Bacterial Vaginosis (Formerly Gardnerella or Anaerobic Vaginosis)
This is when the normal lactobacilli are overgrown by a mixed flora including anaerobes, Gardnerella and Mycoplasma hominis. It is found in 12% of women, but why it occurs is poorly understood. A grey–white discharge is present, but the vagina is not red or itchy. There is a characteristic fishy odour from amines released by bacterial proteolysis. The diagnosis is established by a raised vaginal pH, the typical discharge, a positive ‘whiff’ test (fishy odour when 10% potassium hydroxide [KOH] is added to the secretions) and the presence of ‘clue cells’ (epithelial cells studded with Gram-variable coccobacilli) on microscopy. Treatment of symptomatic women is with metronidazole or clindamycin cream. These bacteria can cause secondary infection in pelvic inflammatory disease (PID; [→ p.77]). There is also an association with preterm labour [→ p.202].
Infection Associated with Foreign Bodies
Infection and discharge in children is often due to a foreign body. Sexual abuse must also be considered, but discharge is more often due to atrophic vaginitis due to low oestrogen levels. Toxic shock syndrome usually occurs as a rare complication of the retained, particularly hyperabsorbable, tampon. A toxin-producing Staphylococcus aureus is responsible: a high fever, hypotension and multisystem failure can occur. Treatment is with antibiotics and intensive care.
Sexually Acquired Infections
Principles in the Management of STIs
Screening for concurrent disease is important because more than one STI may be present.
The regular sexual partner should be treated and screened for other infections.
Partner notification (contact tracing) involves identification and contacting recent sexual contacts, for screening and treatment. This is usually performed by the patient.
Confidentiality should be maintained. The doctor is breaching confidentiality if he/she informs sexual contacts of his/her patient of her diagnosis without her permission. Sexually transmitted infections can occur within monogamous relationships (e.g. genital herpes following orogenital sex). The diagnosis of an STI is emotive and patients need to be handled sensitively and with adequate explanation.
Education:
Frequently changing partners increases the risk of acquiring STIs, including human immunodeficiency virus (HIV).
Barrier methods of contraception greatly reduce the risk of acquiring STIs, including HIV.
Chlamydia
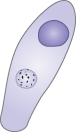
Chlamydia trachomatis is a small bacterium (Fig. 10.2) and is now the most common sexually transmitted bacterial organism in the developed world. Some 5–10% of women aged 20–30 years have been infected. This is usually asymptomatic, but urethritis and a vaginal discharge can occur. The principal complication is pelvic infection, which may also be silent. This can cause tubal damage leading to subfertility and/or chronic pelvic pain. Chlamydia infection also causes Reiter’s syndrome, characterized by a triad of urethritis, conjunctivitis and arthritis. Nucleic acid amplification tests (NAATs), e.g. polymerase chain reaction (PCR), are best and can be used on urine for screening purposes. Treatment is with azithromycin or doxycycline.
Gonorrhoea
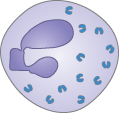
This is caused by Neisseria gonorrhoeae, a Gram-negative diplococcus (Fig. 10.3). It is common, particularly in the developing world. It is commonly asymptomatic in women, although vaginal discharge, urethritis, bartholinitis and cervicitis can occur and the pelvis is commonly infected. Men usually develop urethritis. Systemic complications include bacteraemia and acute, usually monoarticular, septic arthritis. Diagnosis is from culture of endocervical swabs; NAAT tests are also available but should be followed by culture if positive to check antibiotic sensitivities. Antibiotic resistance is increasing, including to ciprofloxacin, and IM ceftriaxone (or oral cefixime) is usually required. Partner notification and treatment are essential.
Genital Warts (Condylomata Acuminata)
These are caused by the human papillomavirus (HPV). They are extremely common. Appearances vary from tiny flat patches on the vulval skin to small papilliform (cauliflower-like) swellings. Warts are usually multiple and may affect the cervix, where certain oncogenic types (mostly 16 and 18) are associated with the development of cervical intraepithelial neoplasia (CIN; [→ p.33]). Treatment is with topical podophyllin or imiquimod cream (external warts only). Cryotherapy or electrocautery is used for resistant warts. There is a high recurrence rate (up to 25%). A vaccine against HPV is now administered to adolescent girls [→ p.33] for the purpose of preventing cervical neoplasia.
Genital Herpes
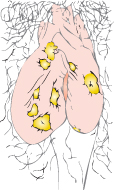
Genital infection is mostly with the herpes simplex virus (HSV) type 2, although type 1, the cause of cold sores, is increasingly implicated (Fig. 10.4). The primary infection is the worst, with multiple small painful vesicles and ulcers around the introitus. Local lymphadenopathy, dysuria and systemic symptoms are common; secondary bacterial infection, aseptic meningitis or acute urinary retention are rarer. The virus then lies dormant in the dorsal root ganglia: in about 75% of patients reactivations occur. These attacks are less painful, less severe, and often preceded by localized tingling. The diagnosis is established from examination and with viral swabs. Aciclovir (also valaciclovir or famciclovir) is used in severe infections and will also reduce the duration of symptoms if started early in a reactivation. Neonatal herpes has a high mortality and can be prevented [→ p.165].
Syphilis
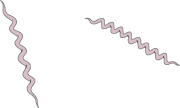
Infection by the spirochaete Treponema pallidum (Fig. 10.5) is common in the developing world, and although relatively rare in developed countries the incidence is rising in the UK. Primary syphilis is characterized by a solitary painless vulval ulcer (chancre). Untreated, secondary syphilis may develop weeks later, often with a rash, influenza-like symptoms and warty genital or perioral growths (condylomata lata). At this stage the spirochaete infiltrates other organs and can cause a variety of symptoms. Latent syphilis follows as this phase resolves spontaneously. Primary or secondary syphilis during pregnancy carries a high risk of congenital infection. Tertiary syphilis is now very rare. It develops many years later and virtually any organ can be affected. Aortic regurgitation, dementia, tabes dorsalis and gummata in skin and bone are the best-known complications. A variety of diagnostic tests are used (including enzyme immunoassay (syphilis EIA) and Venereal Disease Research Laboratories (VDRL) test). Treatment of all stages is with parenteral (usually intramuscular) penicillin.
Trichomoniasis
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree