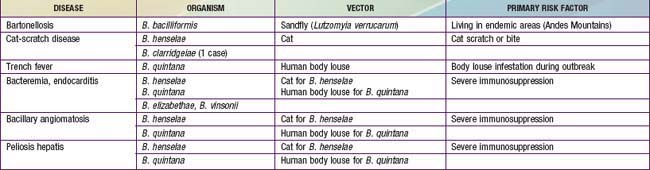
Chapter 201 Bartonella
The spectrum of disease resulting from human infection with Bartonella species includes the association of bacillary angiomatosis and cat-scratch disease (CSD) with Bartonella henselae. Six major Bartonella species are pathogenic for humans: B. henselae, Bartonella quintana, Bartonella bacilliformis, Bartonella elizabethae, Bartonella vinsonii, and Bartonella clarridgeiae (Table 201-1). Several other Bartonella species have been found in animals, particularly rodents and moles.
201.1 Bartonellosis (Bartonella bacilliformis)
Clinical Manifestations
In the pre-eruptive stage of verruca peruana (Fig. 201-1), patients may complain of arthralgias, myalgias, and paresthesias. Inflammatory reactions such as phlebitis, pleuritis, erythema nodosum, and encephalitis may develop. The appearance of verrucae is pathognomonic of the eruptive phase. Lesions vary greatly in size and number.
Prevention
Prevention depends on avoidance of the vector, particularly at night, by the use of protective clothing and insect repellents (Chapter 168).
201.2 Cat-Scratch Disease (Bartonella henselae)
Clinical Manifestations
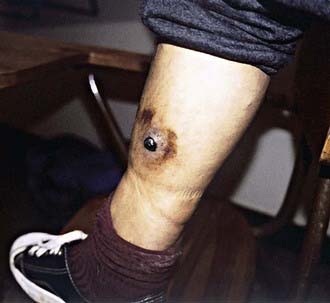
After an incubation period of 7-12 days (range 3-30 days), 1 or more 3- to 5-mm red papules develop at the site of cutaneous inoculation, often reflecting a linear cat scratch. These lesions are often overlooked because of their small size but are found in at least 65% of patients when careful examination is performed (Fig. 201-2
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree