Haemophilus influenzae
Mark R. Schleiss and Arnold L. Smith
Although the types of infectious diseases caused by Haemophilus influenzae have changed considerably in recent years as a result of the widespread implementation of routine childhood immunization against type b organisms, this organism remains an important pathogen. There are two major categories of H influenzae: unencapsulated strains (untypeable, NTHi) and encapsulated strains (typeable). The unencapsulated strains are responsible chiefly for infections at mucosal surfaces, including conjunctivitis, otitis media, sinusitis, and bronchitis. In contrast, one of the six antigenically distinct encapsulated strains, strain type b, is associated with most invasive diseases such as septicemia, meningitis, cellulitis, septic arthritis, epiglottitis, and pneumonia. Prior to the availability of an effective vaccine, H influenzae type b (Hib) was the most common cause of pediatric bacterial meningitis in the United States.
 EPIDEMIOLOGY
EPIDEMIOLOGY
Humans are the only natural host for H influenzae. Maintenance of the organism in the human population depends on person-to-person transmission, which appears to occur by the respiratory tract to hand to respiratory tract route. This mode of transmission was best documented during nosocomial outbreaks of NTHi pneumonia in the elderly. Nontypeable strains colonize the upper respiratory tract of as many as 75% of healthy adults. Type b H influenzae (Hib) strains colonize the nasopharynx of children at a rate of 3% to 5%; the effectiveness of the conjugate vaccines is related (in part) to their ability to diminish the incidence of nasopharyngeal colonization (see below). Although both nontypeable and type b strains of H influenzae are easily spread via person-to-person transmission, only the Hib strains have historically been associated with invasive disease in children. Nasopharyngeal colonization by Hib is for the most part asymptomatic, but breakthrough bacteremia with subsequent development of focal infection was at one time a common occurrence and a major pediatric public health problem in the United States.
In the prevaccine era, invasive Hib disease characteristically had a striking age-related incidence, with approximately 85% of disease occurring in children younger than 5 years. The peak incidence of the most serious form of invasive disease, meningitis, occurred between 6 and 12 months of age. Hib epiglottitis was, in contrast, predominantly a disease of older children, with more than 80% of the infections occurring in children older than 2 years. In the prevaccine era, approximately 20,000 instances of invasive Hib disease occurred annually in the United States, affecting about 1 in 200 children younger than 5 years.1
Chronic illnesses associated with increased risk for invasive Hib disease include sickle cell disease, asplenia, agammaglobulinemia, trisomy 21, Hodgkin disease, and complement deficiencies. Increased risk has also been associated with childcare attendance, the presence of siblings younger than 5 years, household crowding, lower socioeconomic status, and passive smoke exposure. Breast-feeding confers some protection against disease. A bimodal seasonal disease pattern has been described, with one peak of illness in the autumn between September and December, and a second peak in the spring between March and May.2 Although invasive Hib infection has historically been uncommon in adults, apparently due to the gradual development of protective antibodies over time in the context of asymptomatic nasopharyngeal colonization, Hib can occasionally cause invasive infection in adult patients. 
The epidemiology of invasive Hib disease has changed dramatically in recent years as a consequence of the widespread administration of conjugate vaccines.
In populations with high rates of vaccine coverage, the incidence of Hib disease has been reduced by more than 95%.1 The protective efficacy of these vaccines exceeded initial expectations because of an unanticipated decrease in nasopharyngeal carriage, ultimately leading to a decreased environmental burden of Hib and a resultant protection even of unimmunized children, an effect of “herd immunity.” The conjugate vaccines are so effective in preventing Hib infection that the finding of invasive disease in a fully immunized child should prompt further diagnostic evaluation for the possibility of an underlying immunodeficiency. 
An important aspect of Hib epidemiology is the risk it poses to contacts. Although the direct contagiousness of invasive Hib infection is limited, a significant risk for secondary disease exists among household contacts of a patient with invasive Hib disease, particularly in the 30 days following exposure to an index patient. This is a consequence of spread under conditions of continuous household exposure. Colonization rates higher than 70% have been noted following exposure in closed populations, such as within families or in daycare centers. This becomes the rationale for chemoprophylaxis following exposure to an invasive case of Hib disease (see below).
Another less common but recently recognized route of acquisition of H influenzae is vertical transmission via the birth canal. This phenomenon has been manifest in recent years as a “typical” cause of early onset pneumonia. These NTHi can cause neonatal bacteremia and meningitis after acquisition from the genital tract. These strains are genetically distinct from those colonizing the upper respiratory tract and are occasionally a cause of neonatal conjunctivitis.6
 MICROBIOLOGY
MICROBIOLOGY
H influenzae is a small gram-negative coccobacillus that may show considerable microscopic pleomorphism, necessitating careful and cautious interpretation of Gram stains of clinical specimens (Fig. 263-1). Biochemical identification of H influenzae is based on the demonstration that growth on rich media (blood agar) is dependent on supplements, factors X and V, as found in chocolate agar.  The growth of H influenzae is fastidious, and the viability of the organism is lost rapidly, necessitating expeditious handling of clinical specimens.
The growth of H influenzae is fastidious, and the viability of the organism is lost rapidly, necessitating expeditious handling of clinical specimens.
The polysaccharide capsule of H influenzae has a central role in the virulence of invasive H influenzae. Six antigenically and biochemically distinct capsular polysaccharide subtypes (a-f) have been identified. Although type b encapsulated strains have historically been of primary clinical and immunologic importance (because of the association with invasive infection, including meningitis), the other encapsulated strains are also capable of producing invasive disease.
