Fig. 10.1.
External marking of the pertinent anatomy after the patient is prepped and draped. This patient is marked out for potentially two bars. The deepest point of the defect is noted by the large central point. The inferior costal margin has been marked below for orientation. The intercostal spaces that will be used to pass the pectus bars through the thoracic cavity are also marked. The cephalad intercostal markings correspond with the bar that will pass under the deepest point of the defect. Courtesy of Dr. Brian Kenney at Nationwide Children’s Hospital.
The size of the bar is selected by measuring from the right to the left mid-axillary line at the greatest depression and subtracting 1–1.5 in. The bar should then be pre-bent for optimal configuration to the patient’s chest. A semicircular shape with a short flat central apex and gentle convex curve is most commonly used for all patients. Too angulated or a “tabletop” configuration will make for an unstable bar.
Steps
With the patient positioned, draped, marked, and the pectus bar formed to fit, the surgical procedure can begin. It is beneficial to start with thoracoscopy to confirm the internal anatomy prior to the substernal dissection. A small incision, large enough to accommodate a 5-mm trocar, is placed two intercostal spaces below the right lateral bar incision. The 5-mm trocar is placed and a 5-mm fiber-optic scope with a 30-degree angle of visualization is inserted into the thoracic cavity. Adequate visualization can usually be obtained with controlled ventilation by anesthesiology utilizing lower tidal volumes. CO2 insufflation of 5–6 mmHg can be utilized to increase visibility. Utilizing external palpation and internal visualization, the intercostal space previously marked for bar insertion is identified. Two lateral transverse incisions are made on either side of the chest wall. The incisions begin at the mid-axillary line and extend anteriorly 2–3 cm. If using two bars, one or two incisions can be made depending on the surgeon preference. The incision is carried down through the subcutaneous tissues to the chest wall. Once down to the chest wall, small subcutaneous flaps are raised circumferentially to accommodate the end of the pectus bar and the bar stabilizers. A subcutaneous tunnel is then created anteriorly along the chest wall extending to the previously marked points medial to the pectus ridge. This will be the site of entry into the thoracic cavity for the pectus bar . If the pectoralis muscle is present in the horizontal plane, it is preferable to make the tunnel beneath the muscle.
With thoracoscopic visualization, a tonsil clamp is used to enter the right side via the previously dissected tunnel. It is imperative to enter the chest medial to the highest point on the pectus ridge. The pectus introducer is then inserted into the pleural cavity through the previous tunnel and advanced beneath the sternum. Once in the thoracic cavity, the introducer is advanced and turned 180° so that the convexity is directed posteriorly and the tip anteriorly (Fig. 10.2). This keeps the tip directed away from the heart and other mediastinal structures, reducing the likelihood for injury. The introducer tip is then used to locate the bloodless dissection plane between the posterior sternum and the pericardium (Fig. 10.3). Using blunt dissection, the introducer is advanced until the left lateral mark on the pectus ridge is identified again through external palpation and internal visualization. The introducer is then advanced through the appropriate intercostal space (medial to the pectus ridge) into the left-sided subcutaneous tunnel and subsequently delivered through the left lateral incision (Fig. 10.4). It is critical to keep the introducer tip in view at all times to minimize cardiac injury. Various techniques of sternal elevation that have been described can facilitate this dissection and are a must if one cannot see the tip [25–27]. Bilateral thoracoscopy can also be utilized if one cannot visualize the space between the heart and sternum in very severe defects with torsion.




Fig. 10.2.
Passing the introducer into the thoracic cavity. (a) A tonsil clamp is used to enter the thoracic cavity through the previously determined intercostal space at a point just medial to the pectus ridge. The introducer is passed through the tunnel created by the tonsil clamp with the tip pointed posteriorly and the convexity oriented anteriorly. (b) Once the introducer is in the thoracic cavity, it is turned 180° so that the tip is directed anteriorly. This protects the heart and other mediastinal structures during the dissection. This also utilizes the distal curvature of the introducer to make the turn behind the pectus defect. Courtesy of Dr. Brian Kenney at Nationwide Children’s Hospital.

Fig. 10.3.
Retrosternal dissection. The tip of the introducer is used to progressively dissect the bloodless plane between the posterior surface of the sternum and the pericardium as shown in panels (a) through (c). Note that the tip of the introducer is always directed anteriorly and in view at all times so as to avoid cardiac or pericardial injury.

Fig. 10.4.
Completion of the intrathoracic dissection. (a) With the exit point for the introducer identified, the handle of the introducer is dropped toward the floor, forcing the tip anteriorly through the intercostal space. (b) Once through the chest wall, the introducer is advanced through the left-sided subcutaneous tunnel and delivered through the left lateral incision. (c) Both ends of the introducer are then grasped and lifted to correct the defect and help remodel the chest wall. Courtesy of Dr. Brian Kenney at Nationwide Children’s Hospital.
With the path of the pectus bar defined by the introducer, the ends of the introducer are grasped by the surgeon and assistant and elevated to correct the depression. This facilitates passing the bar and helps to remodel the chest. In cases with severe torsion and asymmetry, a very stiff chest upon elevating the introducer, or a very long defect that still has a residual depression with the introducer, a second bar should be placed. If a second bar is required, performing the more superior dissection and leaving the introducer in place facilitates the second dissection.
An umbilical tape adequate to traverse the length of the pectus bar path is attached to the islet on the end of the introducer and pulled through the thoracic cavity to the right side of the chest. This will act as a guide for the pectus bar as it is delivered through the tunnel. The umbilical tape is detached from the introducer and tied through the islet of the pectus bar . Direct visualization with the camera and guidance from the umbilical tape allows the bar to be advanced through the intrathoracic tunnel. Care should be taken to ensure the bar is placed in the correct orientation corresponding to the preoperative molding. The bar should be passed with the convexity directed posteriorly, and once in place, the left and right sides of the bar should match the laterality of the preoperative molding. Once the bar is in place with the ends directed anteriorly, the bar is flipped 180° using even pressure on both ends of the bar using bar flippers (Fig. 10.5). Once the bar is turned, the defect will reverse and the ends should fall within the incisions. The bar should rest laterally on the muscle and not be too tight or too loose. There should be immediate correction of the defect. If there is a residual defect, a second bar is needed and can be placed above or below the initial bar using the same techniques.


