Disorders of the Neck and Spine
Daniel J. Sucato
CONGENITAL MUSCULAR TORTICOLLIS
Torticollis refers to lateral tilt and rotation of the head and neck. The most common form of torticollis is known as congenital muscular torticollis and is due to “over pull” of the sternocleidomastoid muscle to the side of head tilt. So, for example, a right-sided sternocleidomastoid muscle contracture would result in head tilt to the right and rotation of the chin to the left (Fig. 216-1). This deformity is seen at birth and is often associated with a very tight sternocleidomastoid muscle (SCM) that often has a small mass or swelling in its midsubstance which is palpable but not painful. The incidence of congenital muscular torticollis is 3 to 5 per 1000 births. The etiology is not completely understood but is associated with breech presentation and difficult forceps delivery and occurs more commonly in first-born children. It is important to remember that this is a painless torticollis. Other associated orthopedic conditions are associated with torticollis including hip dysplasia and metatarsus adductus. These conditions should be evaluated as part of the normal orthopedic examination with specific focus placed on the examination of the hips and feet, as well as the spine in patients with muscular torticollis.1
The clinical presentation typically demonstrates a predisposition to tilting the head to one side with rotation to the opposite side. A small mass in the midportion of the sterno-cleidomastoid is palpable on the affected sternocleidomastoid muscle and has the feel and size of an olive. The face on the ipsilateral side of the SCM lesion demonstrates some flattening with loss of roundness of the back of the head (plagiocephaly) on the opposite side.
The differential diagnosis of congenital muscular torticollis includes congenital cervical vertebral anomalies, inflammatory atlantoaxial rotatory displacement, central nervous system (CNS) tumors of the posterior fossa or cervical spinal cord, or visual abnormalities. When the sternocleidomastoid is contracted with the palpable olive with a consistent head tilt to the ipsi-lateral side with rotation to the opposite side, the diagnosis is nearly confirmed. Treatment consists of stretching exercises to rotate the infant’s chin to the ipsilateral shoulder, while tilting the head toward the contralateral shoulder. This should be performed several times during the day and generally results in outstanding correction of this deformity over a 6 to 12 month period of time. Other modalities such as positioning the child in their crib so as to look at objects opposite to his or her restricted motion are appropriate. Early nonoperative treatment is usually successful with restoration of full motion.
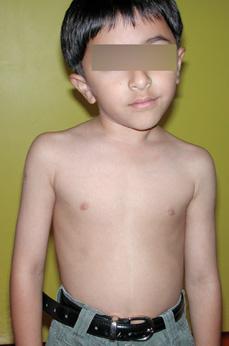
FIGURE 216-1. Congenital muscular torticollis in a young boy. The tight right sternocleidomastoid causes the right head tilt and rotation to the left.
The plagiocephaly seen with congenital muscular torticollis is due in large part to the abnormal head tilt and rotation, as well as the supine position that has been recommended by the American Academy of Pediatrics of 1992. It is exceptionally uncommon for this plagiocephaly to result in facial asymmetry requiring any type of treatment. In general, as the torticollis improves, plagiocephaly improves because asymmetric pressure is alleviated with treatment. There is some evidence that use of an orthotic helmet improves this plagiocephaly; however, well-controlled studies seem to be lacking. Surgical treatment for congenital muscular torticollis is uncommon, if aggressive physical therapy is begun early. Surgical treatment requires lengthening of both the proximal and distal ends of the sternocleidomastoid to improve the position of the head and generally results in improved head positioning but does not generally result in completely normal range of motion treatment.
