Chapter 193 Cholera
Epidemiology
The first 6 cholera pandemics originated in the Indian subcontinent and were caused by classical O1 V. cholerae. The seventh pandemic is the most extensive of all and is caused by V. cholerae O1 El Tor. It began in 1961 in Sulawesi, Indonesia, and has spread to the Indian subcontinent, Southeast Asia, Africa, Oceania, Southern Europe, and the Americas. In 1991, V. cholerae O1 El Tor first appeared in Peru before rapidly spreading in the Americas. Cholera becomes endemic in areas following outbreaks when a large segment of the population develops immunity to the disease after recurrent exposure. The disease is now endemic in parts of East, Southern, and Northwest Africa, as well as in South and Southeast Asia (Fig. 193-1).
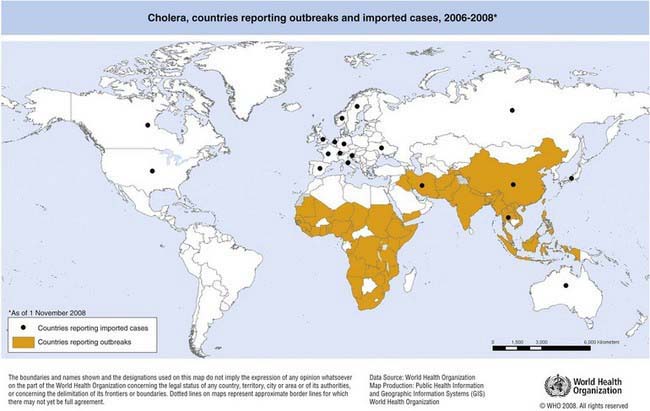
Figure 193-1 Countries reporting cholera outbreaks and imported cholera cases to WHO from 2006-2008.
(From World Health Organization: Cholera, areas reporting outbreaks, 2007-2009 (website). gamapserver.who.int/mapLibrary/Files/Maps/Global_ChoeraCases_ITHRiskMap.png. Accessed August 9, 2010.)