Fig. 10.5.
Flipping the bar. (a) After the bar has been passed through the intrathoracic tunnel, the ends should be directed anteriorly. (b) The bar flippers are placed on either side of the bar. (c) Once the bar flippers are in place, even pressure on both ends will be used to flip the bar 180°, resulting in a correction of the defect. Courtesy of Dr. Brian Kenney at Nationwide Children’s Hospital.
Proper securing of the bar is mandatory to minimize flipping. If the first bar appears loose and unstable, then a second bar is required. Only one stabilizer should be placed for each bar to minimize discomfort with growth. In an adult patient who is done growing, bilateral stabilizers are satisfactory but usually not necessary. The stabilizer slides on either end of the bar, perpendicular to its axis, forming a cross. The subcutaneous flaps can be modified in order to accommodate the stabilizers. Once in place, the stabilizer should be affixed to the pectus bar using any permanent suture. If using two bars, the stabilizers should be staggered. Medial fixation further secures the bar [28]. This can be done by visualizing with thoracoscopy and attaching the bar to the underlying ribs using either an absorbable or permanent suture. The use of an absorbable suture will facilitate bar removal. The passage of the sutures is facilitated by using an Endoclose® needle (Covidien, Norwalk, CT) through the lateral thoracic incision under thoracoscopic guidance. Placing numerous absorbable sutures through all the islets of the bar and stabilizer to the underlying fascia is the final point of fixation (Fig. 10.6).
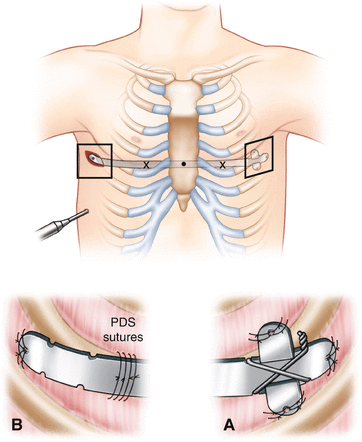

Fig. 10.6.
Bar stabilizer and chest wall fixation. (a) With the bar in place, a stabilizer should be placed on one end. The stabilizer is affixed to the bar with a nonabsorbable suture. The eyelets in both the stabilizer and bar are used for suture fixation to the chest wall usually with an absorbable suture. (b) A third point of fixation is recommended by placing sutures around the bar and rib using thoracoscopic assistance. It is helpful to place these sutures around two separate ribs.
After adequate hemostasis, the lateral incisions are closed in two layers with subcutaneous absorbable suture, followed by a skin closure of choice. Steristrips and a compressive, sterile dressing are placed. Once the incisions are closed, the CO2 is evacuated. This can be performed by cutting the tubing to the trocar and placing it in a basin of sterile water that is below the level of the patient to create a water seal. The evacuation of CO2 is facilitated by placing the patient in Trendelenburg with the left side down and administering multiple positive pressure breaths (Fig. 10.7). The air has been successfully evacuated from the thoracic cavity when there is cessation of air bubbles. The trocar is removed and the incision closed in the same fashion as the two lateral bar incisions.


Fig. 10.7.
CO2 evacuation. A red rubber catheter is threaded through the port and placed in a saline or sterile water-filled basin below the level of the patient to create a water seal as shown here. Alternatively, the insufflation tubing for the port can be cut and used in place of the red rubber catheter. Positive pressure breaths are delivered from anesthesia until the CO2 is evacuated as indicated by cessation of the bubbles. Courtesy of Dr. Brian Kenney at Nationwide Children’s Hospital.
Pearls/Pitfalls
Successful repair of the pectus deformity begins with meticulous attention to the individual patient’s anatomy and appropriate bar molding. Ensure that the anatomic landmarks stated above are utilized for appropriate placement and that the entrance and exit sites are medial to the greatest apex of the pectus ridge. However, if the defect is not appropriately reversed with the initial attempts, there should be no hesitation to place a second bar if needed. The central portion of the convexity should be relatively flat and should not be in a “tabletop” configuration. Creating a prominent apex increases the risk of bar dislodgment and overcorrection by creation of a pectus carinatum deformity. In asymmetric deformities, complete correction may not be achieved; although the bar placement reverses the sternal depression, it may not reverse the sternal rotation which often occurs in these types of defects. Vigorous elevation of the sternum with the introducer and placing a second bar significantly improves asymmetric defects, and the majority will look significantly better. During the intrathoracic portion of the case, finding the bloodless plane between the posterior surface of the sternum and the pericardium is key to avoiding cardiac injury or the less severe pericardial injury. This is best achieved through adequate visualization which can often be hindered by the more severe defects. Visualization can be improved by either placing a second camera port in the left chest if needed or through sternal elevation. Sternal elevation can be achieved by multiple techniques that have been described elsewhere [25–27]. Some have also suggested the use of a laparoscopic dissector in lieu of the Biomet introducer to dissect in the retrosternal space as it offers more fine and directed dissection [29].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


