Fig. 38.1
Neonatal acne consisting of small pinkish-red inflamed papules and pustules mostly confined to the cheeks, eyelids, and forehead
The pathogenesis of neonatal acne is unclear. Sebum production and Malassezia species have been implicated, but, their exact role has not been clarified [29].
The condition is usually mild and always self-limited. Typically, reassurance is all that is needed. In more extensive cases, treatment with ketoconazole 2 % cream can improve the eruption [30].
Infantile Acne
Infantile acne typically appears around 6 months of age and may last 1–2 years. Boys are more frequently affected than girls. Clinically, infants present with classic acne lesions: open and closed comedones, inflammatory papules, and small pustules (Fig. 38.2). Uncommonly, severe nodular acne may be seen [31]. Small, pitted scars are commonly observed sequelae of infantile acne, occurring in up to 50 % of affected infants [32]. Parents may be counseled that infantile acne is associated with a strong family history of acne and may be associated with more severe adolescent acne [33].
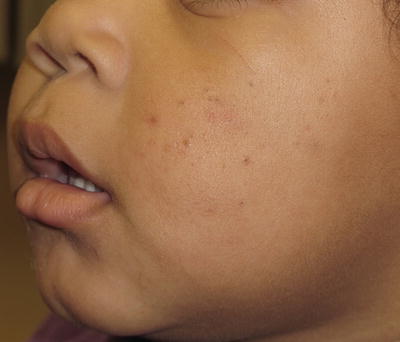

Fig. 38.2
Infantile acne consisting mostly of open comedones scattered over the cheeks
The pathogenesis of infantile acne is due to the transient overproduction of androgens by the developing adrenal gland. Increased dehydroepiandrosterone sulfate (DHEAS) is noted, with an increased production of testicular androgens in boys as well [33]. The majority of cases are not the result of clinically significant hormonal abnormities. However, a thorough physical examination including growth (height, weight, and growth curve), testicular growth and breast development, presence of hirsutism, and increased muscle mass should be done. If signs of precocious puberty are noted, a hormonal work-up should be undertaken [31, 34]. Serologic evaluation should include follicle-stimulating hormone (FSH), luteinizing hormone (LH), testosterone, DHEAS, 17-OH-progesterone, serum cortisol, thyroid studies, and a bone age [31].
Treatment involves gentle, “baby friendly” formulations of topical retinoids (adapalene 0.1 % gel or tretinoin 0.025 % cream) and topical antimicrobials (benzoyl peroxide 2.5 % cream). Washes and alcohol-based gels should be avoided. An open-label trial of adapalene 0.1 % gel in 12 patients with infantile acne demonstrated a reduction of inflammatory and noninflammatory lesions in 4 months [35]. Side effects were mild and did not require discontinuation of the medication. At 1-year follow-up, there was no observable scarring [35]. Oral antibiotics appropriate for babies, such as erythromycin or azithromycin, are used for moderate-to-severe cases and oral isotretinoin may be considered for the very rare cases of severe nodular disease [31].
Mid-Childhood Acne
Mid-childhood acne, defined as acne occurring in children aged 1–7 years, is rare [31]. At this age, children should not produce significant levels of adrenal or gonadal androgens; therefore, an endocrine abnormality should be suspected in any child presenting with acne during this time frame. A thorough physical examination, evaluating for signs of precocious puberty, should be performed. A referral to a pediatric endocrinology is usually warranted to rule out adrenal or gonadal pathology such as androgen-secreting tumors as well as evaluating for other causes of precocious puberty. Congenital adrenal hyperplasia is more common in some groups with skin of color such as Hispanics and atypical cases may not have been noted in infancy [36]. Early adrenarche can be also seen in girls at risk for polycystic ovarian syndrome (PCOS). With a negative work-up, treatment is similar to adolescent acne (see below) with the exception of oral tetracycline and doxycycline which are contraindicated in those 8 years and younger due to risk of bone and dental enamel damage [31]. Minocycline is not approved for use in children less than 12 years of age.
Preadolescent Acne
Acne in the preadolescent period (ages 7–11) is a not uncommon, and the incidence appears to be on the rise [17, 29, 31]. Early acne presents as mostly comedones in the T-zone, involving the forehead and central face with occasional inflammatory papules (Figs. 38.3 and 38.4) [31]. Comedones can also appear in the concha bowl of the ear. In girls of any ethnicity, an early onset of acne (<10 years of age) may be indication of more severe adolescent acne [37]. If there are signs of androgen excess, then the appropriate work-up should be done. PCOS is important to consider in severe acne and/or that recalcitrant to treatment. Screening questions regarding irregular menstrual cycles, excessive premenstrual symptoms, and hirsutism may guide management. Treatment is similar to adolescent acne with an emphasis on simplifying treatment plans to aid with adherence. While limited, there are some therapeutic trials in this younger age group [38–40]. These are discussed below.
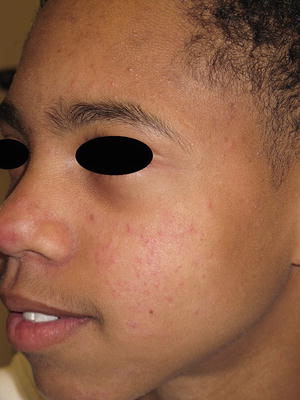
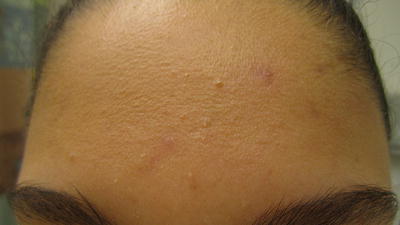

Fig. 38.3
Preadolescent acne consisting mostly of closed comedones and small pink papules

Fig. 38.4
Preadolescent acne concentrated in the “T-zone” area of forehead
Adolescent Acne
As mentioned above, acne is one of the most common disorders of adolescence in all ethnic backgrounds. There are limited studies comparing the differences in acne characteristics between differing skin types. Some studies have indicated that Caucasians and Hispanics are more prone to nodulocystic acne than African Americans [41, 42].
The diagnosis of acne is usually straightforward and made clinically by the presence of classic acne lesions: open and closed comedones (Fig. 38.5), inflammatory papules and pustules (Fig. 38.6), and nodules in more severe disease. These lesion types are present in all skin tones. However, erythema may be more challenging to appreciate in darker skin tones and may appear dark, resembling postinflammatory hyperpigmentation. To help differentiate, active lesions may be palpated for induration or tenderness [43].
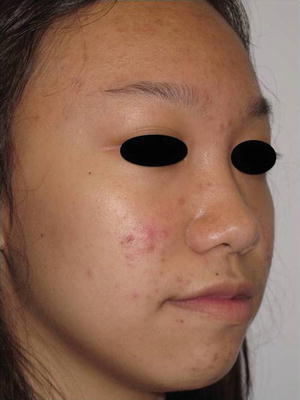
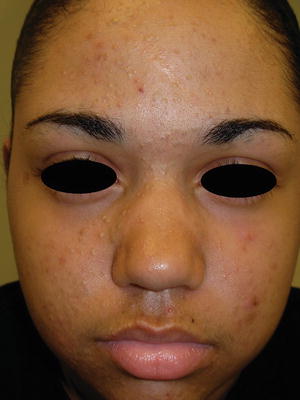

Fig. 38.5
Adolescent acne in an Asian female demonstrating moderate inflammatory and comedonal acne

Fig. 38.6
Deep comedonal acne in an adolescent
A differential must be considered especially when traditional treatments are not effective [44]. The differential includes gram-negative folliculitis, pityrosporum folliculitis [45], steroid-induced acne, keratosis pilaris, eruptive hidradenoma, molluscum contagiosum, pseudofolliculitis barbae, acne keloidalis nuchae [46], and hidradenitis suppurativa. Additionally, it is important to evaluate for any systemic hormonal abnormalities that may cause acne such as PCOS, hormone-secreting tumors, or autoinflammatory disorder such as SAPHO (synovitis, arthritis/acne, palmar pustulosis, hyperostosis, osteitis).
Sequelae
The sequelae of acne are a crucial consideration when considering a treatment regimen in skin of color patients. Postinflammatory hyperpigmentation (PIH) and hypertrophic/atrophic scarring or keloid formation can result.
PIH is characterized by hyperpigmented macules or patches that can occur at sites of acne or result from irritation caused by acne treatment. Often, PIH secondary to acne may be the chief complaint at presentation (Fig. 38.7) [47]. African Americans (65 %) and Hispanics (48 %) have a higher prevalence of PIH than Asians (18 %), Continental Indians (10 %), and Caucasians (25 %) [3, 41]. Although African Americans may experience less severe nodular acne, their acne may have a higher degree of inflammation when evaluated histologically [48, 49], thus contributing to the propensity for PIH [50]. In general, when the pigment is within the epidermis, it appears lighter and better circumscribed (epidermal melanosis). When the pigment is in the dermis, it appears darker gray and less demarcated [51]. PIH can cause significant stress and frustration as dermal hyperpigmentation and epidermal melanosis may take years and 6–12 months to fade, respectively [52].
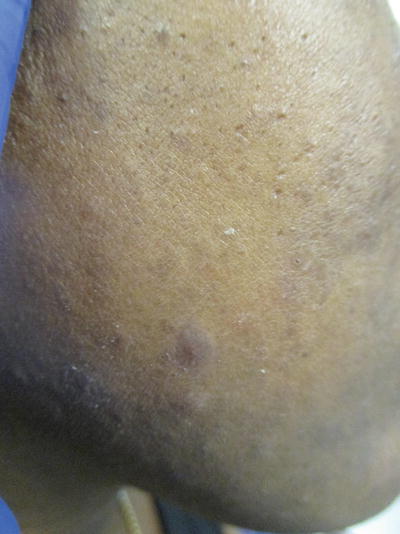

Fig. 38.7
Sequelae—Postinflammatory hyperpigmentation
Keloids (Fig. 38.8) and hypertrophic/atrophic (Figs. 38.9 and 38.10) scarring formation occur between 5 and 16 times more often in skin of color, and can result in significant and permanent disfigurement [50]. Pain and itching are common symptoms. The biologic basis of keloidal/hypertrophic scarring has been widely explored. There are multiple contributing factors such as differences in fibroblast size and activity, immune cell action, and growth factors that result in the promotion of excess collagen and inhibition of extracellular matrix degradation [53, 54]. Treatment of keloids is exceptionally challenging and often unsuccessful.
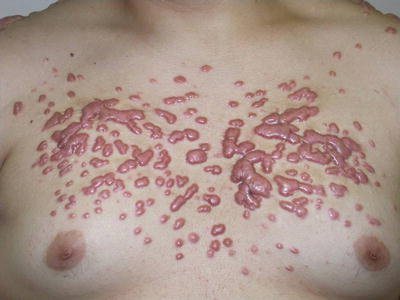
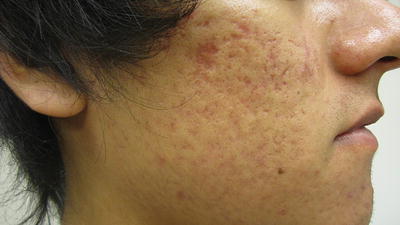
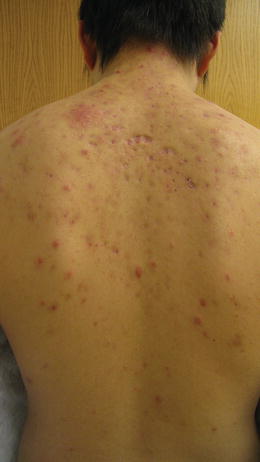

Fig. 38.8
Sequelae—Extensive keloids due to acne fulminans in an adolescent

Fig. 38.9
Sequelae—Atrophic scarring due to nodulocystic acne

Fig. 38.10
Mixture of inflammatory acne and atrophic scarring
Special Considerations
It is important to inquire about topical beauty products used in all patients, but it is especially crucial in those with skin of color. There are different perceptions of acne and beauty and subsequent practices range widely among different groups. It is impossible to generalize for each group, but hair care practices, cultural remedies, and over-the-counter treatments can play a major role in acneiform eruptions [7]. For example, one study examining practices in Arab Americans found patients used mixtures of honey and sugar to exfoliate, lemon juice or a milk and honey blend to wash the face, and mixture of herbs and Dead Sea clay to make facial masks [55]. Cocoa butter is also a popular product among African Americans and can be comedogenic [56].
Furthermore, astringents, scrubs, buffs, toners, and sonic brushes are used regardless of background or skin type. The goal of facial cleansing is to remove makeup, dirt, and excess oil [57]. Excessive and harsh cleansing routines predispose one to increased transepidermal water loss, bacterial colonization, and comedone formation, and can result in inflammation [58, 59]. This is especially problematic in those with skin of color as increased erythema and irritation can cause PIH.
Hair Care Practices
Africans, Afro-Caribbeans, and African Americans often use hair pomades to improve texture, assist in manageability, and reduce brittleness of hair [26, 41, 56, 60]. A survey of patients at a skin of color clinic found 46 % of patients used hair oil or pomades and 70 % of these patients had forehead acne [41]. Hair pomades and oils often contain lanolin, coconut oil, squalene, mineral oil, and isopropyl myristate which are known to be comedogenic. These result in a monomorphic acne called pomade acne [60]. There is even one study that suggests that use of hair oils may contribute to early menarche [61]. The authors speculate that hair oils often contain placenta, estrogen, and endocrine-disrupting chemicals (EDCs), such as mono-ethyl phthalate or methylparaben that may accelerate puberty [61]. Further studies on the hormonal effects of these substances are needed. However, inquiring about hair products is essential, and recommending silicone or water-based gels as alternatives can prevent this type of acne [26, 56].
Skin-Lightening Practices
The use of skin beaching agents is common in skin of color [41]. Beauty stores that specialize in African, Afro-Caribbean [62], African-American, and Asian products frequently have aisles containing products devoted to skin lightening, demonstrating its popularity [43, 53]. Many of these products are imported and contain potent corticosteroids such as clobetasol propionate and are sold under the names of Dermovate, Betnovate, Topsone, and Movate. It is also common for patients to obtain products while traveling abroad, or from friends and family members visiting the United States. In a dermatology clinic in Dakar, Senegal, over half the women were current users of bleaching products. Products used contained hydroquinone (4–8.7 %), corticosteroids (usually class I), mercury iodide, and other caustic agents [63]. These products can result in steroid-induced acne [46, 63] (Fig. 38.11) and cause other problems such as skin atrophy, hypopigmentation, erythema, and telangiectases. A prospective study in Lome, Togo examined acne in patients who were bleaching their skin, and found the main areas for acne lesions were on the back and shoulders [64]. There are also increased rates of steroid-induced acne in India and Hong Kong due to lax regulation on topical steroids and widespread use [7].
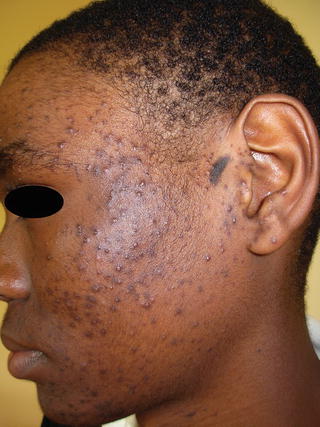

Fig. 38.11
17-year-old Tanzanian male with steroid-induced acne due to over-the-counter clobetasol used for skin bleaching
Treatment
1.
Treatment is two-part: controlling the acne and then managing its sequelae.
2.
Treat acne in skin of color early and aggressively to prevent long-term side effects: postinflammatory hyperpigmentation, hypertrophic/atrophic scarring, and keloids.
3.
Tailor treatment strategies (age, medication tolerance, risk of scarring) towards individual skin type.
Treatment of acne in skin of color should be done early and aggressively to prevent PIH and scarring. There are published acne treatment guidelines for both children and adolescents [31, 65]. Modified guidelines for Asian patients [7] can be applicable to all skin of color patients [26]. Therapy should be carefully tailored to treat acne without inducing too much irritation that will result in PIH. The main difference in treating acne in darker skin tones is that treatment is not over after the acne is under control. The second stage of treatment addresses the aftermath of acne.
With the multifactorial components of acne pathogenesis, current acne therapies target individual factors contributing to acne formation. Ideally, treatment regimens combine therapies to address multiple pathogenic factors simultaneously. Patient expectations need to be managed; allowing them to understand effectiveness may not be appreciated for 8–12 weeks. Table 38.1 provides a treatment algorithm based on severity.
Table 38.1
Treatment algorithm for acne in skin of color
Mild | Moderate | Severe | |||
|---|---|---|---|---|---|
Comedonal | Papular/Pustular | Papular/Pustular | Nodular | Nodular | |
First choice | Topical retinoid | Topical retinoid + topical antimicrobial | Oral antibiotic + topical retinoid ± BP | Oral antibiotic + retinoid + BP | Oral isotretinoin |
Alternatives | Alt. topical retinoid or azelaic acid or salicylic acid | Alt. topical retinoid antimicrobial agent + alt. topical retinoid or azelaic acid | Alt. oral antibiotic + alt. topical retinoid ± BP | Oral isotretinoin or alt. oral antibiotic + alt. oral topical retinoid ± BP/azelaic acid | High dose oral antibiotic + topical retinoid + BP |
Alternatives for females | See first choice | See first choice | Oral antiandrogen + topical retinoid/azelaic acid ± topical antimicrobial | Oral antiandrogen + topical retinoid/± oral antibiotic ± alt. antimicrobial | High dose oral antiandrogen + topical retinoid ± alt. topical antimicrobial |
Maintenance therapy | Topical retinoid | Topical retinoid ± BP | |||
Postinflammatory hyperpigmentation | 4 % Hydroquinone “Spot Treatment” | 5–10 % Hydroquinone ± Chemical peels, Microdermabrasion, Lasers | |||
Topicals
Retinoids, used as monotherapy and in combination, are the cornerstone of treatment in acne (Table 38.2). It can be especially useful in skin of color as it can help with PIH as well (see below). Large studies including adolescent populations of 12–18 years of age have demonstrated effectiveness and safety of retinoids. Two products are currently FDA approved for patients aged 9–11: tretinoin gel 0.05 % (Atralin®, Coria Laboratories, Fort Worth, TX) for patients ≥ 10 years of age [66] and adapalene/benzoyl peroxide gel 0.1 %/2.5 % (Epiduo®, Galderma Laboratories, Fort Worth, TX) for patients ≥ 9 years of age [67]. However, other retinoids such as adapalene, tretinoin gel, and tretinoin microsphere gel have documented safety in patients less than 12 years of age [35, 38, 68].
Table 38.2
Frequently used topical retinoids and fixed-combination agents
Formulations | Comments | ||
|---|---|---|---|
Retinoids | Tretinoin | ||
Generic | 0.025, 0.05, 0.1 % cream | Pregnancy category C | |
0.01, 0.025 % gel | |||
Atralin® | 0.05 % aqueous gel | Contraindicated with fish allergies [26] | |
(Coria Laboratories, Fort Worth, TX) | |||
Retin-A Micro® (OrthoNeutrogena, Los Angeles, CA) | 0.04, 0.1 % | Microsphere gel or gel pump | |
Tretin-X® | 0.025, 0.05, 0.1 % cream | ||
(Triax Pharmaceuticals, Cranford, NJ) | 0.01, 0.025 % gel | ||
Ziana® | Tretinoin 0.025 % | ||
(Medicis, Scottsdale, AZ) | Clindamycin phosphate 1.2 % gel | ||
Adapalene | |||
Differin® | 0.1 % cream | ||
(Galderma Laboratories, Fort Worth, TX) | 0.1, 0.3 % gel | ||
0.1 % solution | |||
0.1 % lotion | |||
Epiduo® | Adapalene 0.1 % | FDA approved for 9–11 years of age | |
(Galderma Laboratories, Fort Worth, TX) | BP 2.5 % gel | ||
Tazarotene | |||
Tazorac® | 0.05, 0.1 % cream | Second-line treatment in skin of color Pregnancy category X | |
(Allergan, Irvine, CA) | 0.05, 0.1 % gel | ||
Antibiotic and BP | Benzamycin | Erythromycin 3 % | Requires refrigeration |
BP 5 % gel | |||
Benzaclin | Clindamycin 1 % | ||
BP 5 % gel | |||
Duac® | Clindamycin 1 % | ||
(Steifel Laboratories, Coral Gables, FL) | BP 5 % gel | ||
Acanya® | Clindamycin phosphate 1.2 % gel | ||
(Coria Laboratories, Fort Worth, TX) | BP 2.5 % gel | ||
Retinoids normalize follicular epithelium desquamation, preventing microcomedone formation and clearing existing comedones [69]. Some retinoids also have anti-inflammatory effects [70]. Appropriate use involves a pea-size amount to entire face. Emphasize to patients that it is not a spot treatment as there is a tendency to use it as such, resulting in inflammation and PIH. Common side effects include burning, stinging, dryness, and scaling [65]. There is a perception amongst those treating Asians that they may have more sensitive skin and their acne may respond to retinoids slower than Caucasian patients [7]. To improve tolerability, initiate retinoid at the lowest strength, avoid alcohol-based vehicles, encourage moisturizer use, and start with thrice-weekly application and increase to daily as tolerated [31, 38, 71]. Conversely, if patients have oily skin and little risk for irritation, stronger retinoids and gel formulations can be utilized [41]. Adapalene is a distinct second-generation retinoid that is considered well tolerated. It is photostable and can be combined with benzoyl peroxide [72].
Preadolescent and Skin of Color Trials
Although there are no studies to date focusing on preadolescents or children with skin of color in acne, understanding the existing data on preadolescents and attempting extract the data on the skin of color population may provide insight into treatment recommendations. Both efficacy and tolerability are important considerations in this population.
Micronized gel formulations have been used to increase tolerability. In a 12-week open-label study of 40 patients (8–12 years of age) using microsphere tretinoin 0.04 % gel daily, 75 % of participants were graded as mild or clear by the end of 12 weeks [38]. In this study, 62.5 % (25/40) of the patients had skin of color (black, Hispanic, Asian, or combination with white) [38]. Of all the participants, 30 % experienced irritation although it was graded as mild and no one was discontinued from the drug due to irritation. Interestingly, 5 % (n = 2) experienced PIH.
In a randomized, controlled study of microsphere tretinoin gel 0.04 % pump in preadolescents [9–11], there was a significant improvement in noninflammatory lesions in the treatment group versus the vehicle by 12 weeks (−19.9 vs. −9.7, p = 0.04) and overall improvement in the investigator global assessment as well. However, there was no difference in the two investigator global evaluations of acne severity scales: a pediatric scale and standard 5-point FDA scale, which may have been due to the small sample size [39]. Of the 55 patients receiving treatment, 24 were skin of color (African-American—12; Hispanic—10; Asian—2), and in the vehicle group, 17 were skin of color (African-American—8; Hispanic—9; Asian—0) [39]. Although the results were not subdivided by race, there were no statistically significant changes in baseline erythema, dryness, peeling, burning or stinging, or itching between treatment and vehicle by week 12. However, 15 (27.3 %) patients with treatment did cite skin irritation as an adverse effect and four patients on treatment discontinued the trial compared to the one on vehicle.
Adapalene has been shown to be well tolerated in skin of color [71, 73–75]. A meta-analysis of five studies evaluating the safety and efficacy of adapalene use in black patients (Fitzpatrick skin types IV–VI) compared to white patients demonstrated comparable effectiveness. Blacks were less likely to have erythema, scaling, and moderate-to-severe dryness [73]. A randomized, blinded controlled study evaluating the effectiveness and safety of adapalene 0.1 % gel in 200 Japanese patients aged 12–35 (only 2 patients were between the age of 12 and 15 and 16 patients were aged 16–19 years) demonstrated reduction in inflammatory and noninflammatory lesions [71]. Most of the side effects were mild to moderate and noted during the first 2 weeks of treatment, subsiding as treatment continued [71]. A study comparing adapalene gel 0.1 % and tretinoin gel 0.025 % in Chinese patients (n = 139) found adapalene comparable in efficacy but less irritating than tretinoin [76].
Tazarotene is another effective retinoid but is not approved in the United States for children less than 12 years. There is no specific data on tazarotene in adolescents with skin of color. An open-label study on tazarotene 0.1 % gel in Indian patients (n = 126) aged 13–30 showed moderate to complete clearance in 90 % of inflammatory and noninflammatory acne by weeks 8 and 12 [77].
Topical Antimicrobials
Benzoyl peroxide (BP) is an effective and safe treatment for acne in all age groups [78]. Its lipophilic nature allows it to penetrate the stratum corneum and into the pilosebaceous gland where P. acnes are located. It then generates free radicals, oxidizing the proteins in the cell walls of P. acnes. It also has mild comedolytic and anti-inflammatory properties [79, 80]. Other positive qualities of BP include prevention of antibiotic resistance in P. acnes and increased efficacy in combination with retinoids [81, 82]. There have been no reports of P. acnes resistance to BP [83–85].
Side effects of BP include dryness, erythema, and flaking during initiation of treatment. Lower concentrations of BP can decrease irritation without reducing effectiveness [31]. Allergic contact dermatitis can occur in 1/500 people. Complaints of pruritus and eye swelling can be indicators. Patients can conduct a “use test” to distinguish between irritation and allergy [86].
BP formulations range from 2.5 to 10 %. One study demonstrated that treatment of acne on the back may benefit from an increased concentration and longer contact time [87]. BP leave-on products can leave a white film, which can be more apparent in skin of color. Therefore, BP washes may garner improved compliance, though they do require a 20-s contact time to achieve effectiveness. Additionally, washes can reduce the possibility of bleaching clothing, bedding, and towels.
Salicylic acid (SA) is frequently found in over-the-counter acne treatments and is generally well tolerated. It has anti-comedolytic and anti-inflammatory properties. However, in a study comparing SA wash with BP wash, SA was less effective [88].
Topical erythromycin and clindamycin have been used for decades in the treatment of acne and are also generally well tolerated. They are typically used in combination with BP to decrease the development of bacterial resistance. There are rare reports of topical clindamycin associated with pseudomembranous colitis [89, 90]. Topical sulfacetamide is more widely used in rosacea and its odor may limit its use. Patients with sulfa allergies should avoid this product.
Azelaic acid (AA), a dicarboxylic acid produced by Pityrosporum ovale, has antibacterial, anti-inflammatory, and anti-comedogenic properties. Additionally, it has been found to improve PIH (see below). It is formulated in a 15 % gel and 20 % cream. Although well tolerated, mild burning, tingling, and pruritus are not uncommon. Studies have demonstrated its efficacy to be comparable to tretinoin 0.05 % cream, BP 5 % gel, clindamycin 1 %, and erythromycin 2 % ointment [91, 92]. Its efficacy is thought to increase with the combination with a retinoid or BP.
Topical dapsone is a synthetic sulfone that has antimicrobial and anti-inflammatory effects. However its mechanism of action in acne is unknown. Two 12-week randomized, double-blind trials comparing topical dapsone 5 % gel twice daily with vehicle gel in patients aged 12 years and older found a significant reduction in inflammatory and noninflammatory lesions [93]. Initial concerns related to hematologic safety in individuals (≥12 years of age) with glucose-6-phosphate dehydrogenase deficiency were unfounded with application on face, neck, and upper shoulders [94]. However, widespread use over large areas in children aged 6–10 in at-risk populations is cautioned [26]. When dapsone and BP are used together, it can result in a temporary orange discoloration of the skin or hair [31].
Combination Topical Products
Combination topical products can be extremely beneficial for adherence especially in a younger population (Table 38.2). In a post hoc analysis of 2 double-blind, multicenter studies, 1,755 adolescents ranging from 12 to <18 years with moderate-to-severe acne were randomized to receive either a fixed combination of clindamycin phosphate (CP) 1.2 %–benzoyl peroxide (BP) 2.5 % gel, CP 1.2 % alone, BP 2.5 % alone, or vehicle once daily for 12 weeks. There was a statistically significantly reduction in inflammatory and noninflammatory lesions in the CP 1.2 %–BP 2.5 % gel group versus the other 3 groups [95]. When the skin of color group (n = 337) from this study was evaluated, similar lesion count reductions were noted between skin of color and the non-skin of color control [68]. Topical BP 5 %–erythromycin 3 % combination gel has long been available. However it does require refrigeration, which may curtail compliance. One 12-week randomized, placebo-controlled, double-blind trial of 36 patients revealed that CP 1.2 %–tretinoin 0.025 % combination gel in skin types IV–VI had a mild reduction of inflammatory lesions compared to the placebo and no change in PIH. However, it was relatively well tolerated [96].
