Diagnosis and Management of Thrombosis
Janna M. Journeycake and Anthony K. C. Chan
Thrombosis, defined as excessive clotting, has three main causes: reduced blood flow (stasis), increase in blood coagulation factors (hyper-coagulability), and abnormalities in the vessel wall. Once the endothelium is injured, platelet adhesion is accompanied by platelet aggregation and thrombin formation. This process is usually tightly regulated in order to prevent excessive bleeding or clotting. However, at times, the process is uncontrolled, and a thrombus can form in excessive amounts or in an unusual place, causing harm.
Thrombosis and thrombophilia in childhood is of increasing concern. Although symptomatic thrombotic disease in children is rare when compared with adults, its occurrence can lead to mortality or life-long sequelae. The reported rate of thrombosis is 5.3 per 10,000 hospitalized patients, with a bimodal peak in incidence in the neonatal and adolescent age groups.1-4 Less than 10% of events in children are idiopathic.1-4 Thrombosis during childhood is a multifactorial event caused by both genetic and acquired risk factors.  Most children with thrombosis have an underlying medical condition that alters the hemostatic system to induce activation of coagulation and/or to prevent the inhibition of coagulation. The majority of conditions are related to inflammation or to abnormal blood flow (Table 438-1). In addition to the hemostatic changes secondary to underlying illness, many children also have the additional risk factor of a central venous catheter inserted to facilitate therapy for the underlying illness.1-3,7,8 The use of central venous catheter constitutes the most common acquired risk factor for thrombosis.5,7,8 As many as 60% of children with thrombosis will also have an inherited prothrombotic abnormality (Table 438-2), but the clinical relevance of congenital thrombophilia in asymptomatic children or in the presence of an acquired risk factor (eg, the presence of a central venous catheter) in childhood is still uncertain.1,9,10 There is debate about which children to screen, as well as when and how, for these genetic states. Families should be counseled about the significance of a prothrombotic state before testing is performed, especially in asymptomatic children. The pediatric community needs to be able to educate families about the signs and symptoms of thromboembolic disease, medical treatments and their potential adverse effects, and types of inherited and acquired thrombophilias.
Most children with thrombosis have an underlying medical condition that alters the hemostatic system to induce activation of coagulation and/or to prevent the inhibition of coagulation. The majority of conditions are related to inflammation or to abnormal blood flow (Table 438-1). In addition to the hemostatic changes secondary to underlying illness, many children also have the additional risk factor of a central venous catheter inserted to facilitate therapy for the underlying illness.1-3,7,8 The use of central venous catheter constitutes the most common acquired risk factor for thrombosis.5,7,8 As many as 60% of children with thrombosis will also have an inherited prothrombotic abnormality (Table 438-2), but the clinical relevance of congenital thrombophilia in asymptomatic children or in the presence of an acquired risk factor (eg, the presence of a central venous catheter) in childhood is still uncertain.1,9,10 There is debate about which children to screen, as well as when and how, for these genetic states. Families should be counseled about the significance of a prothrombotic state before testing is performed, especially in asymptomatic children. The pediatric community needs to be able to educate families about the signs and symptoms of thromboembolic disease, medical treatments and their potential adverse effects, and types of inherited and acquired thrombophilias.
Table 438-1. Major Medical Illnesses Associated with Thromboembolic Complications
Need for central venous catheter |
Malignancy |
Infection: sepsis, musculoskeletal infections, head and neck infections |
Congenital heart disease |
Trauma |
Burns |
Malignancy and associated therapies |
Inflammatory diseases: systemic lupus erythematosis, inflammatory bowel disease |
Renal disease: nephrotic syndrome, renal transplantation Liver disease |
Major surgery |
Pregnancy |
Obesity |
Diabetes mellitus |
Vascular malformations |
TYPES OF THROMBOSIS
 DEEP VEIN THROMBOSIS (DVT) OF EXTREMITY
DEEP VEIN THROMBOSIS (DVT) OF EXTREMITY
The signs and symptoms of acute DVT typically include swelling, pain, warmth, and a reddish purple discoloration of the extremity. Confirmation of diagnosis in a symptomatic patient is easily accomplished by a compression Doppler ultrasound of the affected extremity.4,11-14 Magnetic resonance venography and contrast venography can aid in the diagnosis if there is concern for central thrombosis (eg, in the superior vena cava) or if the ultrasound study is inconclusive. For thrombosis in the intrathoracic blood vessels (eg, subclavian vein) sonography may not be sensitive enough, so a venogram is required. The commonly used D-dimer test has not been well studied in children as a diagnostic tool for deep vein thrombosis. 
 PULMONARY EMBOLISM
PULMONARY EMBOLISM
Pulmonary embolism (PE) is considered a rare event in children, but the incidence is likely underestimated as most cases are not detected until autopsy.1 No prospective clinical trial has evaluated all children who have symptomatic thrombosis for objective evidence of PE. Hence, its incidence remains unknown. Because affected children generally have a concurrent medical condition with symptoms that can mimic those of PE (ie, dyspnea, chest pain, hypoxia, fever), physicians do not often have a high index of suspicion for thrombosis. Diagnosis can be made with a spiral computed tomography (CT) scan, CT angiography, or by ventilation/perfusion (V/Q) scan.22 The incidence of PE associated with deep vein thrombosis is approximately 25%, and children with PE are likely to have a hypercoagulable state identified.22
 CATHETER-RELATED THROMBOSIS
CATHETER-RELATED THROMBOSIS
As many as 60% of thrombotic events in children and 90% of thrombotic events in neonates are associated with the use of indwelling catheters.1,7
The prevalence of catheter-related central venous thrombosis is as high as 50% in children who have cancer, hemophilia, chronic malnutrition, and other medical conditions.7,30-33 Although the majority of central venous catheters (CVCs) in children are inserted into the veins of the upper extremities and chest, catheter-related thrombosis can be seen in any extremity and within the right atrium. The gold standard test to identify catheter-related deep vein thrombosis (DVT), particularly of the upper extremity, is contrast venography.11-14 Compression Doppler ultrasonography (appropriate for screening lower extremities) may not identify thrombi in the subclavian and central veins, but is often better at identifying occlusion of jugular veins.11,14 Therefore, it is recommended that both modalities be used to assess the vessels of the upper venous system. Magnetic resonance venography is an appealing alternative because it can image all veins,13 but it is sensitive to motion artifact and many young children will require sedation to undergo the study.7
Compression Doppler ultrasonography (appropriate for screening lower extremities) may not identify thrombi in the subclavian and central veins, but is often better at identifying occlusion of jugular veins.11,14 Therefore, it is recommended that both modalities be used to assess the vessels of the upper venous system. Magnetic resonance venography is an appealing alternative because it can image all veins,13 but it is sensitive to motion artifact and many young children will require sedation to undergo the study.7
Although clinically overt DVT develops in association with an indwelling CVC, the incidence of subacute or “silent” thrombi in children who have catheters is far greater. These subacute DVTs still have clinical significance because numerous studies have demonstrated the association of catheter-related DVT, catheter-related infection, and catheter occlusion.7,34-41
When catheter-related thrombosis is identified, many issues arise about its management, including the necessity for anticoagulation and its intensity and duration once initiated. Although the best management includes removal of the catheter,49 this may be impractical in a critically or chronically ill child who has limited intravenous access. The most recent consensus guidelines for treatment of central venous catheter–related thrombosis in children recommend anticoagulation to prevent propagation or sequelae of the thrombus if the catheter cannot be removed.49 The natural history of catheter-related deep vein thrombosis has not been defined. 
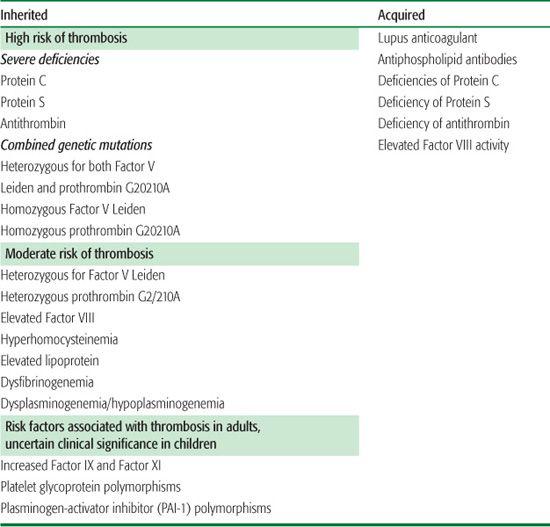
Table 438-2. Inherited and Acquired Thrombophilia
 RENAL VEIN THROMBOSIS
RENAL VEIN THROMBOSIS
Renal vein thrombosis usually presents within the first month of life. The classic triad of flank mass, macroscopic hematuria, and thrombocytopenia occurs only in about 25% of patients.71 Risk factors include maternal gestational diabetes, perinatal asphyxia, and dehydration, but these are identified in less than one third of babies.71 Outside of the neonatal period, most children will have associated nephrotic syndrome.72 Aggressiveness of treatment will be determined by extent of thrombosis. Anticoagulation with or without thrombolytic therapy is recommended for bilateral thrombosis, unilateral thrombosis extending into the inferior vena cava, or signs of impending renal failure.71,72 However, there is no clear evidence that anticoagulation therapy improves renal outcome.71
 PORTAL VEIN THROMBOSIS
PORTAL VEIN THROMBOSIS
Portal vein thrombosis can lead to the serious and life-threatening complication of portal hypertension, esophageal varices, and gastrointestinal bleeding. Initially, portal vein obstruction can present as asymptomatic splenomegaly. Causes include umbilical vein catheterization (particularly if the line is in place for more than 3 days or is subdiaphragmatic in position), compression by tumors in the abdomen, abdominal trauma or infection, dehydration, and inherited hypercoagulable states. Unfortunately, the majority of cases have no identifiable etiology. Diagnosis is typically made by Doppler ultrasonography. Most portal vein thrombosis outside of the neonatal period is diagnosed in the chronic stage after cavernous transformation has occurred. Anticoagulation is not generally indicated in this setting due to increased risk of variceal bleeding. These children may need surgical interventions such as portosystemic shunting or splenectomy. 
THROMBOPHILIA
Thrombophilia is the increased likelihood for development of thrombosis. It may be hereditary, due to abnormality of the coagulation system, or acquired.
 INHERITED CONDITIONS
INHERITED CONDITIONS
The lifetime risk of thrombosis in a child who is a carrier of thrombophilia is estimated to be fourfold higher compared to normal population.7,74 However, healthy young children who have single thrombophilic defects rarely present with thrombosis during childhood.75,76 The risk of thrombosis seems to increase with multiple thrombophilia traits and with the addition of exogenous risk factors.77
The list of current known thrombophilias is shown in Table 438-2.
Protein C, protein S, and antithrombin are the natural anticoagulants regulating hemostasis. Although deficiencies of these proteins are rare (0.03% to 0.1% of population), they are strongly associated with a first thrombotic event prior to age 40 years. Severe homozygous congenital protein C or protein S deficiency usually presents within a few days of birth with disseminated intravascular coagulation, purpura fulminans, and large vessel thrombosis that affects the eyes, central nervous system, aorta, vena cavae, and renal veins.81 Early and indefinite anticoagulation therapy is necessary for these severe deficiencies.  Antithrombin deficiency is generally identified in later childhood, as severe deficiencies are rare and in the homo-zygous state may be incompatible with life.83
Antithrombin deficiency is generally identified in later childhood, as severe deficiencies are rare and in the homo-zygous state may be incompatible with life.83
These antithrombotic regulatory proteins can be affected by age and acute health status. For example, they are decreased in newborn infants.3,84 In addition, underlying medical conditions, including sepsis, nephrotic syndrome, liver disease, inflammatory bowel disease, and childhood leukemia therapy can cause acquired deficiencies in the natural anticoagulation regulatory proteins.83,85 Finally, they can be consumed in a massive thrombus.
