10 Postnatal care
Postnatal Care—What Should it Entail?
What is the normal course of events for women in the postpartum period?
With the increasingly prevalent phenomenon of early discharge after childbirth, GPs must be cognisant of the normal physiological changes that occur in women in the first days/weeks postpartum. These are listed in Box 10.1.
BOX 10.1 What to expect in the first days/weeks of the postpartum period
Uterus
Lochia
Cervix and vagina
Why has the traditional postnatal visit been set at 6 weeks?
Traditionally women have been instructed to return to see their obstetrician 6 weeks after their baby’s birth.1 At this appointment the practitioner usually inquires about breastfeeding, undertakes an abdominal and vaginal examination and advises the woman about contraception. The focus of this visit has been to ensure that ‘things have returned to normal’. This form of postnatal care however, devotes time and resources to routine examinations that screen for morbidities that are no longer the major health burden for women2 and does not necessarily address the needs of women at this time. The content and timing of postnatal care therefore needs to be reviewed.3
What postnatal problems commonly arise?
There are high levels of maternal morbidity after childbirth. One study has documented that 85% of women report at least one health problem 2 weeks after childbirth, and 12–18 months later 76% of women are still suffering from at least one problem.4 The common problems encountered by women in the postnatal period5 are listed in Box 10.2.
Despite the fact that more than 90% of women attend a postnatal check-up,6 they are unlikely to raise problems such as back pain, urinary incontinence, depression, haemorrhoids and perineal pain with their doctor.7 They are also unlikely to discuss sexual problems, which are common after childbirth. While only 15% of women report these problems to a health professional, some 83% experience sexual problems in the first 3 months after delivery. This declines to 64% at 6 months but does not reach the pre-pregnancy level of 38%.8 Common problems include vaginal dryness, painful penetration, pain during intercourse, pain on orgasm, vaginal tightness, vaginal looseness, bleeding/irritation after sex and loss of sexual desire.
What advice can a GP give to women about weight gain or weight loss in the postpartum period?
In the USA about 50% of women are either overweight or obese (body mass index >25).9 For many of these women their weight gain occurred with each pregnancy. Advice may therefore be sought from a GP about weight loss in the postpartum period. While many women expect to lose weight while breastfeeding, the reality is that weight loss during lactation is very variable. On average women can expect to lose between 0.6–0.8 kg per month, but the range is between 5.6 kg loss and 5.5 kg gain per month.10
Some researchers are concerned that if women deliberately try to lose weight while they are lactating, the growth of their infant may be compromised.11 However, a recent study has shown that maternal loss of 0.5 kg per week induced by dieting and exercise did not affect infant growth.12
How should postnatal care be delivered?
How exactly postnatal care should be delivered in order to optimise maternal and child health remains debatable. Simply bringing the timing of the postnatal visit forward to 1–2 weeks postpartum does not bring about improved outcomes.13 Midwife-led, flexible postnatal care tailored to the needs of the individual was shown in a study to help to improve women’s mental health but not their physical health.2
Recent UK guidelines have identified the essential core (routine) care that every woman and her baby should receive in the first 6–8 weeks after birth.14 Key priorities of these guidelines are:
TABLE 10.1 Signs and symptoms of potentially life-threatening conditions
| Signs and symptoms | Condition |
|---|---|
| Postpartum haemorrhage | |
| Infection | |
| Pre-eclampsia/eclampsia | |
| Thromboembolism |
(From National Institute of Clinical Excellence14)
When women do present to their GP in the postnatal period, the presenting complaint should be addressed first, but then the GP should focus on the following issues14:
Summary of key points
Common Breastfeeding Problems and Issues
How does a mother know if the baby is getting enough milk?
Mothers should be advised that the baby is getting enough milk if:
What common breastfeeding problems present to the GP?
Most women have made the decision whether or not to breastfeed prior to the birth of their baby. While breastfeeding is initiated in hospital, many women are discharged before their milk ‘comes in’ (day 3–5 post-delivery). With the increasing trend towards early discharge, GPs are faced with the whole range of breastfeeding problems, which are summarised in Box 10.3.
What are the causes of nipple pain?
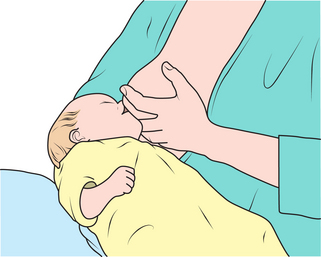
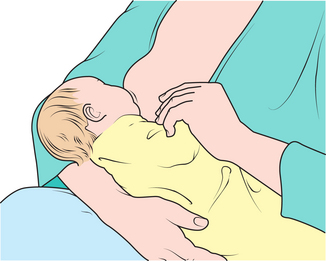
The best way to assess if a woman is feeding her baby correctly is to observe her latching the baby on and feeding (Figs 10.1 and 10.2).
In advising a mother about correct technique, the following should be covered15:
A plethora of agents are suggested to ease nipple pain, but a recent systematic review showed that no one topical agent showed superior results in the relief of nipple discomfort.16 The most important factor in decreasing the incidence of nipple pain was the provision of education in relation to proper breastfeeding technique and latch-on.
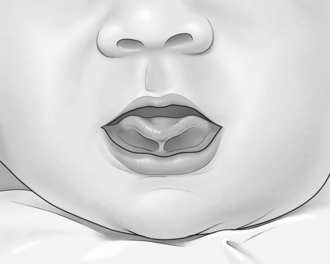
Dummies and teats may be contributing to the problem, as they encourage an incorrect sucking action (different from that used at the breast) and are best discouraged at least until breastfeeding is established. Other factors that may be contributing to nipple pain are listed in Box 10.4, while Box 10.5 lists indicators of good attachment and successful breastfeeding.
BOX 10.4 Factors contributing to nipple pain
How do I know if the cause of the nipple pain is candidiasis?
Breastfeeding women with these symptoms have been shown to be significantly more likely than other breastfeeding women to grow Candida from their nipples.17 A swab of the nipple, however, is not a useful diagnostic test for this condition, as the sensitivity of the test is very low. Other symptoms of thrush could include rash and pruritus of the nipple and areola.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree