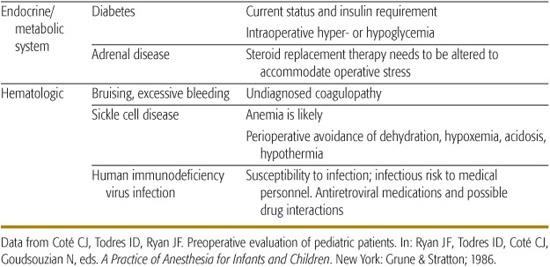
The preoperative evaluation usually consists of a careful history and an oriented physical examination aimed at establishing surgical risk and designing anesthetic planning and postoperative care. The physical examination should be sufficiently complete to detect any major problems and should be informed by the medical history (Table 112-1).
 LABORATORY EVALUATION
LABORATORY EVALUATION
Because of low predictive value and cost-effectiveness, many centers no longer perform routine laboratory screening tests in otherwise healthy children scheduled for minor elective surgery.4,6-10 However, important baseline values (eg, hemoglobin level determination) in anticipation of major blood loss or specific diagnostic tests to rule major organ-specific pathology are still performed. At present, there are no universal guidelines concerning preoperative laboratory testing; many anesthesiologists follow institutional protocols or their own personal preferences.
Mild anemia (Hb ≥ 9.5 g/dL) has been reported in up to 2% of pediatric patients undergoing elective surgery. No studies to date have shown justification to modify the perioperative management in otherwise healthy children who have a borderline low hemoglobin concentration, and therefore routine hemoglobin determinations are usually not necessary.5,11,12 However, it is reasonable to obtain preoperative hemoglobin values in (1) former preterm infants (postoperative apnea), (2) patients with chronic illness, (3) children with sickle cell disease (including sickle cell anemia, sickle Hb C disease, and the sickle thalassemias), and (4) those instances where having a baseline hemoglobin value may be useful (along with blood typing and cross-matching) in anticipation of significant surgical loss. In patients with sickle cell disease, the optimal level of sickle Hb and the role of transfusion to avoid perioperative complications in different categories of surgery and anesthesia (regional vs. general) is still unknown. Perioperative evaluation and management of patients with this disease is best performed in conjunction with the patient’s hematologist and surgeon.
Routine coagulation screening also has a weak predictive value for assessing the risk of surgical bleeding in patients with no history of abnormal bleeding.5,13-17 Screening is only advisable in patients in whom a hemostatic defect is suspected either by history or physical examination, patients in whom minimal postoperative bleeding could be critical (eg, neurosurgical interventions), or when the surgical procedure is likely to cause perioperative coagulation dysfunction (eg, cardiopulmonary bypass).
The value of routine preoperative pregnancy testing in women of childbearing age, particularly in adolescent females, is controversial. There is no scientific evidence that short-term exposure to anesthetics can induce spontaneous abortions or congenital malformations. However, surgery involves physical and psychological stresses, and exposure to X-rays and nonanesthetic medications may result in finite fetal risk.
Table 112-1. The Preanesthetic History, Systemic Review, and Related Anesthetic Implications

Arguments against preoperative pregnancy testing are based on lack of demonstrated cost-effectiveness and on confidentiality and consent issues.18-28
SPECIFIC ISSUES THAT INFLUENCE ANESTHETIC MANAGEMENT
Obstructive Sleep Apnea Several studies have indicated that there is an increased risk of postoperative respiratory difficulty in patients with moderate to severe obstructive sleep apnea, and a majority of anesthesiologists will hospitalize these patients for postoperative respiratory monitoring.
Children older than 3 years of age and who have mild obstructive sleep apnea uncomplicated by comorbid conditions do not routinely require admission and often have their surgery performed in day surgery centers.29-36
Preoperative Fasting Preoperative fasting is recommended to prevent aspiration of particulate material and liquids into the lungs while the airway-protective reflexes are suppressed under an anesthetic (Table 112-2). However, fasting is eminently difficult to enforce with children, not only because the child is unlikely to see the benefits, but also because prolonged fasting is ill advised in small infants or debilitated children who may have reduced glycogen stores. Any attempt to implement unreasonable fasting criteria is an invitation for violation, which may happen without family knowledge if the child is old enough. Several studies have confirmed the safety of having clear liquids (apple juice, glucose-electrolyte solutions) up to 2 to 4 hours preoperatively in healthy infants and children (see Table 112-2).5,37
Upper Respiratory Infection Anesthesiologists and surgeons often face decisions regarding children who are experiencing respiratory symptoms at the time of a scheduled surgery. Upper respiratory infections (URIs) are very common in children, averaging 5 to 10 episodes per year, especially in those under the age of 2 years. The prevalence is even higher in children with chronic illnesses and those who attend daycare centers; therefore, sometimes the scheduling of elective surgery is a gamble. Some studies indicate significant risk for laryngospasm, bronchospasm, arterial O2 desaturation, and postextubation stridor in children who are suffering from an URI, whereas other studies did not show major increased risk.4,38-50 There is still controversy among pediatric anesthesiologists on whether to proceed with surgery in the presence of a current or recent URI. The decision often depends on the experience of the anesthesiologist and the type and urgency of the surgery. Most anesthesiologists postpone elective surgery if the patient exhibits one or more of the following: fever, ill appearance, purulent rhinorrhea, tachypnea, or involvement of the lower respiratory tract.
Table 112-2. American Society of Anesthesiologists Fasting Guidelines
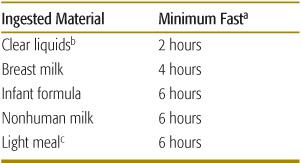
a Fasting times apply to all ages.
b Water, fruit juice without pulp, carbonated beverages, clear tea, and black coffee
c Dry toast and clear liquid. Fried or fatty foods may prolong gastric emptying time. Both amount and type of food must be considered.
The guidelines recommend no routine use of gastrointestinal stimulants, gastric acid secretion blockers, or oral antacids.
Newborn Apnea Infants born prior to 37 weeks gestational age who are less than 56 weeks postconceptional age at the time of surgery are at greater risk of anesthetic complications than full-term infants. Apnea, periodic breathing, and bradycardia are common during and after general anesthesia or sedation.48,49,51-53 As a rule, these patients should be admitted overnight for cardiopulmonary monitoring or at least undergo in-hospital prolonged observation prior to discharge. Limited data suggest that spinal anesthesia may offer a lower risk of respiratory depression in young infants, but data in the literature are in conflict. Full-term infants (gestational age greater than 37 weeks) require overnight admission or extended observation if they are less than 44 weeks post-conceptional age at the time of surgery.54,55
Bronchopulmonary Dysplasia Preoperative evaluation in children with bronchopulmonary dysplasia should include an assessment of the severity of their mechanical and gas-exchange abnormalities (see Chapter 102). Hypercapnia, metabolic alkalosis (elevated serum bicarbonate), hypochloremia, and hypokalemia are common is patients with severe disease and are often aggravated by the chronic use of loop diuretics. Hepatomegaly may indicate the presence of right ventricular dysfunction and suggests a limited cardiac reserve. A preoperative echocardiogram will confirm the presence of right-atrial and ventricular hypertrophy and enlargement and affords the opportunity to estimate the right-ventricular pressures.
Infants and children with bronchopulmonary dysplasia are often treated with opioids and benzodiazepines and may therefore exhibit tolerance to these medications. Growth failure, chronic malnutrition, and the ensuing hypoproteinemia may affect the pharmacology of anesthetic drugs. Patients with hepatic congestion may also suffer from impaired hepatic clearance of drugs. Prolonged diuretic therapy may cause calcium wasting, nephrocalcinosis, and impaired renal function. Infants treated with long-term corticosteroids require treatment with “stress” corticosteroid doses in the perioperative period.