Factor V Leiden is the most common inherited thrombophilia mutation. Its estimated prevalence is 5% in those of European ancestry. It is rare in persons of African or Asian ancestry. This mutation in factor V leads to resistance of factor V inactivation by activated protein C and protein S. The heterozygous state causes a 5-fold to 8-fold increased risk for thromboembolic complications. The homozygous state confers an 80-fold increased lifetime risk.77
The prothrombin G20210A mutation occurs in approximately 3% of the general population. Its presence increases the risk for thrombosis mainly by causing excess prothrombin production. The heterozygous state increases the risk for thromboembolic events threefold. However, a recent meta-analysis demonstrated that the presence of this mutation is significantly associated with the risk of recurrence for thrombosis in children.77
Lipoprotein (a), which is involved in cholesterol metabolism, competes with plasminogen for binding to fibrin. It therefore slows fibrinolysis and is associated with thrombosis. Elevations in lipoprotein (a) are associated with accelerated arterial vascular disease in adults. Preliminary studies of children describe elevations in lipoprotein (a) in association with venous and arterial thrombosis, but these data require confirmation.77,86 Elevated levels of plasma homocysteine are also associated with vascular disease in adults and thought to be a risk factor for stroke in children. Polymorphisms of the thermolabile methylenetetrahydrofolate reductase (MTHFR) gene may contribute to elevations of homo-cysteine levels.87
The presence of elevated factor VIII at the time of diagnosis of deep vein thrombosis and its persistence has been shown to be associated with increased risk of recurrent events.92 Other genetic polymorphisms that predispose to thrombosis have yielded conflicting results or are still under initial investigation.
 ACQUIRED CONDITIONS
ACQUIRED CONDITIONS
Malignancy
As in adults, cancer is one of the primary conditions associated with thromboembolism in children. Acute lymphoblastic leukemia (ALL) is the most common malignancy in children. At diagnosis, these children demonstrate activated coagulation as evident by having increased levels of thrombin-antithrombin complexes stimulated by tumor cells.93 However, they also may have long-term tunneled central venous catheters for administration of intravenous therapy.93-95 Also, they are treated with chemotherapeutic agents that are caustic to vessel walls and/or can induce a transient hypercoagulable state.93,96
Infection
Thrombosis may occur as a complication of systemic or invasive local infection. Head and neck infections may trigger cerebral sinovenous thrombosis.51 Musculoskeletal infections, particularly those associated with Staphylococcus aureus, are being recognized as predisposing to venous thrombosis.100,101
Liver Disease
Liver disease will lead not only to a decreased production of all of the coagulation factors except factor VIII but also reduction in concentrations of the natural anticoagulant proteins C and S and antithrombin. Accordingly, thrombosis may result.
Congenital and Acquired Heart Disease
Another condition highly associated with both venous and arterial thrombotic events is complex congenital heart disease.102 Cardiac catheterization required for diagnosis and treatment carries a risk of arterial thrombosis at the site of catheterization, primarily the femoral artery. 
Antiphospholipid Antibodies
Antiphospholipid antibodies include the lupus anticoagulant (LA), and anticardiolipin, antiphosphatidyl serine, antiprothrombin, and anti-β-2-glycoprotein I antibodies.109 The LA is present in approximately 25% of children who develop thrombosis.23 Children who have LA should be retested at least 12 weeks after the first test, and at least 2 screening methods should be used. The association of a persistent antiphospholipid antibody with symptomatic thromboembolism defines the antiphospholipid antibody syndrome, which is associated with a high recurrence rate; thus, long-term (indefinite) anticoagulation should be considered.49
Oral Contraceptive Pills (OCPs)
Oral contraceptives are commonly prescribed to teenage girls for a variety of medical indications. Oral contraceptive pill use has been associated with threefold to tenfold increased incidence of deep vein thrombosis (DVT) in an otherwise young, healthy female population. The incidence of DVT is highest in the first year of use.111 This risk is further increased in the presence of hyper-coagulable disorders, particularly factor V Leiden.112 Risk of DVT development in patients with factor V Leiden is increased by approximately 35-fold when they are taking OCPs. Screening patients for factor V Leiden prior to initiating use of OCPs has been debated. However, because of the cost of testing and the low mortality related to DVT, the consensus has been to screen only those patients with a personal or family history of venous throboembolism.111 Having inherited thrombophilia without a personal history of thrombosis is a relative contraindication for use of OCPs. However, in adolescents with thrombophilia, alternatives to OCP for medical conditions such as acne and menorrhagia should be strongly considered.
