Malignant
Benign
Surface epithelial-stromal tumors
Mucinous cystadenocarcinoma
Serous cystadenocarcinoma
Adenofibroma
Adenocarcinoma
Sex cord-stromal tumors
Granulosa cell tumors
Theca cell tumors
Fibromas
Sclerosing stromal tumors
Sertoli-Leydig cell tumors
Sex cord tumors with annular tubules
Steroid cell tumors
Germ cell tumors
Dysgerminoma
Endodermal sinus tumors
Embryonal carcinomas
Choriocarcinomas
Teratomas
Mixed germ cell tumors
Follicular cysts
Corpus luteum cysts
Paraovarian cysts
Serous cystadenoma
Endometriosis
Gonadoblastomasa
Torsionb
Preoperative Evaluation
Physical Exam
Ovarian cysts have a variety of presentations and symptoms. During the neonatal period, they are usually identified prenatally on US as a cystic mass or postnatally with abdominal fullness and presence of a mass. Older patients usually present with abdominal pain and/or fullness that is either acute or chronic. Sometimes the cysts are found on routine physical examination as a mass in the lower abdomen. Torsion usually presents as sudden onset of acute, sharp, or colicky lower abdominal pain (usually the right side) lasting less than 48 h. Nausea and vomiting are usually associated with the pain [2].
Malignant neoplasms can present with symptoms similar to cysts and torsion. Abdominal enlargement can occur from the mass, ascites, or a combination of both. Pain may be present. If the neoplasm produces hCG, there may be a history of abnormal vaginal bleeding or precocious puberty [3]. Likewise, pregnancy symptoms may present if hCG is produced. A functional lesion may present similar to other ovarian pathology. Acute or chronic pain is usually present, however some present with painless abdominal enlargement. Precocious puberty or virilization (increased muscle strength, acne, hirsutism, frontal hair thinning, deepening of the voice) may occur if androgen production is high [4].
Labs
For benign lesions, laboratory markers can vary and do not directly help in diagnosis. For torsion, the patient may have leukocytosis, elevated lactate, or electrolyte imbalances. Any lesion suspicious for malignancy should have tumor markers evaluated including alpha-fetoprotein, LDH, CA-125, hCG, CEA, LH, FSH, and estrogen levels [5, 6].
Imaging
Ovarian cysts can be diagnosed by ultrasound examination, even in the prenatal population [7]. Although used regularly, ultrasound has some limiting factors: it is operator dependent and can be influenced by patient weight and age (Fig. 48.1). Transvaginal ultrasound is preferred in older patients as it can better visualize adnexal lesions.
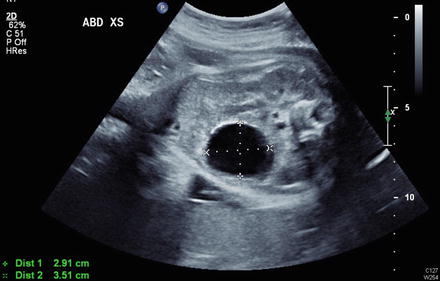

Fig. 48.1.
Ultrasound showing a benign simple, right ovarian cyst. Notice the homogeneity and anechoic nature of the cyst. (Courtesy of Robert Weinsheimer, MD, Swedish Medical Center, Seattle, WA).
If there should be a concern for malignancy or for larger lesions, then evaluation with cross-sectional imaging such as CT or MRI is indicated (Fig. 48.2).


Fig. 48.2.
MRI showing a large ovarian benign, simple cyst. Notice the lack of septations and areas of heterogeneity. (Courtesy of Robert Weinsheimer, MD, Swedish Medical Center, Seattle, WA).
Surgical Indications and Controversies
Ovarian Cyst
For simple, small ovarian cysts, most favor close monitoring. Cysts diagnosed in utero are monitored with serial ultrasounds. These cysts typically regress spontaneously and do not require any intervention. If leading to other complications during pregnancy, in utero aspiration is an option but comes with some risk. Postnatally, lesions are followed closely with serial imaging until the cyst has fully resolved or requires intervention. If the cyst grows, is complex, or does not regress, then intervention is warranted. Aspiration of simple cysts greater than 4 or 5 cm is possible; otherwise surgical excision is preferred. Larger cysts are prone to, or may have already undergone, torsion [8].
For simple cysts outside of neonatal populations, usually no intervention is necessary. If they are large or growing, simple aspiration can be performed. If the cysts are >5 cm, complex, or leading to symptoms, then surgical excision is warranted (Fig. 48.3). In every case where malignancy is not suspected or involved, ovarian-sparing excision should be considered.


Fig. 48.3.
Gross specimen of large ovarian cyst. Note that even benign lesions can grow quite large. (Courtesy of Ian Mitchell, MD, San Antonio, TX).
Ovarian cysts greater than 10 cm, as with large teratomas, can also be challenging to remove. Spillage, domain, and removal of the cyst from the peritoneal cavity are some of the main concerns when developing an operative plan. If imaging shows no concern for malignancy, then laparoscopic techniques can be used [9].
Ovarian Torsion
Ovarian torsion is considered a surgical emergency in effort to save the ovary. There is an increasing favor to detorse and leave the ovary with postoperative surveillance ultrasounds at designated intervals. This is a departure from the historical management, which consisted of oophorectomy with or without salpingectomy. Commonly a mass or cyst is associated with the torsion, and it can be difficult to interpret where the mass ends and the ovary begins (Fig. 48.4). As a result, it can be difficult to separate the ovary from the mass, and trying to dissect the two free could cause damage to the ovary. In addition, many cysts associated with torsion are functional cysts and can be treated without resection, as they will resolve on their own [10]. An ovary that does not appear viable after detorsion, if left to remain, can be viable in future US surveillance. At follow-up US, if there is a persistent mass, then removal may be warranted and is still a consideration [11].


Fig. 48.4.
Intraoperative findings of a torsed right ovary and associated large cystic lesion originating from right fallopian tube. (Courtesy of Robert Weinsheimer, MD, Swedish Medical Center, Seattle, WA).
There is no good prospective data to support the use of ovariopexy and its practice appears to be surgeon dependent [12]. Some specific situations may warrant ovariopexy, such as patients undergoing pelvic radiation for a malignancy, bilateral torsion, or recurrent ipsilateral torsion may benefit from a pexy procedure. In addition, pexy may be beneficial if torsion occurs on an ovary with a malformed or excessively long utero-ovarian ligament or in a patient with a single ovary. Clipping the utero-ovarian ligament or infundibulopelvic ligament to the pelvic sidewall or posterior uterus may also serve the same purpose as a pexy.
Teratoma/Malignancy
For malignant lesions, surgical excision is the preferred treatment. This is both diagnostic and therapeutic. In most cases, the extent of the operation depends on intraoperative findings.
Historically, large ovarian tumors over 10 cm in diameter have been removed by laparotomy due to concern for malignancy and risk of spread via rupture or peritoneal seeding. There are arguments that laparoscopy has no role in any lesion over 15 cm, but despite this, laparoscopy is being used more often to approach these lesions [13]. Imaging and tumor markers will aid in determining if the tumor is an appropriate candidate for laparoscopic resection. The goal remains to remove the lesion en bloc without spillage which can upstage the tumor. Spillage rates for ovarian cystectomies can reach upward of 25 % during laparoscopy for experienced surgeons [14]. As a result, techniques have been developed to minimize this risk.
Operative Considerations
Anesthesia
It is important to have an anesthesia team familiar with minimally invasive surgery in the pediatric population. General anesthesia should be used in all laparoscopic cases. Prophylactic antibiotics such as cefazolin (first-generation cephalosporin) or some similar antibiotic should be given.
Room Setup
Viewing towers should be optimally arranged to allow the surgeon and assistant to comfortably perform the operation. A screen is placed at the patient’s feet. The surgeon will be on the patient’s left side facing the feet and assistant will be on the opposite side holding the camera. The scrub nurse will be next to the surgeon. The anesthesiologist is at the head of the bed.
Positioning
The patient is in supine position, with padding on bony prominences. The patient is placed as far down the bed as possible, so the distal part of the surgical bed does not get in the way of towers or viewing monitors. The arms are tucked on both sides to allow for more operating freedom. A Foley catheter is placed to keep the bladder from interfering in the operative field. Trendelenburg position will help with visualization of the pelvic organs.
Laparoscopic Settings
The insufflation setting is based on the patient’s age and surgeon’s preference. An intraperitoneal pressure of 15 mmHg is usually tolerated by most healthy pediatric patients who weigh more than 5 kg. Intraperitoneal pressures of more than 20 mmHg can lead to decreased venous return and ventilator issues. If the patient is less than 5 kg, an intraperitoneal pressure of 8–12 mmHg is used.
Instrumentation
Standard laparoscopic instruments of appropriate size, either 3- or 5-mm, are sufficient for laparoscopic ovarian procedures. Devices such as monopolar cautery hook or scissors, a sealing device, or ultrasonic energy device can be chosen based on surgeon preference. A 3-mm or 5-mm 30-degree scope is optimal for visualization. Use of blunt graspers will avoid injury to the ovary or surrounding structures. In neonates and smaller patients, 3-mm trocars, instruments, and camera may be used. There is a 3-mm sealing device that is available that is helpful in the neonatal population. If a stapling device will be used, it is possible to use a 5-mm stapler, but otherwise consider which 5-mm port may be upsized to a 12-mm port to allow this if necessary. There are both 5-mm and 10-mm endoscopic specimen bags which can be used.
Trocar Site Placement
The types of trocars used are based on surgeon preference. There are 3- or 5-mm trocars available. The abdominal wall in this population is thin and much more compliant than adults and is an important consideration when placing trocars. Local anesthetic should be used at all trocar sites. A cutdown technique can be used to place the initial trocar in the umbilicus, or a Veress needle with dilatable expandable trocars can be used safely. Once the peritoneal cavity is accessed, additional trocars can be placed under direct vision in a triangulated position to optimize working conditions. The location of the lesion will dictate where the trocars are placed, and with pelvic neoplasms, the trocars sites will usually be mid abdomen or cephalad to the umbilicus.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


