Dehydration
Water accounts for up to 80% of an infant’s weight. Loss of more than 5% of this water represents significant dehydration. Fluid may be depleted in the intracellular or extracellular compartments. If significant fluid is lost acutely from the intravascular part of the extracellular space, then shock may ensue. Normal body fluid is a balance between intake (drinking) and output (urine output, stool volume, sweat and insensible losses such as expiration). If intake does not keep up with losses, then the child becomes dehydrated. The commonest cause of dehydration in children is diarrhoea and vomiting due to gastroenteritis.
Acute Diarrhoea
Episodes of acute diarrhoea are common in children, and are usually due to infection, although not always gastrointestinal (GI) infection. Dehydration due to gastroenteritis is sadly still a major cause of mortality in children in developing countries. Gastroenteritis is usually viral, and rotavirus is the main agent causing winter epidemics. Diarrhoea follows 1–2 days after low-grade fever, vomiting and anorexia. There may be acute abdominal pain and malaise. The diarrhoea resolves within a week and the management is adequate rehydration (see below). Bacterial gastroenteritis has a similar presentation and the common pathogens are Escherichia coli, shigella, salmonella and campylobacter. Meningism and febrile convulsions can occur with shigella, whilst bloody diarrhoea occurs in shigella and campylobacter infection.
Any infection or febrile illness can cause diarrhoea, especially in infants. This includes viral URTIs, chest infections, otitis media and UTI. Use of antibiotics may cause diarrhoea due to a disturbance of the normal enteric flora. Recurrence of diarrhoea on refeeding is most likely to be due to lactase deficiency and may require a lactose-free diet for a number of weeks.
Antibiotics should not be prescribed for uncomplicated gastroenteritis. Antiemetics and antimotility agents are not generally recommended. If there is evidence of septicaemia the child should be admitted for intravenous antibiotics. There is some evidence that the use of probiotics (e.g. lactobacillus species) may reduce the duration of diarrhoea. Breast-feeding should be continued whenever possible.
Management of Dehydration
Try to determine the cause of the diarrhoea and the degree of dehydration. Ask about the duration of diarrhoea, whether there has been vomiting and when the child last passed urine.
The degree of dehydration can be assessed by the pulse, blood pressure, mucous membranes, urine output, skin turgor and by feeling the fontanelle (see box opposite).
In mild dehydration the only physical sign may be a dry mouth. ‘Red flag’ warning signs that may indicate likely progression to shock include sunken eyes, altered responsiveness, tachycardia, tachypnoea and reduced skin turgor (pinch test).
The child should be weighed, the difference between the weight at presentation and a recent weight can be used to estimate the volume of body water that has been lost (1 kg = 1 L). If the child is significantly dehydrated, blood should be taken for urea, electrolytes and bicarbonate and interpreted as in the table:
| Finding | Interpretation |
| Metabolic acidosis | Bicarbonate loss in diarrhoea or shock with lactic acidosis |
| Metabolic alkalosis | Loss of H+ ions from persistent vomiting in pyloric stenosis. |
| Hyponatraemia | Dehydration where diarrhoea contains high concentration of sodium ions. When Na+ < 130 mmol/L the child is often lethargic and the skin feels dry and can be pinched into creases |
| Hypernatraemia | Dehydration where there is greater loss of water than sodium ions or excessive salt intake or excessively concentrated formula feeds. When Na+ > 150 mmol/L the child is very thirsty and the skin may feel doughy. |
Calculating the replacement and maintenance fluid requirements for intravenous rehydration
An infant weighing 7.5 kg is thought, on the basis of clinical examination, to be 10% dehydrated.
(A) If we assume the child is all water then 7.5 kg water = 7500 mL. 10% of this is 750 mL (fluid deficit).
(B) Maintenance fluids = 100 mL/kg per day for the first 10 kg of body weight, 50 mL/kg for next 10 kg and 20 mL/kg thereafter.
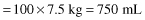
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


