Board Simulation: Potpourri
Robert J. Cunningham III
Camille Sabella
QUESTIONS
1. Respiratory distress develops in a 10-hour-old term infant. Physical examination reveals tachypnea, diminished breath sounds on the left side of the chest, and a scaphoid abdomen. The most likely diagnosis is:
a) Sepsis
b) Transient tachypnea of the newborn
c) Pneumothorax
d) Congenital diaphragmatic hernia
e) Meconium aspiration
View Answer
Answer
The answer is d. The findings of a scaphoid abdomen and diminished breath sounds in the chest of a newborn infant are characteristic of congenital diaphragmatic hernia. A poster lateral defect (Bochdalek type) is most common, and 75% to 85% of defects occur on the left side; 5% are bilateral. Chest radiography is diagnostic, although the diagnosis can be made prenatally with ultrasonography. A 40% to 50% mortality rate is associated with congenital diaphragmatic hernia; long-term complications, such as growth and developmental delays, gastroesophageal reflux, pectus excavatum, and scoliosis, are common.
2. Bilious vomiting develops in a 1-day-old infant (Fig. 68.1). This infant’s condition is most closely associated with:
a) Cystic fibrosis
b) Turner syndrome
c) Trisomy 21
d) DiGeorge syndrome
e) Vertebral anomalies
View Answer
Answer
The answer is c. Bilious vomiting and the appearance of a “double bubble” (Fig. 68.1) in a newborn infant are characteristic of duodenal atresia, which accounts for 25% to 40% of all cases of intestinal atresia. Fifty percent of infants with duodenal atresia are premature, and associated anomalies include:
Trisomy 21 (20%-30%)
Malrotation (20%)
Esophageal atresia (10%-20%)
Bilious vomiting without abdominal distension, maternal polyhydramnios, and the “double bubble” finding on abdominal x-ray film are common features.
3. A 6-month-old boy is brought in for a well-baby visit. On examining the infant, you note a white pupil in his
left eye. The infant was born at 33 weeks of gestation with a birth weight of 2000 g. The least likely cause of a white pupil in this infant is:
left eye. The infant was born at 33 weeks of gestation with a birth weight of 2000 g. The least likely cause of a white pupil in this infant is:
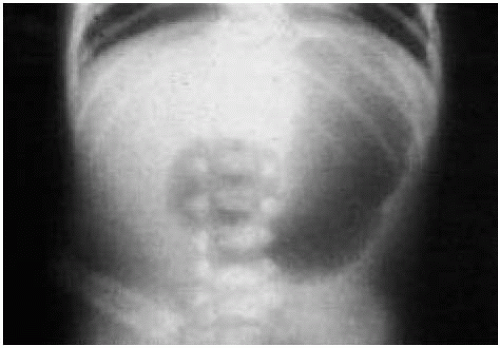 Figure 68.1 Abdominal film of the patient in question 2. See explanation of question 2 for details. |
a) Congenital cataract
b) Glaucoma
c) Retinoblastoma
d) Retinopathy of prematurity
View Answer
Answer
The answer is d. The differential diagnosis of leukocoria includes all of the choices listed in this question. Although retinopathy of prematurity is a cause of leukocoria, it occurs in infants who are born before 33 weeks of gestation, with a birth weight <1500 g. Therefore, the leukocoria of the infant described in the question is least likely to be associated with retinopathy of prematurity.
Case for Questions 4-5
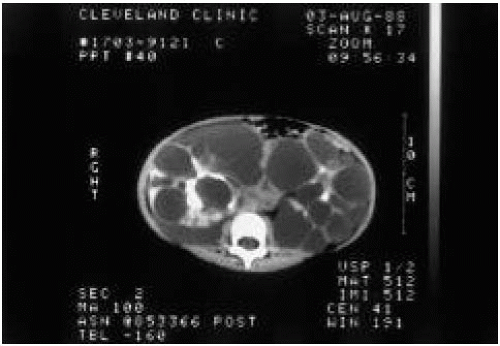
A girl who is now 5 years old was taken to her pediatrician at 6 months of age with abdominal masses. At 18 months of age, she had seizures 5 days after vaccination with diphtheria-tetanus-pertussis booster. She is severely developmentally delayed. Her renal ultrasonogram is shown in Figure 68.2.
4. The most likely diagnosis is:
a) Infantile polycystic kidney disease
b) Adult polycystic kidney disease
c) Tuberous sclerosis
d) Multicystic kidney disease
View Answer
Answer
The answer is c. The most likely diagnosis is tuberous sclerosis, which is usually inherited in an autosomaldominant manner. Tuberous sclerosis is characterized by a seizure disorder, pathognomonic skin lesions (ash leaf lesions and hypopigmented macules; see Fig. 35.5), calcified tubers in the brain, rhabdomyomas of the heart, and hamartomas or polycystic disease in the kidneys. The clinical manifestations vary widely from patient to patient. The incidence of tuberous sclerosis is high in infants who present with infantile spasms.
5. What is the best study to confirm your diagnosis?
a) Urinalysis
b) Ultrasonography of the liver
c) Computed tomography (CT) scan of the brain
d) Cerebral angiography
View Answer
Answer
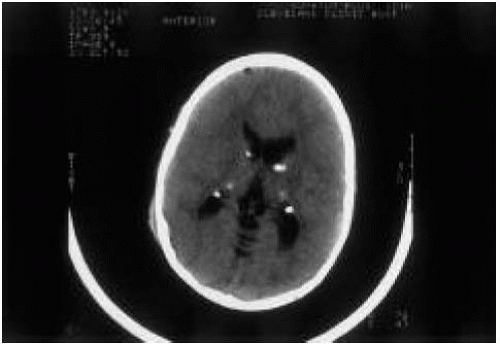
The answer is c. Tubers in the brain are diagnostic of tuberous sclerosis. They are typically found in the subependymal region and undergo calcification (Fig. 68.3). The tubers may not be apparent until a patient with tuberous sclerosis is 3 to 4 years of age.
6. A 3-year-old boy is referred to you with a history of increasingly severe headaches. Physical examination reveals skin lesions (Fig. 68.4). The child’s father has similar lesions on his trunk and a “lumpy” tumor at
the base of his wrist. The child’s blood pressure is 150/110 mm Hg. The most likely cause of this child’s hypertension is:
the base of his wrist. The child’s blood pressure is 150/110 mm Hg. The most likely cause of this child’s hypertension is:
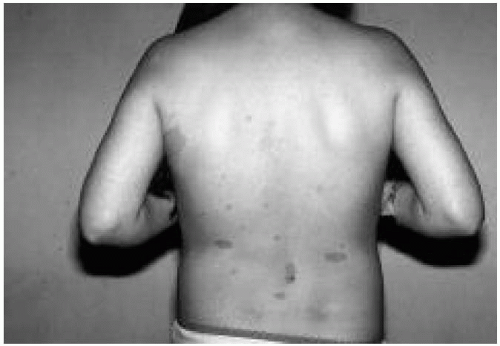 Figure 68.4 Skin lesions in patient in question 6. See explanation of question 6 for details. (See color insert.) |
a) Coarctation of the aorta
b) Conn syndrome
c) Renal artery stenosis
d) Multicystic kidney disease
View Answer
Answer
The answer is c. The presence of café au lait lesions, which are evident in Figure 68.4, and the family history of similar lesions are consistent with a diagnosis of neurofibromatosis. Patients with neurofibromatosis have an increased incidence of:
Renal artery stenosis
Pheochromocytoma
Optic gliomas
Neurofibromas
Renal artery stenosis is common in children with neurofibromatosis, whereas pheochromocytoma is common in adults with neurofibromatosis.
7. A worried mother brings her two sons to your office. They are 5 and 7 years of age. Her concern is that her father’s brother has just been started on dialysis and has adult-onset polycystic kidney disease. The mother’s father was evaluated and had normal findings on renal ultrasonography. Which of the following studies should be performed to alleviate the mother’s concern?
a) Renal ultrasonography
b) Intravenous pyelography
c) Abdominal CT scan with contrast
d) Liver function studies and liver ultrasonography
e) None of the above
View Answer
Answer
The answer is e. Adult-onset polycystic kidney disease is transmitted in an autosomal-dominant pattern. Therefore, if the mother’s father does not have the disease, the mother is not at risk and her children cannot be affected. Patients with adult-type polycystic kidney disease (autosomal dominant) usually begin to have symptoms at 40 to 60 years of age, although cysts may be present early in life. Approximately 12% of patients have associated berry aneurysms.
8. You are asked to see an expectant mother for prenatal counseling because the fetus has been noted to have two large kidneys, both with numerous large cysts. The mother wants to know whether her child has polycystic kidney disease and if so what problems the infant might have. Which of the following is true?
a) The infant will most likely be born with renal failure and will require immediate dialysis.
b) Severe respiratory distress in the early newborn period is likely.
c) The risk that siblings will be affected is 50%.
d) Signs of hepatic fibrosis may develop in older children with infantile polycystic kidney disease.
View Answer
Answer
The answer is b. The infantile type of polycystic kidney disease is transmitted in an autosomal-recessive fashion. Therefore, the risk that subsequent children will have the disease is 25%. The clinical manifestations appear early in infancy; hypoplastic lungs are commonly associated, so that respiratory distress in the newborn period is likely. The disease is also associated with congenital hepatic fibrosis.
9. A 13-year-old mentally retarded and institutionalized child with tuberous sclerosis is brought to your office with swelling of both wrists, which appear painful when touched. No erythema or fever is present. Radiographs show widening of the epiphyseal plates and “fraying.” Which historical factor is important?
a) History of milk allergy
b) Family history of osteoporosis
c) Seizure disorder controlled with phenytoin (Dilantin)
d) History of stopping multivitamins 3 months earlier
e) History of a fractured rib
View Answer
Answer
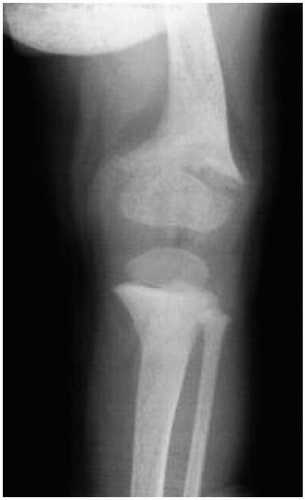
The answer is c. This is a summary of one of the first cases of anticonvulsant-induced rickets. The child was institutionalized and found to have rickets on radiography. The radiographic features of rickets include widened, concave, and frayed epiphyses (Fig. 68.5 and see Fig. 18.2). Although she lived in the United States and her intake of milk was normal, her exposure to sunlight was limited. She was being treated with both phenytoin and phenobarbital, and these agents stimulate the liver enzymatic systems that accelerate the destruction of 1,25-dihydroxycholecalciferol. Anticonvulsant therapy is a rare but important cause of rickets.
10. You are asked to perform a preoperative evaluation for a patient who is undergoing surgery to correct ptosis. The patient previously had an orchiopexy, is below the fifth percentile for height, and has a webbed neck. Physical examination reveals a midsystolic murmur heard over the entire chest and pronounced over both sides of the back. You conclude that the child has:
a) Holt-Oram syndrome
b) Menkes disease
c) Russell-Silver syndrome
d) Noonan syndrome
View Answer
Answer
The answer is d. This child likely has Noonan syndrome, a usually sporadic disorder in which the karyotype is normal. The anomalies of Noonan syndrome also occur in girls with Turner syndrome. The most common ones include:
Short stature
Webbed neck
Pectus excavatum or carinatum
Congenital heart disease
Characteristic facies (hypertelorism, epicanthus, ptosis, micrographic)
Moderate mental retardation (25% of cases)
The most common cardiac defects are pulmonic valvular stenosis and atria septal defect. Russell-Silver syndrome (Fig. 68.6) is characterized by:
Short stature that becomes apparent even before birth
Small, triangular face
Asymmetry of the limbs
Small, inwardly curved little finger
Large, persistent fontanelle
Holt-Oram syndrome is characterized by both skeletal and cardiovascular abnormalities. The common skeletal abnormality is a defect of the upper limb (absent thumb, syndactyly, or an absent radius). This often is asymmetric, with only one side involved, but occasionally involvement is bilateral. The most commonly associated cardiac defects are ostium secundum atrial septal defect and ventricular septal defect.
Menkes disease is an X-linked-recessive defect of copper metabolism. The levels of both ceruloplasmin and copper have been low in all patients studied. The disease is characterized by a profound neurologic deficit that becomes evident by 1 to 2 months of life, and the process is degenerative. Death usually occurs by 3 years of age. The unusual feature of this disease is kinky hair. The hair is sparse and lightly pigmented, and twisting and partial breakage are apparent when the hair is viewed through a magnifying glass.
11. A 13-year-old girl is seen for a routine physical examination after having moved to the United States from Egypt. She has had three past episodes of swelling in the middle of her neck associated with redness and exquisite tenderness. Her symptoms have resolved with antibiotic therapy. During the examination, a small mobile mass is noted just above the hyoid bone in the midline of the neck. The mass feels “fluctuant,” and it moves up and down when the patient sticks out and retracts her tongue. The most likely diagnosis of this mass is:
a) Branchial cleft cyst
b) Follicular carcinoma of the thyroid
c) Early lymphoma
d) Thyroglossal duct cyst
View Answer
Answer
The answer is d. Thyroglossal duct cysts are defects located in or near the midline of the neck; they may extend to the base of the tongue, and they occasionally contain aberrant thyroid tissue. Branchial cleft cysts are lateral in origin and may open to the skin surface or drain into the pharynx. They may become secondarily infected and require antimicrobial therapy. Thyroid carcinoma and lymphoma are very unlikely given this case history.
12. The State Health Department notifies your office that a newborn screening test has revealed a low thyroxine (T4) level in an infant now 7 days old. The best course of action is to:
a) Repeat measurements of the T4, thyroid-stimulating hormone (TSH), and free T4 levels.
b) Obtain a thyroid scan.
c) Begin thyroid replacement therapy now.
d) Obtain a skull film to assess sutures.
e) Answers a and b are correct.
f) Answers a and c are correct.
g) Answers a, b, and c are correct.
View Answer




Answer
The answer is f. Confirmation of the screening test result is necessary. Therefore, the infant’s T4, TSH, and free T4 levels should be measured. Once the results are available, therapy with levothyroxine should begin without delay. Therapy is discontinued if the confirmatory test results are negative. A thyroid scan should be performed only if the diagnosis of hypothyroidism is confirmed. Prolonged open sutures are a sign of congenital hypothyroidism, but this sign is not helpful diagnostically.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree