Head and Neck Masses
David E. Tunkel and Jonathan A. Perkins
Head and neck masses commonly occur in young children, and the differential diagnosis for such masses is broad. The initial history and physical examination usually provides sufficient information to narrow the possible causes of a swelling in a child’s head or neck. This should direct the subsequent evaluation and initial therapy. While the majority of these head and neck masses are inflammatory in nature, congenital abnormalities and neoplasms can occur and often require surgical intervention for diagnosis and treatment. In one review of children with head and neck masses that were biopsied or excised, 55% had congenital lesions, 27% had inflammatory masses, and 14% had a benign or malignant neoplasm.1 A thorough evaluation of a child with a head and neck mass is necessary to prevent delay in diagnosing a malignancy and to allow appropriate medical or surgical treatment of persistent benign diseases.
AGE CONSIDERATIONS IN DIFFERENTIAL DIAGNOSIS
Neonates and young infants who present with neck masses at or close to the time of birth most likely have congenital abnormalities such as branchial cleft cysts, thyroglossal duct cysts, or vascular malformations (see Chapter 372). Infants can also develop infectious neck masses, including abscesses that usually occur from suppuration of lymph nodes. Neck abscesses in infants can occur throughout the neck (Fig. 373-1) and are usually caused by Staphylococcus aureus.2 These abscesses are treated with appropriate antibiotic therapy (with the increasing frequency of methicillin-resistant Staphylococcus aureus in mind) and with surgical drainage when necessary.3 A neck mass that appears in the first several weeks of life is fibromatosis coli, also called sternomastoid tumor of infancy, which presents with a firm lateral neck swelling and is often associated with a head turn or tilt (Fig. 373-2). Both parents and primary care physicians often have concerns of potential malignancy with this presentation. The diagnosis is a clinical one, supported by ultrasonographic findings of a solid mass within the sternomastoid muscle, and resolution is expected in almost all infants.4 The most common malignancies that present as neck masses in infants are blue-cell tumors, which include neuroblastoma, rhabdomyosarcoma, and lymphoma (see discussion of malignant neoplasms below).
Neck masses in preschool children usually are inflammatory in nature, and transient lymphadenopathy can occur commonly in association with other infectious symptoms. Congenital neck masses may first present at this age, when a quiescent congenital cyst enlarges as a result of infection. Nontuberculous mycobacterial adenitis occurs primarily in this age group, usually presenting as a mass in the submandibular, parotid, or upper neck areas that eventually causes skin discoloration or fistula formation.5 Surgery is the primary treatment for this localized infection.
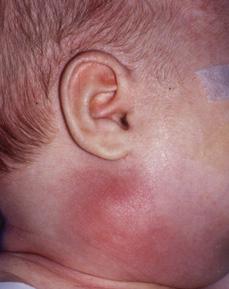
Figure 373-1. Suppurative adenitis/neck abscess in an 8-month-old child.
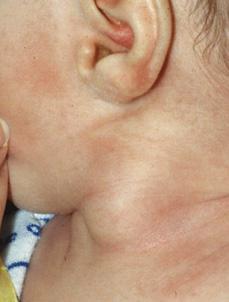
Figure 373-2. Firm swelling within the sterno-mastoid muscle in a 4-week-old child with sterno-mastoid tumor of infancy (fibromatosis coli).
Older children and adolescents with neck masses usually have enlarged cervical lymph nodes as a reactive process that is secondary to viral or bacterial infection. However, children in this age group can have malignant tumors such as lymphoma or carcinomas of the thyroid or salivary glands, and consultation for possible tissue diagnosis should be sought in patients with other associated symptoms, a mass that is enlarging, and persistent swelling.6 African American teenagers have an increased risk of nasopharyngeal carcinoma, a disease that often presents with metastatic disease in the neck before the nasopharyngeal primary is detected.7
DIAGNOSTIC EVALUATION
The initial focused history should assess the lesion’s time of onset and duration, the rate of growth, and the presence of associated systemic symptoms such as fever, weight loss, and cough. Information about environmental exposures, including exposure to cats, HIV, tuberculosis, or radiation, should be obtained.
The examination should focus on the location, size, and consistency of the mass(es), and whether the mass seems tender. Discoloration, fixation, or necrosis of the overlying skin should be noted. Supraclavicular and posterior triangle masses in children have a higher incidence of malignancy.8
Laboratory studies should be directed based on the findings of the history and examination. A complete blood count and C-reactive protein may be helpful in assessing acute inflammatory processes in the neck. Tuberculin skin testing or Quantiferon TB blood testing should be used when mycobacterial infection is suspected. Specific serological tests, such as Epstein-Barr virus antibody titers or Bartonella henselae (“cat-scratch” disease) titers, may be helpful when these diseases are suspected clinically.
Imaging studies are useful in confirming diagnoses and detailing anatomy for subsequent surgical intervention. Ultrasonography is most helpful for confirming the diagnosis of sterno-mastoid tumor of infancy and for assessing the presence of normal thyroid gland in children with suspected thyroglossal duct cysts.9 Computerized tomography, almost always done with intravenous contrast administration, is useful for delineating the anatomy of most pediatric neck masses and for diagnosing neck abscesses (eFig. 373.1  ). Magnetic resonance imaging (MRI), with or without magnetic resonance angiography, is the preferred method for diagnosing suspected vascular lesions or masses that may involve the central nervous system (eFig. 373.2
). Magnetic resonance imaging (MRI), with or without magnetic resonance angiography, is the preferred method for diagnosing suspected vascular lesions or masses that may involve the central nervous system (eFig. 373.2  ). MRI also allows soft-tissue imaging without ionizing radiation, an advantage that has become more significant recently with published concerns about the potential oncogenic effects of radiographic imaging.10
). MRI also allows soft-tissue imaging without ionizing radiation, an advantage that has become more significant recently with published concerns about the potential oncogenic effects of radiographic imaging.10
INDICATIONS FOR SURGICAL INTERVENTION
Surgery for neck masses in children can be divided into incisional or excisional biopsy for diagnosis, excision of masses for treatment, and drainage or debridement of infectious masses/abscesses. While many neck masses in children are transient and will respond to medical therapy, persistent masses without obvious diagnosis should be evaluated for biopsy. Fine-needle aspiration biopsy can provide specimens for culture and cytopathology, but the frequency of nonepithelial neoplasms in children often requires open surgical biopsy for definitive diagnosis.11
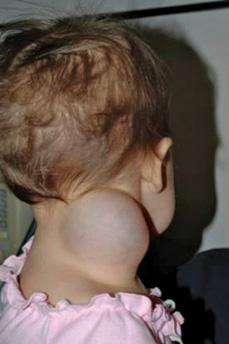
Large neck masses, such as lymphatic malformations, in young children may be unsightly and may cause compressive symptoms, including airway obstruction (Fig. 373-3). These masses may require surgical intervention to avoid airway compromise. Congenital neck cysts and sinuses are usually excised to avoid the risk of subsequent infection or enlargement.
Surgical drainage of pediatric neck abscesses should be considered when the abscesses are large, the child is toxic, or when response to antibiotic therapy is not prompt. Small abscesses or areas of cellulitis may respond to medical therapy. Drainage also allows culture of the abscess material, which is particularly useful when resistant organisms are suspected. In children with chronic lymphadenitis, as seen with nontuberculous mycobacterial infection, debridement and curettage will provide tissue for pathological diagnosis and cultures and may cure many cases.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