KLIPPEL-FEIL SYNDROME
Klippel-Feil syndrome presents as a spectrum of congenital fusions or failure of formation of the cervical vertebrae. Klippel-Feil syndrome is defined as the triad of a short, webbed neck, combined with low posterior hairline and fusions in the cervical spine. It is important to recognize Klippel-Feil syndrome because neck mobility is limited and may predispose the patient to a cervical spine injury with some traumatic event. In addition, Klippel-Feil syndrome can be associated with an elevated scapula (Sprengel’s deformity), which should be recognized at the time of the evaluation. Finally, scoliosis below the cervical spine either due to congenital abnormalities in the thoracic or lumbar region or associated compensatory curves below the cervical congenital scoliosis can be seen. Sprengel’s deformity is seen in up to 50% and scoliosis is seen in 30% of patients with Klippel-Feil syndrome. In addition, because the intrauterine development of the spine occurs at a similar time, the genitourinary system should be evaluated with renal ultrasound to ensure normal development.2
The clinical examination will demonstrate a low hairline with a short, webbed neck and restricted range of motion. There is a wide spectrum of motion because only a mild single-level fusion of the cervical spine is defined as KlippelFeil syndrome, and almost-complete fusion is given the same diagnosis. Radiographic features include cervical spine fusions in either single levels or multiple levels, or there may be two blocks of vertebrae separated by a single motion segment. A spot lateral radiograph is ideal to identify the deformities and fusions (Fig. 216-2); however, anteroposterior (AP) and open-mouth views are also necessary for a complete initial evaluation of the cervical spine. Visualization of the entire thoracic and lumbar spine is also necessary to fully evaluate any scoliosis in these regions of the spine. Referral to the orthopedist is necessary for full evaluation of these deformities and would include a neurologic examination to assess for upper motor neuron signs or other neurologic deficits. Lateral radiographs of the cervical spine with the head positioned in flexion and extension are important to look for cervical spine instability. Further evaluation with magnetic resonance imaging (MRI) is important, especially for those patients who demonstrate neurologic abnormalities or who have cervical spine instability.
Patients with Klippel-Feil syndrome usually only require education of the patient and family to refrain from high-energy activities that may lead to cervical neck injuries. Surgical treatment is necessary only when there is increasing or painful deformity or neurologic deficits. Surgical decompression of the cervical spinal cord is necessary when neurologic deficits are present, and fusion to stabilize the spine is important if progression of the spine deformity occurs or there is instability.
The spine has normal sagittal plane contours to include lordosis (swayback to the cervical spine). When kyphosis occurs, it can be due to many causes including congenital abnormalities that are most often associated with syndromes such as Larsen’s syndrome, diastrophic dysplasia, camptomelic dysplasia, and neurofibromatosis. These cervical kyphoses are important to recognize because they can result in constriction of the spinal cord and neurologic deficits. Any young patient should be evaluated for a syndromic condition by a dysmorphologist or a geneticist. Treatment is necessary for progressive deformity or when neurologic deficits occur. Surgical treatment is the only definitive treatment and requires either posterior fusion or anterior and posterior fusion combined with decompression when neurologic problems occur. Iatrogenic kyphosis is most often due to a previous removal of the posterior elements to gain access to the neural elements for tumors, infection, or syringomyelia. The loss of the posterior elements leads to kyphosis which can result in neurologic deficits.
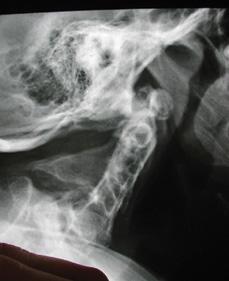
FIGURE 216-2. Lateral radiograph demonstrating congenital fusion of the cervical spine (Klippel-Feil syndrome).
SCOLIOSIS
A lateral curvature of the spine with rotational deformity in the axial spine is true scoliosis. Those with scoliosis can be divided into those who have an underlying neurologic condition and subdivided into upper motor neuron (cerebral palsy, Charcot-Marie-Tooth disease) and lower motor neuron (spinal muscular atrophy, myelomeningocele). Myopathic conditions include Duchenne’s muscular dystrophy and arthrogryposis. Connective tissue conditions include Marfan’s syndrome and osteogenesis imperfecta. One of the most common miscellaneous categories includes neurofibromatosis. Congenital scoliosis refers to a failure of segmentation (separation) or formation of the vertebra which distorts the spine by the absence of normal rectangular vertebrae. The most common type of scoliosis seen is idiopathic in which an identifiable cause cannot be found.