 SCREENING FOR THROMBOPHILIA
SCREENING FOR THROMBOPHILIA
The need for thrombophilia screening, particularly in asymptomatic children, is debatable. The incidence of thromboembolism in children who are younger than 15 years of age with confirmed thrombophilia is low.75 Anticoagulation prophylaxis in high-risk situations such as major surgeries or trauma could prevent thrombosis in children who are identified with thrombophilia,112,113 although this is theoretical and has not been tested in clinical trials. Many inherited causes of thrombophilia are unknown, so a negative screening test in a child with a significant family history does not guarantee that the child will not develop thrombosis. 
Some experts recommend screening symptomatic children for all known thrombophilic conditions at the time of diagnosis. However, after an acute thrombotic event, transient reductions due to consumption of some natural anticoagulant proteins may occur.116 A low level should always prompt measurement 3 to 6 months later to confirm a congenital deficiency. Despite the potential for transient deficiency, identifying significantly low protein C, protein S, or anti-thrombin levels at the time extensive or progressive life-threatening thrombosis is diagnosed would provide an opportunity to replace the factor with protein concentrates or fresh-frozen plasma.116 Genetic (polymerase chain reaction– based) testing for the thrombophilic mutations can be performed reliably at any time and is accurate at the time of acute thrombosis. Testing at the onset may obviate difficulties with patient follow-up. Table 438-3 outlines one approach to testing a symptomatic child for prothrombotic conditions. 
TREATMENT
Guidelines for the treatment of thromboembolic events in neonates and children have been extrapolated from the experience in adults. Virtually no randomized clinical trials have been completed in children that successfully define optimal duration and dosing. However, published guidelines by the American College of Chest Physicians are acknowledged by many as reasonable and rational, even though not strongly evidence based.49
 UNFRACTIONATED HEPARIN AND LOW-MOLECULAR-WEIGHT HEPARIN
UNFRACTIONATED HEPARIN AND LOW-MOLECULAR-WEIGHT HEPARIN
Unfractionated heparin administered as a continuous infusion functions by binding to anti-thrombin, which allows inhibition of thrombin as well as factor Xa.117 Because it is a large molecule, it can bind other plasma proteins, macrophages, platelets and platelet factor 4, osteoclasts, and endothelial cells, leading to the potential complications related to heparin, such as heparin-induced thrombocytopenia and bone loss. Low-molecular-weight heparins (LMWHs) given subcutaneously are smaller molecules that lack a pentasaccharide subunit. Therefore, this compound has reduced binding to plasma proteins, macrophages, and endothelial cells, which makes for more predictable pharmacokinetics and a longer half-life. It also has reduced platelet and osteoclast binding, which decreases the rates of heparin-induced thrombocytopenia and osteoporosis.117 However, because of the shortened length, it cannot bind to antithrombin and thrombin simultaneously. The main mechanism of action is via factor Xa inhibition.
Because the activity of heparin relies on the presence of antithrombin, some children may be resistant to standard doses of anticoagulation and cannot achieve therapeutic levels. Antithrombin levels are often reduced in very young or ill children.118 Antithrombin supplementation may be necessary for these patients who appear to be resistant to heparin therapy or who cannot achieve therapeutic levels. Neonates may require higher doses of heparin because the clearance is more rapid secondary to a large volume of distribution.119,120 The risk of bleeding associated with the use of heparin is 1.5% to 10%.119 Heparin-induced thrombocytopenia is reported occasionally in pediatric patients receiving unfractionated heparin, but is rare with LMWHs.120
Table 438-3. An Approach to Screening Children for Thrombophilia77,117



