Disorders of the Upper Extremity
Marybeth Ezaki
This brief section is meant to cover the upper extremity conditions that are commonly seen or are important for timely diagnoses and treatment or referral. This section is not meant to be comprehensive or inclusive of all upper extremity conditions that may be seen, but rather is a brief overview of conditions that every pediatric resident and practicing pediatrician should know about. A “triage” list is provided along with a list of references at the end of the section.
EMERGENCY CONDITIONS
 TRAUMA
TRAUMA
Physical examination of the hand injured by trauma is critical to determine if tendons or nerves have been damaged. Assess the active range of motion of the fingers distal to the injury as well as directly inspect the depths of the wound for partial or complete tendon injuries. Assess sensation in all fingers, and assess function of the intrinsic muscles in the hand, while inspecting the wound for evidence of nerve injury. The presence of arterial injury makes the possibility of nerve injury much higher.1
If an injury is confirmed or suspected, refer the patient to a hand surgeon.
All open wounds should be gently cleansed and assessed for nerve, vessel, and tendon injury. If bleeding cannot be adequately controlled by direct pressure or if the distal circulation has been compromised, the patient should be referred to an emergency department for further evaluation. Open wounds should never be clamped to control bleeding. If sensation is normal in all fingers, and tendon function intact, the wound can be closed and the entire forearm and hand splinted to allow the wound to heal. If there are deficits in tendon or nerve function, follow-up evaluation and definitive treatment by a hand surgeon should be arranged within the next 5 to 7 days.
It is important to note that some finer amputations do not have to go to the emergency department when they occur. If no bone is exposed, the finger wound can be gently cleansed and then covered with a nonadherent dressing (telfa, adaptic, xeroform gauze, petrolatum gauze, etc). Fluffed gauze can then be put between all the fingers and then over the injured finger that can then be wrapped with cast padding, followed by a short or long arm cast, and examined subsequently by an orthopedic hand surgeon for further care. If a child is under 5 years, a long arm cast with the elbow bent to 90° is preferred. For a child older than age 5 years, a short arm cast is appropriate. The wound will heal by secondary intention, and after approximately 3 weeks in a cast, most of these minor injuries will be healed and pain free. If bone is exposed or if the nail plate has been pulled out of the eponychial fold (otherwise known as an open Seymour physeal fracture), the patient with this injury would need to be referred to the emergency department for urgent care.
 BITE WOUNDS
BITE WOUNDS
Superficial dog and cat bites from domestic animals should be cleansed and dressed and appropriate antibiotics administered. The most common organisms that can cause an infection from a bite are staphylococcal and streptococcal species, but for cat bites, coverage for Eikenella corrodens should be added (Chapters 122 and 367). Snake bites with envenomation require emergency evaluation in the emergency department and may require antivenom or surgical debridement. Spider bites are rarely life threatening, but local reaction may require individualized treatment. Human bites that penetrate fascial and synovial spaces in the hand require surgical debridement and aggressive antibiotic care.
 PAINT GUN AND INJECTION INJURIES
PAINT GUN AND INJECTION INJURIES
High-pressure injection injuries from paint guns or water pressure nozzles are surgical emergencies. The injected substance travels along tissue planes and, depending on the material injected, can result in chemical necrosis, tissue destruction, and proximal spread of infective material. Compartment syndrome is probable. These types of injuries require emergent surgical care.
 FRACTURES (See Chapter 218)
FRACTURES (See Chapter 218)
An acutely displaced fracture is not difficult to diagnose and requires urgent care. The nondis-placed closed fracture without neurological or vascular deficit can be splinted and referred in the next 24 to 48 hours to the orthopedist for semiurgent evaluation and definitive care. Open fractures constitute an emergency and require surgical debridement and definitive fracture care.2
A compartment syndrome is a true emergency. Any condition that leads to an increase in the pressure within a muscular compartment that exceeds the perfusion pressure results in ischemia and impending tissue death, so urgent medical care should be sought as soon as possible. Common causes for compartment syndrome include direct vessel injury, kinking or spasm of a vessel due to fracture, bleeding into the compartment and resultant swelling from blunt or open trauma, bleeding associated with a coagulopathy, and prolonged entrapment of the hand or forearm in a tight space. Clinical findings should be recognized by all physicians and include pain out of proportion to the associated condition, increased pain on stretch of the muscles involved (usually the finger flexors), and fullness or hardness of the muscle compartment. If the compartment syndrome is unrelieved, loss of sensation, and paralysis of muscles occurs because of nerve ischemia.
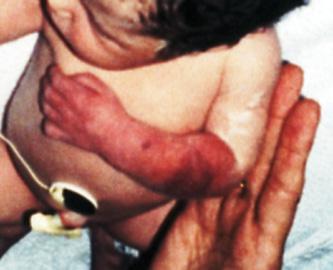
FIGURE 217-1. The appearance of the forearm with a neonatal compartment syndrome. Note the sentinel lesion and the discoloration.
A rare but devastating variant of compartment syndrome occurs in the neonate. It develops during the immediate antepartum period, but the exact etiology is unknown. Intrinsic thrombophilic mechanisms as well as extrinsic compression have both been implicated. The neonate presents in the delivery room with a swollen, paralyzed, dysvascular limb. There is typically a sentinel bullous or open lesion on the forearm (Fig. 217-1).