 IDIOPATHIC SCOLIOSIS
IDIOPATHIC SCOLIOSIS
This is the most common type of scoliosis, and it can be divided by age group into infantile (0 to 3 years), juvenile (3 to 10 years), and adolescent (> 10 years).3 The vast majority of patients with idiopathic scoliosis present secondary to an observed abnormal appearance in their spine which is visualized as a shifting of the body to one side, waistline asymmetry, shoulder height differences, or a prominence seen in the back. Scoliosis can be defined as a lateral curvature of the spine > 10°, with rotational deformity as the hallmark of this spinal curvature.
The incidence of scoliosis in the adolescent period is approximately 2% with only 0.6% of patients requiring treatment. Adolescent idiopathic scoliosis (AIS) is more commonly seen in girls, especially when the curves are larger. Although the etiology of idiopathic scoliosis is not known, we know that AIS curves progress in two main ways: first, with continued spinal growth curves tend to progress, and second, if curves are > 45° to 50° at the time of skeletal maturity, curve progression in adulthood is likely.
Infantile and juvenile scoliosis differ from the more common adolescent scoliosis in that curve progression is more likely because patients are younger and underlying neural axis abnormalities (ie, syringomyelia, tethered cord, diastatometamyelia) are seen in 20% of patients. An MRI of the entire spine is necessary to identify these abnormalities. The position and angle of the ribs relative to the spine at the apex of the deformity are used to predict curve progression.
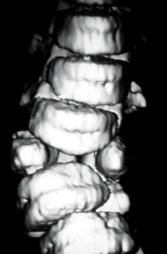
FIGURE 216-3. Computerized tomography (CT) scan of the spine demonstrating a congenital abnormality with resultant scoliosis.
 CLINICAL FEATURES
CLINICAL FEATURES
Patients with idiopathic scoliosis do not present with symptoms of pain. The deformity is noticed by family members, as well as nurses when school screening is performed, or by the pediatrician during annual visits. The physical examination is best performed with the patient standing in a relaxed position with feet together and arms at his or her sides. The patient is visualized from the back to look for shoulder height asymmetry, waistline asymmetry, or prominences in the back secondary to the rotational deformity. The Adam’s forward bend test is then performed by having the patient bend forward at the waist with the arms dangling in front in a very relaxed position. The rotational deformity of the spine is easily visualized or palpated (Figs. 216-3 through 216-5). Pain with palpation may indicate a diagnosis other than idiopathic scoliosis, and further imaging will be necessary. A careful neurologic examination is always performed in a patient with scoliosis to include a good motor examination, sensory examination, and most importantly, reflex examination. The most reliable reflex examination is the presence of abdominal reflexes in which the abdomen is stroked from medial to lateral. The umbilicus should move toward the stroked side. Symmetric (right and left) presence or absence of these reflexes is considered normal, and asymmetry or absence suggests neurologic abnormality.
During the Adams forward bend test, a scoliometer can be utilized to objectively measure the rotational deformity. In general, patients with curves > 7° on the scoliometer reading should be referred to the orthopedist. This usually represents a 20° coronal radiographic curve measurement.
Radiographic imaging can be performed but is often done at the orthopedist’s office. This includes a standing posteroanterior (PA) view, as well as a lateral view of the spine to include the cervical, thoracic, lumbar, and sacrum. On the PA view, the curves are measured using the Cobb method, which is performed by measuring the largest curve, and angular measurements are then determined (Fig. 216-6). Other important parameters on the radiographs include assessment of the Risser sign, the status of ossification of the iliac wing apophysis which correlates with the amount of remaining spinal growth. A Risser stage 0 or 1 indicates significant remaining spinal growth, and a Risser stage 4 or 5 indicates little remaining growth. Rapid spinal growth is occurring when the growth plate of the acetabulum (triradiate cartilage) is open and when girls are premenarchal.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