Asthma It is important for anesthesiologists to recognize the various presentations of asthma before surgery is undertaken. Active wheezing or decreased breath sounds indicate active airway obstruction and, if possible, should prompt a deferral of surgery until the airway obstruction is relieved. Preoperative pulmonary function testing is not necessary unless used to optimize the drug regimen in the patient with severe disease. It is usually recommended that all preoperative treatments be continued through the morning of surgery. In addition, some anesthesiologists routinely administer a nebulized beta-adrenergic agonist before inducing anesthesia. Patients who have received chronic steroid therapy, either systemically or at high doses via aerosol, should be treated with stress corticosteroid doses. Anesthetic induction can be accomplished by any route. At present, sevoflurane is the inhalational agent of choice, because it does not irritate the airways and has bronchodilatory effects. Among the intravenous anesthetics, ketamine has been proposed as a last resort adjuvant in the treatment of status asthmaticus, because it causes bronchodilation. Propofol has less hista-mine-releasing effects than other rapid acting sedatives and therefore is often preferred to etomidate or thiopental for induction or short anesthetic courses in asthmatic patients. A slow, smooth emergence from anesthesia minimizes the risk of bronchospasm. Unless contraindicated, many anesthesiologists proceed with extubation under deep anesthesia to minimize airway irritation during emergence, when airway reflexes may be enhanced.
Sickle Cell Disease Appropriate preoperative evaluation and preparation is mandatory in children who suffer from the various forms of this disease. Children who have experienced frequent crises, including acute chest syndrome, or who require multiple transfusions represent a particularly high anesthetic risk.
Although there is no ideal anesthetic technique, perioperative complications may be minimized by vigilant observation, adequate pain control, and careful avoidance of dehydration or any other circumstances that lead to decreased tissue perfusion or arterial oxygenation. The choice of transfusion strategy before surgery depends on the patient’s history and should be carefully planned in conjunction with the patient’s pediatrician, hematologist, and surgeon.
ANESTHETIC RISK ASSESSMENT
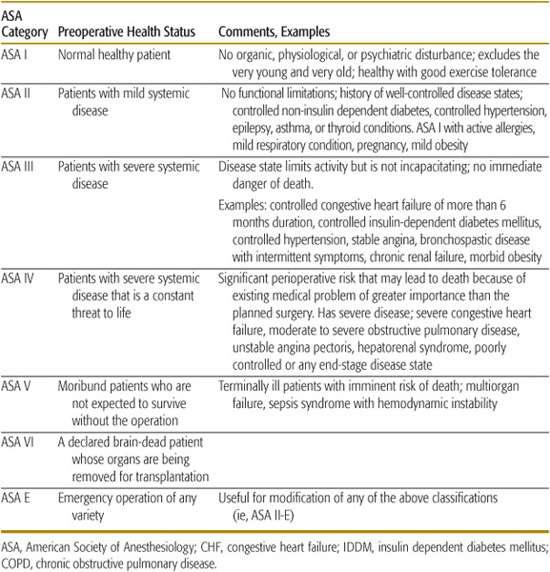
The risk of anesthesia and surgery depends to a large extent on the child’s health and the complexity of the surgery. The most common classification often used to determine the relative risk is the ASA Physical Status Classification (Table 112-3); it is important to note that the ASA classification does not account for the risk of the surgery itself or for the existence of multiple diseases.
Table 112-3. ASA Physical Status Classification
INTRAOPERATIVE MANAGEMENT
Intraoperative management requires complex skills beyond the scope of this chapter. However, pediatricians should have some familiarity with the various components of this management, especially those that may affect the postoperative course or that may raise questions by the family.
 INDUCTION OF ANESTHESIA
INDUCTION OF ANESTHESIA
The main goal of the induction phase is to achieve surgical anesthesia in a manner that is fast, smooth, and least distressing for the patient. In children, this is usually best accomplished by using inhalational rather than intravenous agents. Ultimately, the choice of anesthetic induction technique is determined by the patient risks, the state of health, and the circumstances of the moment. For instance, in a child at risk for aspiration, a rapid intravenous sequence results in safer cannulation of the airway and is preferable to an inhalational induction.