Ischemia as a result of a compartment syndrome that lasts more than several hours results in muscle necrosis, hemoglobinuria, and permanent functional loss of the limb. The only treatment that may salvage some function is emergency surgical fasciotomy.
 INFECTION
INFECTION
Infections in children’s hands are not common, but early diagnosis and appropriate treatment should be part of primary care practices. The most common infections are bacterial and result from direct inoculation by a puncture wound or minor trauma. A paronychia is an infection of the paronychium, or the cuticle and delicate superficial tissue around the base of the fingernail. Warm soaks, elevation, and gently pushing the cuticle back will often resolve these minor infections. Oral antibiotics may hasten the resolution of a paronychia. A felon by contrast is an infection in the closed space of the pulp of the fingertip and usually requires surgical drainage. Deep infections that involve synovial-lined spaces, bones, or joints require emergency surgical care. Any child with a swollen tender hand, fever, and systemic signs of sepsis such as blood pressure instability or a rapid heart or respiratory rate should be referred emergently to a hand surgeon or hospital.
Herpetic whitlow is a relatively common infection in children, especially a child who sucks a thumb or finger. This infection is recognized by the absence of swelling, but either vesicles or pustules on a red base. Oral lesions are often present. Treatment is symptomatic and time limited, although a primary infection may benefit from use of acyclovir.
Chronic swelling of joints or tendon sheaths may be indicative of unusual infectious or inflammatory conditions. The differential diagnosis should include atypical mycobacterial infections, juvenile chronic arthritis, and psoriatic arthritis. Being able to culture the organism is most helpful in diagnosing the particular organism causing an infection in the hand or arm.
SUBACUTE OR SEMIURGENT CONDITIONS
 NEONATAL BRACHIAL PLEXUS PALSY
NEONATAL BRACHIAL PLEXUS PALSY
Stretch injury to the brachial plexus is a common condition following the birth of a large baby. The diagnostic findings are diminished or asymmetric motion of the involved upper extremity in the neonate. Initial treatment is to protect the limb and support for comfort. Most of these birth palsies will recover spontaneously in the first several weeks. Treatment of these injuries is evolving, and there is not yet consensus as to the optimal timing or nature of treatment. If recovery is not complete by age 2 months, the infant should be referred to a team of specialists who can deal with early physical therapy, neurological evaluation, musculoskeletal care, and decision making regarding appropriateness of direct surgical intervention in the brachial plexus. Decisions about appropriate treatment are made after a period of observation.3
 AMNION DISRUPTION SEQUENCE WITH IMPENDING TISSUE LOSS
AMNION DISRUPTION SEQUENCE WITH IMPENDING TISSUE LOSS
Amnion disruption sequence (amniotic band syndrome, constriction band syndrome) typically presents with fenestrated syndactyly, finger amputations and tissue loss, distal edema, and constriction bands. Rarely, a band may entwine a finger or limb and cause increasing edema and impending tissue loss in the early newborn period. Immediate surgical release of the encircling bands may salvage the endangered part.3
CHRONIC OR ELECTIVE CONDITIONS
 CONGENITAL ANOMALIES
CONGENITAL ANOMALIES
In general, there is rarely an indication for early surgery if congenital anomalies of the upper extremity are noted at birth, even though they can be quite distressing to the parents, who want immediate answers and reassurance about their infant. Most care for congenital conditions is nonoperative, and reconstructive procedures are postponed until anesthetic risk is lessened after approximately age 7 to 8 months of age. Larger size and maturation of airway and critical organ systems makes surgical care more predictable.4
Certain conditions necessitate a search for related conditions. These include, in particular, the spectrum of “radial dysplasia.” Recognition of a small thumb or other elements of radial dysplasia require evaluation of the cardiac, spinal, renal, and hematological systems. The hand anomaly may be the presenting finding in VACTERRL association, (Chapters 176 or 179) Fanconi’s anemia, thrombocytopenia absent radius (TAR) syndrome (see Chapter 176), and other conditions.
Other congenital conditions such as syndactyly, polydactyly with broad connection to the hand, and major morphologic limb malformation can be referred to a hand surgeon at 3 to 6 months of age. The postaxial polydactyly with a small, pedunculated base can be tied off or ligaclipped by the primary pediatrician. If the base is too wide, surgical care is best delayed until the child is 1 year of age.4
Trigger thumbs and fingers are mislabeled as truly being congenital because most occur in infancy and early childhood, and some will spontaneously resolve. A trigger thumb appears as a flexed distal joint of the thumb, usually locked in flexion. There is a characteristic nodule at the flexor aspect of the metacarpophalangeal joint. There is no need for radiographs or other imaging with this condition. Treatment is by surgical release if the deformity is bothersome and still present by age 3. Trigger fingers are more complicated than trigger thumbs and require surgical care as well. There is no place for corticosteroid injection in the treatment of trigger thumbs or trigger fingers.
Congenital contractures and angled digits should be referred for diagnosis, splinting, and treatment. The hand deformity may be the presenting complaint in a number of conditions, including the myriad forms of arthrogryposis.
Oligodactyly, or too few fingers, and missing parts of fingers are common congenital upper limb malformations. Few of these are related to amnion disruption sequence. The most common diagnosis is symbrachydactyly, which has a broad spectrum of presentation. Other diagnoses include ulnar dysplasia and clefting syndromes. Referral for diagnosis and treatment can be delayed until after 3 to 6 months of age.
Table 217-1. Triage Classification of Upper Extremity Emergencies