Most recently, a randomized 12-week study compared preadolescents aged 9–11 using topical adapalene–BP (Epiduo®, Galderma Laboratories, Fort Worth, Texas) (n = 142) to a vehicle (n = 143). It found adapalene–BP was significantly superior to vehicle with regard to treatment success (49.3 % vs. 15.9 %) and percentage of reduction in total lesion count (68.6 % vs. 19.3 %), inflammatory (63.2 vs. 14.3 %), and noninflammatory lesion counts (70.7 % vs. 14.6) all (p <0.001). Overall, it was well tolerated. Only 2 subjects discontinued in the adapalene–BP group due to erythema and skin irritation, both mild in severity [40]. Along with this data and that of 285 patients aged 9–11 years from Galderma, the FDA approved this combination product for use in those 9 years old and older [97].
Oral Antibiotics
Oral antibiotics are very effective in treating moderate-to-severe acne (Table 38.3). It is important to counsel patients that 6–8 weeks of treatment is required to see improvement and the goal is to taper oral antibiotics once disease is diminished. Combination therapy, with topical retinoids and antimicrobials, is required to ensure best results and to decrease the risk of antibiotic resistance. For older children and adolescents, the tetracycline class of antibiotics is most frequently used including doxycycline, minocycline, and tetracycline. Although a mainstay of acne treatment, with the exception of extended-release minocycline, there is no FDA approval for oral antibiotics in acne [98].
Table 38.3
Oral antibiotics used for pediatric acne
Antibiotic | Recommended dosage | Comments/side-effects | |
|---|---|---|---|
Frequently used | Tetracycline | 250–500 mg BID | Dental staining <9 years |
Ingest on empty stomach preferable; dairy products and iron, calcium, or many other metal ions found in vitamins/supplements decrease absorption | |||
GI upset, photosensitivity, teratogenic, PTC, VVC, FDE | |||
Minocycline | 50–100 mg QD-BID | Dental staining <9 years | |
Dairy products decrease absorption | |||
Acute: Vertigo, GI upset (less than doxycycline), teratogenic, PTC, VVC | |||
Chronic: LLS, blue-gray hyperpigmentation, hepatitis | |||
ER 1 mg/kg QD | Lower incidence of vestibular and pigmentation side effects with ER formulations | ||
Doxycycline | 50–100 mg QD-BID | Dental staining <9 years | |
ER 75, 100, 150 mg QD | Can be taken with meals; take with large glass of water and maintain upright position ≥1 h to decrease risk of GI upset | ||
Photosensitivity, photo-onycholysis, teratogenic, PTC, VVC | |||
Erythromycin | 250–500 mg | Antibiotic of choice for children < 8 years of age | |
Erythromycin ethylsuccinate 400 mg/5 mL, 200 mg/5 mL | High prevalence of antibiotic-resistant P. acnes | ||
Less frequently used | Trimethoprim-sulfamethoxazole | 80/400 mg, 160/800 mg BID | Severe drug reactions, bone marrow suppression, hepatitis, GI upset, VVC, FDE |
Do not use as first- or second-line agent for acne | |||
Clindamycin | 75–150 mg BID | Pseudomembranous colitis, GI upset, drug reactions, VVC | |
Cephalexin | 250–500 mg BID | GI upset, drug reactions, VVC | |
125 mg/5 mL, 250 mg/5 mL |
Macrolides
For children under 8 years of age, kids who have not lost their primary teeth, and those with tetracycline allergies, erythromycin and azithromycin can be used in the treatment of acne. Due to the emergence and prevalence of P. acnes resistance to erythromycin, it is not commonly used in older children, except when the tetracyclines are contraindicated [99, 100].
Trimethoprim/Sulfamethoxazole
Trimethoprim/sulfamethoxazole should be used with caution in acne and only in refractory cases due to the risk of severe adverse effects such as Stevens–Johnson syndrome. Data supporting its use in acne are lacking.
Doxycycline
The most common side effects of doxycycline include photosensitivity/phototoxicity and “pill esophagitis” [101–103]. Patients should be instructed to practice good sun protective behaviors. To prevent esophagitis, patients should take doxycycline with food, or with a large glass of water, and remain in an upright position for at least 2 h after ingestion. Enteric-coated doxycycline is an alternative form if needed.
Minocycline
Minocycline has less potential for photosensitivity and gastrointestinal discomfort and is frequently used in the management of adolescent acne. Rare and serious side effects should be discussed with patients. Vestibular toxicity, drug hypersensitivity (DHS), and serum sickness-like reaction can occur within days to weeks of initiating the drug. Vestibular toxicity presents with vertigo and/or dizziness and resolves with discontinuation of minocycline [104–106]. DHS usually presents within the first 8 weeks of treatment with flu-like symptoms, diffuse erythema, facial edema, cervical lymphadenopathy, and transaminitis. There may be interstitial inflammation of other organs as well [107, 108].