In a typical induction, the child is brought to the operating room area, often accompanied by a parent and a favorite toy. Monitoring equipment, including a pulse oximeter, electrocardiographic electrodes, and a blood pressure cuff, is placed gently on the child. Next, a face mask carrying oxygen and frequently mixed with nitrous oxide is carefully placed on the child’s face. One to 2 minutes of inhaling nitrous oxide induces a state of euphoria. At this point, an inhalational anesthetic such as sevoflurane is introduced into the inhaled gas mixture. Once the child is unconscious, an intravenous line is started and more comprehensive intraoperative monitoring is applied if appropriate. Surgical anesthesia can be maintained by spontaneous ventilation with a mask. However, it is usually safer to secure the airway either with a supraglottic device or an endotracheal tube.
 CHOICE OF ANESTHETIC
CHOICE OF ANESTHETIC
There is a wide choice of inhalational anesthetics, but sevoflurane, desflurane, isoflurane, and enflurane are the ones most commonly used in the United States. Dosing with these agents is defined by the minimum alveolar concentration (MAC), which is the alveolar concentration that provides sufficient depth of anesthesia for surgery in 50% of patients. For most potent inhalational agents, the alveolar concentration reflects the arterial concentration of anesthetic in the blood perfusing the brain. Thus, the MAC is an indication of anesthetic potency analogous to the ED50. Inhalational anesthetics have the advantage of producing both a rapid onset and a rapid offset of anesthesia. The less soluble the agent is in the blood (ie, the lower the blood/gas partition coefficient of the anesthetic), the faster will be the induction and the emergence from anesthesia. Inhalational agents are also convenient to administer (as they do not require special access) and provide profound amnesia and excellent analgesia. However, among their disadvantages, they cause airway irritation (thus rendering the patient more likely to cough or develop laryngospasm, bronchospasm, or breath-holding) and nausea and vomiting.
Intravenous anesthetics belong in several pharmacological families, including but not limited to barbiturates, narcotics, and benzodiazepines. They have the advantage of speed—generally inducing anesthesia more rapidly than inhalational agents—without some of the complications. On the other hand, they require intravenous access, which is threatening to a usually already apprehensive child. All intravenous agents have some effect on cardiorespira-tory function, usually including some degree of respiratory depression, apnea, and hypotension.
Maintenance of Anesthesia During surgery, the obvious expectation is that the patient remain asleep, unaware of pain, unresponsive without motion, and hemodynamically stable. Anesthesia is usually maintained with nitrous oxide, an inhalational anesthetic, and an opioid to increase intraoperative and postoperative analgesia. Benzodiazepines are often given as premedication or intraoperatively to supplement hypnosis and amnesia. A nondepolarizing muscle relaxant (vecuronium or rocuronium) provides neuromuscular blockade if needed. Some of the medications used in pediatric anesthesia are listed in eTable 112.1  , along with their most common side effects. A discussion of the use of bispectral index (BIS) monitoring is available on the book DVD.
, along with their most common side effects. A discussion of the use of bispectral index (BIS) monitoring is available on the book DVD.
Postoperative Care The main goal of postoperative care is to ensure smooth return from anesthesia and surgery to patient’s baseline state. The initial recovery period is critical; up to 13% of all reported adverse events occur at this time. Therefore, it is essential that every facility where children undergo surgery has a well-equipped postanesthesia recovery unit with dedicated nursing staff able to detect and manage immediate postoperative problems. Following arrival at the unit and proper briefing by the anesthesiologist, staff should maintain a constant surveillance of airway patency, ventilation, and circulatory function. A patient is usually deemed stable enough for discharge when consciousness is fully recovered, postoperative nausea and vomiting are controlled, and pain is relieved. There are several scoring systems for determining discharge readiness in the PACU (see eTables 112.2  and 112.3
and 112.3  ).58-68
).58-68
REFERENCES
See references on DVD.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