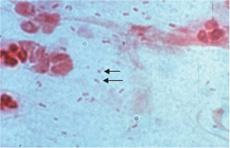
FIGURE 263-1. Gram stain of Haemophilus influenzae. Arrows point to two small “cocco-bacillary” gram-negative rods. (Provider: Professor Shirley Lowe, University of California, San Francisco School of Medicine. With permission.)
Plasmid-mediated ampicillin resistance due to production of β-lactamase has become extremely common in Hib and NTHi, ranging from 5% to 50% of isolates in various parts of the world. Non-β-lactamase–mediated ampicillin resistance is increasing in the United States; thus, susceptibility testing should be performed on all isolates identified in invasive infections.8
 IMMUNITY
IMMUNITY
Age-dependent susceptibility to Hib infections correlates with an age-dependent nature of immune response to Hib surface components. The bactericidal activity of children and adults against Hib and certain NTHi is directed against LPS and outer membrane proteins. Even after recovery from an invasive Hib illness, anticapsular antibody levels in infants remain low. As a consequence, instances of second or third episodes of invasive Hib disease are well described; thus, a previous episode of invasive infection does not obviate the need for Hib immunization. This failure to make serum anti-PRP antibodies is typical of the natural delay in immune response of infants to polysaccharide antigens. PRP stimulates B cells but does not adequately activate macrophages and appropriate T-helper cells, and therefore it is considered to be a T-cell-independent antigen. The characteristics of T-cell-independent antigens include limited immune responses, particularly in young infants; no booster response occurs with repeated antigenic stimulation, and production of antibody that is of low affinity and mostly consisting of IgM. The development of a Hib vaccine that was more immunogenic and protective for young infants required conversion of PRP from a T-cell-independent antigen to a T-cell-dependent antigen, using the principles of carrier-hapten linkage.10
 CLINICAL MANIFESTATIONS OF DISEASE CAUSED BY TYPABLE STRAINS
CLINICAL MANIFESTATIONS OF DISEASE CAUSED BY TYPABLE STRAINS
Meningitis
Prior to Hib conjugate vaccines, meningitis was the most common and serious manifestation of invasive Hib disease. The differential diagnosis and clinical manifestations of meningitis are detailed in Chapter 231. The sequelae from Hib meningitis differ from other causes of bacterial meningitis. Approximately 30% of children will have seizures at some point in the course of Hib meningitis. Like patients with meningococcal disease, children with Hib bacteremia can have a petechial rash. They can also have a secondary site of infection, such as a septic arthritis or facial cellulitis (see below). Shock is present in approximately 20% of cases. Anemia is common, the result of a combination of accelerated red blood cell destruction and diminished erythropoiesis. Complications of H influenzae type b meningitis include subdural effusion or empyema, ischemic or hemorrhagic cortical infarction, cerebritis, ventriculitis, intracerebral abscess, and hydrocephalus. Intravenous antibiotics and supportive care are the mainstays of therapy, but the mortality from Hib meningitis remains approximately 5%, even with prompt diagnosis. Long-term sequelae occur in 15% to 30% of survivors and are manifest as sensorineural hearing loss, language disorders, mental retardation, and developmental disorders. A meta-analyses of randomized controlled clinical trials in children has shown that the incidence of severe hearing loss due to H influenzae was decreased by the administration of corticosteroids, an effect that was more evident in children in high-income countries.11
Epiglottitis
Acute upper airway obstruction caused by Hib infection of the epiglottis and supraglottic tissues is perhaps the most dramatic and rapidly progressive form of disease caused by this organism. In contrast to the peak incidence of meningitis in children younger than 1 year, epiglottitis occurs primarily in older children (2–7 years of age) and usually has an abrupt onset with high fever, dysphagia, drooling, and toxicity. Occasional cases of Hib epiglottitis are still observed in older children who were never fully immunized, and Hib is also an important cause of epiglottitis in adult patients.
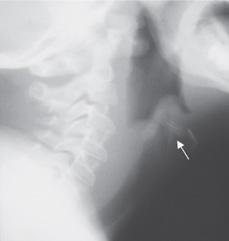
Classically, the child with Hib epiglottitis will drool because of an inability to swallow oropharyngeal secretions. Progressive respiratory distress develops over a period of hours with tachypnea, stridor, cyanosis, and retractions. The patient may sit forward with the chin extended to maintain an open airway (“tripod” position). Few conditions produce such a striking constellation of symptoms and findings. A lateral neck radiograph is helpful if the clinical presentation is subtle, but the study should be performed cautiously and without undue delays, with a physician experienced in airway management in attendance (Fig. 263-2). Diagnostic studies should not delay the need for direct inspection of the epiglottis in the operating room and insertion of an endotracheal tube (Fig. 263-3). The mortality rate is 5% to 10% and is invariably related to poor control of the airway early in illness.
Septic Arthritis/Osteomyelitis
In the prevaccine era, Hib was the leading cause of septic arthritis in children younger than 2 years. Approximately 8% of H influenzae invasive disease presents as septic arthritis, typically affecting large joints, particularly knees, ankles, hips, or elbows. A contiguous osteomyelitis may be present, but isolated osteomyelitis without an adjacent septic joint is uncommon. Characteristically, there is a preceding nonspecific illness, followed by pain, swelling, and erythema of the involved joint. Clinical signs in children with a septic hip may be less prominent than for other joints, with findings limited to decreased range of motion of the joint, often with the leg abducted at the hip and externally rotated. In some cases, pain is referred from the hip to the lower leg. Septic arthritis of the hip joint requires surgical drainage; the majority of cases involving the shoulder also require open drainage. There is a strong association of septic arthritis with meningitis, necessitating lumbar puncture in these patients.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