Conversely, lupus-like syndrome (LLS) and hyperpigmentation tend to occur after chronic use of minocycline (months to years). LLS presents with malaise, distal polyarthralgias with or without polyarthritis, and rarely autoimmune hepatitis. The autoimmune antibody profile can be variable. Antinuclear antibodies are usually present, p-ANCA strongly supports the diagnosis, and anti-histone antibodies are not required for diagnosis [31]. Cutaneous and mucosal blue-gray hyperpigmentation can occur in areas of scarring, on the shins, oral mucosa, sclera, and nail beds. Risk is associated with a cumulative exposure [109–111].
Hormonal
Hormonal treatments in acne can be divided into four groups: (1) androgen receptor blockers, (2) ovarian androgen blockers, (3) adrenal androgen production blockers, and (4) enzyme inhibitors. The two most commonly used agents in the United States include spironolactone (androgen receptor blocker) and combined oral contraceptives (COCs) (ovarian androgen blockers). Hormonal treatments should be considered especially in patients who complain of acne in the mandible region, chin, and neck.
Spironolactone is a steroid androgen receptor blocker and can be very helpful in adult female pattern acne [114–117]. It competes with testosterone and dihydrotestosterone (DHT) for androgen receptors on sebaceous glands and reduces the sebocyte proliferation [118]. Its use in pediatric patients may be limited as there is minimal data on its role in adolescent acne and appropriate age of initiation.
COCs can be very effective in treating the hormonal component of acne. COCs contain an estrogen, ethinyl estradiol, and a varying progestin. The estrogen inhibits LH and FSH, which suppress ovulation and ovarian androgen production. This subsequent reduction in androgens results in a decreased activation of androgen receptors at the level of the sebaceous gland. Estrogen also stimulates the production of steroid hormone binding globulin (SHBG) in the liver, which decreases circulating levels of testosterone.
COCs are rarely used as monotherapy for acne. In most instances, patients are already on a combination therapy of topical retinoids, topical BP, and antibiotics. There are several situations where the addition of COCs is appropriate: (1) girls who desire regulation of their menstrual cycle; (2) inadequate response to treatment; (3) acne flares corresponding with menstrual cycles; (4) complaints of oiliness; and (5) contemplation of isotretinoin therapy [119]. Younger patients and parents can initially present with reluctance and anxiety at the suggestion of starting COCs. Emphasizing the hormonal component in the pathophysiology may reduce discomfort. It can also be presented as a stepwise approach to isotretinoin therapy.
There are currently three FDA-approved COCs for the treatment of acne: ethinyl estradiol/norgestimate (Ortho Tri-cylen®, McNeil Janssen Pharmaceuticals, Raritan, NJ) for females ≥ 15 years of age, ethinyl estradiol/norethindrone (Estrostep®, Warner-Chilcott, Rockaway, NJ) for females ≥ 15 years of age, and most recently, ethinyl estradiol/drospirenone (Yaz®, Bayer, Montville, NJ) for females ≤ 14 years of age.
As stated by American College of Obstetricians and Gynecologists (ACOG), pelvic exams are not required prior to oral contraceptive initiation in teenagers. Most recently, ACOG guidelines recommend less frequent cervical screening in general: 3 years after onset of sexual activity or at the age of 21. The decision to prescribe COCs is not determined by the pelvic exam findings. COCs can be safely prescribed based on careful review of medical history and blood pressure evaluation [120, 121]. While routine well-women exams are advocated, it is acceptable to start COCs with future follow-up with a gynecologist or primary care physician.
Although the risk of thromboembolic events is lower in adolescents, a careful family history is required and smoking is strongly discouraged. Patients are instructed to take their oral contraceptives daily, at approximately the same time each day. Irregular use impedes treatment; in addition, patients may experience unscheduled bleeding and a false sense of contraception security. Patients are encouraged to set an alarm on their cellular devices as a daily reminder to routinely take their pill. If the daily pill is forgotten or missed, patients should take the missed pill as soon as they realize. If one whole day is missed, the patient should take both pills at the same time [119].
Initial bleeding or spotting is normal during the first 3 months of treatment and should resolve after the body adjusts to the new hormonal levels. Other common side effects include nausea, vomiting, weight gain, mood changes, and breast tenderness. Weight gain is often a cited barrier to treatment. However, a recent Cochrane review indicated no large effect of COCs on weight gain, although the current evidence was not adequate [122]. In teenage patients, it is especially important to mention that COCs do not protect against sexually transmitted infections (STIs). If a patient is using COCs for treatment of acne and contraception, they should be evaluated regularly by a primary care provider for STI counseling and surveillance. Monitoring blood pressure for several months after starting COCs should also be done at follow-up visits as they may cause hypertension [123].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


