Anterior Segment Disorders
David S. Walton
The anterior segment of the eye consists of the cornea, the anterior chamber, the iris, the pupil, and the lens, which anatomically divides the anterior segment of the eye from its posterior segment. The posterior segment includes the vitreous gel, the retina, the optic nerve, and the choroid. This is a useful clinical division, because many diseases of the eye predominantly affect the anterior or posterior segment and are usefully differentiated from conditions (eg, endophthalmitis) that affect the whole eye. Casual inspection of the eye (the globe) is inevitably an assessment of the anterior segment structures and offers very little information about the internal, more posterior ocular structures. A checklist of anterior segment findings that may be recognized by the pediatrician would include cornea size and transparency; iris color (eg, heterochromia); pupil size, shape, position, and reaction to light; lens clarity (eg, cataract) and position (eg, dislocation/subluxation); and signs of elevated eye pressure.
CORNEA
Transparency of the cornea can be judged by how well the iris can be visualized and by noting the appearance of the normally black pupil. Comparing the patient’s cornea with those of a sibling or parent can be helpful. A cloudy cornea (Fig. 590-1) is always a significant clinical observation and has many pathological causes (Table 590-1). Corneal transparency is essential for normal vision, and its loss is an important cause of childhood blindness. Corneal opacification or change in the cornea’s size are essential signs of both systemic and ocular disease. Some corneal conditions that cause cloudiness are best treated promptly, such as glaucoma and corneal keratitis (inflammation or infection of the cornea). Glaucoma in young children causes corneal cloudiness and enlargement (Fig. 590-1), as well as optic neuropathy, potentially associated with permanent vision loss.
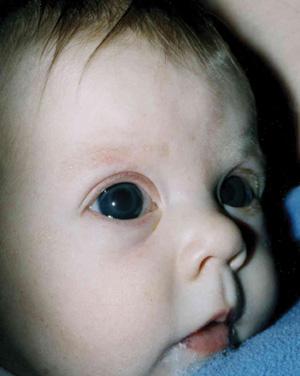
FIGURE 590-1. A 3-month-old girl with bilateral congenital glaucoma associated with corneal enlargement, cloudiness (note iris details are difficult to visualize), and photophobia.
The corneas are normally transparent and equal in diameter. Rapid growth occurs in infancy, reaching adult size of 10 to 13 mm in horizontal diameter by 12 to 81 months of life. A cornea with a diameter greater than 13 mm is considered enlarged, and a diameter less than 10 mm is considered small.1 These abnormalities are more easily appreciated when the two corneas differ is size; this is always abnormal and requires immediate investigation (Table 590-2).
Symptoms of corneal disease vary considerably. Acquired defects of the corneal epithelium produce intense pain associated with photophobia and tearing. Corneal tears secondary to continued corneal stretching from elevated intraocular pressure are associated with intense photophobia and discomfort. Systemic diseases associated with cornea deposits of storage material are typically asymptomatic. Corneal enlargement secondary to glaucoma can also be asymptomatic.
ANTERIOR CHAMBER
The anterior chamber is filled with aqueous humor, which is optically clear. This space is delineated anteriorly by the back surface of the cornea and posteriorly by the iris and the front surface of the lens. It is best examined with a slit beam of light, which is a routine component of ophthalmologic examinations. The slit beam from an ophthalmoscope or a handheld slit can be substituted when children are examined. Common abnormalities of the anterior chamber are shown in Table 590-3.
IRIS
Abnormalities of the iris and pupil are listed in Table 590-4. The iris (from Greek, iris means “rainbow”) is normally easily seen through the clear cornea and anterior chamber. It is variably colored from blue to dark brown, depending on the amount of melanin present. This pigmentation is normally uniform and approximately equal bilaterally. The architecture of the iris stroma making up the body of the iris is highly variable and is studied carefully by ophthalmologists for evidence of intraocular disease.
The pupils are usually approximately equal in size; they enlarge (dilate) in reduced illumination and constrict in response to increased light or with accommodation. Careful assessment of pupillary reactivity to a light stimulus is an important test of ocular and optic nerve function as well as a test of third nerve function. If pupil size is asymmetric, it is important to determine which is the abnormal pupil. If the relative disparity increases in bright light, the larger pupil is abnormal (ie, not constricting properly). If the disparity increases in dim light, the smaller pupil is abnormal (ie, not dilating properly). If the relative disparity is maintained regardless of the illumination, the child has physiological anisocoria, a finding seen in approximately 20% of the normal population. Examination of old photographs may be useful in establishing the congenital nature of this minor anomaly.
Table 590-1. Causes of Corneal Opacification in Childhood
Present at Birth—Congenital Anomalies |
Newborn infantile glaucoma |
Corneal hereditary dystrophies |
Corneolimbal dermoid |
Peters anomaly |
Anterior staphyloma |
Sclerocornea |
Trisomy 8 mosaic |
Presenting in Infancy or Childhood |
Congenital |
Infantile/congenital glaucoma (with Haab striae) |
Corneal ulceration (bacterial, corneal hypesthesia, tyrosinemia type 2) |
Metabolic disease (mucopolysaccharidoses, mucolipidosis 1V, infantile Niemann-Pick disease, Lecithin cholesterol acyl-transferase, Wilson disease, cystinosis) |
Corneal hydrops (trisomy 21, newborn congenital glaucoma, keratoconus) |
Acquired |
Trauma (forceps injury, accidental) |
Keratitis (herpes simplex, syphilis, maternal rubella, phlyctenule) |
Band keratopathy (juvenile idiopathic arthritis, uveitis) |
Arguably the most important pediatric pupil-lary eye sign is leukocoria, the white pupillary reflex, also referred to as the cat’s eye reflex (Fig. 590-2). This defect is caused by the reflection of light from a white cataract or from a white structure in the posterior segment. Many defects produce this reflex, including cataract, retinoblastoma, and retinal detachment. The expected “red reflex” is the normal reflection from the vascular choroid underlying the retina. It is rarely actually red but more often a combination of yellow, pink, and orange. Most importantly, it is symmetric between the two eyes. An absent red reflex (“black reflex”) is also a sign of intraocular disease, indicating an obstruction in the ability of light to reach and reflect back from the inner eye. Possible causes include cataract and presence of blood, but it is commonly merely the result of miosis (small pupils); pharmacological dilation of the pupils may reveal a normal red reflex and obviate the need for referral. An absent reflex or leukocoria should prompt urgent referral for ophthalmology consultation.
Table 590-2. Causes of Abnormal Corneal Size



