The active total care of a patient’s mind, body, and spirit, including:
Managing distressing symptoms
Establishing goals of care
Facilitating decision-making and advance care planning
Providing additional psychosocial and/or spiritual support
Facilitating home-based care including hospice
Providing bereavement support for families
“Palliative care” refers to the active total care of a patient’s body, mind, and spirit and therefore strongly complements the whole patient psychosocial care (WHO 2014). Although the term “palliative care” historically referred to care specific to patients at the end of life, its current definition is more holistic; it begins when illness is diagnosed and continues regardless of whether or not a child receives disease-directed treatment (WHO 2014). Pediatric palliative care (PPC) has emerged as both an approach and a medical subspecialty that improves the quality of life of patients and families facing the problems associated with life-threatening illness through prevention and relief of suffering (Fig. 14.1) (Wolfe and Sourkes 2011). Effectively integrating palliative care into the care of children with cancer requires a broad interdisciplinary perspective that includes the family and also makes use of available local and community resources. It may be provided in tertiary care facilities, community health centers, and children’s homes.
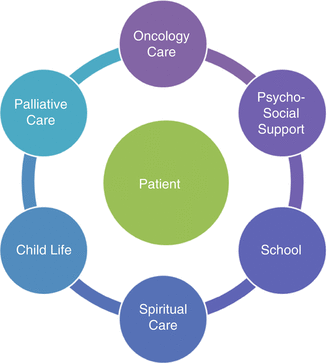

Fig. 14.1
Model of pediatric palliative care approach and specialty. Palliative care approach refers to interdisciplinary patient care that recognizes and meets the needs of the whole patient. Palliative care subspecialty teams fit within this approach and provide additional expertise (e.g., pain and symptom management, decision-making support, and/or advance care planning)
Pediatric oncology care necessarily involves an interdisciplinary team, typically consisting of physicians, nurses, and psychosocial clinicians, as well as child life specialists, educators, chaplains, physical therapists, and subspecialty medical teams, depending on patient and family needs. While each member of the team has discipline-specific roles, all members are responsible for providing a steady presence, anticipatory guidance, assessment and relief of child and family distress, and response to questions and concerns. Palliative care teams also consist of multiple disciplines and provide additional perspective and skill, especially when prognosis is uncertain. PPC providers are trained to help children and families make choices consistent with their values and overall goals of care. They also have expertise in complex pain and symptom management, decision-making, and enabling patient quality of life despite the inherent restrictions of their illness.
The role and involvement of palliative care change over time. Early integration of oncology and PPC may facilitate patient and family adjustment, support, and comprehension of complicated and/or high-risk treatment plans. Later roles may include decision-making support for patients with poor prognoses, exploring overall goals of care, coordinating outpatient hospice care, and providing ongoing bereavement support.
For example, children with advanced cancer have high degrees of symptom burden and suffering from both physical and emotional causes (Wolfe et al. 2000a). Prognostic uncertainty is prevalent and patients’ parents may be highly distressed (Rosenberg et al. 2013). For the more than 2000 children in the United States who die from their cancer each year (Onelov et al. 2007; Ries Lag et al. 1999), the anticipated time until death and how one should spend this time are often unclear. Clinical experience suggests that patients with some forms of incurable cancer may live for months to years; whereas others may be expected to die within weeks. All of these factors may inhibit mindful family decision-making and patient and family quality of life.
The empirical benefits of integrated palliative care include optimal pain and symptom management; better understanding of patient and family goals, values, and beliefs; stronger psychosocial and spiritual care; and improved patient and family quality of life. Many of these have been confirmed in the adult oncology literature. Among adults with terminal lung cancer, for example, palliative care has been associated with fewer physical symptoms, improved mood, and more accurate perceptions of prognosis. Patients who received standard oncology care integrated with palliative care survived longer than those who received oncology care alone, refuting presumptions that inclusion of palliative care would necessarily shorten patient’s life expectancies (Temel et al. 2010). Multiple studies have suggested that palliative care involvement is associated with improved management of distressing symptoms, better communication, earlier recognition of prognosis, and fewer hospitalizations among other adult oncology populations (Greer et al. 2012; Bakitas et al. 2009; Epstein and Morrison 2012).
However, few studies have been conducted in pediatric oncology populations, and formal evidence of these benefits is sparse. In a study of over 24,000 children who died more than 5 days following an admission to a children’s hospital, only 4 % received formal palliative care consultations. Those that did receive PPC consultations had fewer days in the hospital before death, received fewer medications, and were less likely to have invasive interventions or die in an intensive care unit (Keele et al. 2013). In pediatric oncology settings, increased focus on palliative care has resulted in improved advance care planning, including better preparation for end-of-life experiences and decreased pain among patients with advanced cancer (Wolfe et al. 2008).
Integrating palliative care into routine care for patients with advanced cancer is becoming more common in medical oncology settings but is unfortunately inconsistent in pediatric centers. Only 58 % of Children’s Oncology Group institutions report having a formal PPC team (Dalberg et al. 2013; Johnston et al. 2008). Therefore, psychosocial clinicians may be responsible and have the opportunity to integrate the concepts of PPC into their care for children with cancer and their families. This PPC-inclusive approach provides a support system to help patients live as actively and as wholly as possible until death and to help families cope throughout the illness experience, bereavement, and beyond.
Caring for Children with Prognostic Uncertainty
Case Vignette
Jonah was 17 years old when his acute lymphoblastic leukemia came back for the first time. His doctors recommended a hematopoietic stem cell transplant (HSCT) as a potential curative option and explained that Jonah’s disease was high risk and that chances for cure were less than 30 %.
Jonah and his family decided to proceed with the transplant. “Of course we would try it,” said Jonah later. “I wanted to live, and 30 % was still good enough odds.” During his months of treatment and recovery, he and his family remained optimistic he would survive, although each privately struggled with the angst of “what if it comes back?”
Unfortunately, Jonah’s leukemia did come back. This time his doctors said his chances for cure were less than 5 %. “I didn’t know what to do the second time around,” he explained. “All of a sudden, the odds were really low. Part of me felt like the numbers couldn’t be right and I should keep fighting, but another part said ‘that’s not how I want to live.’”
During the ensuing discussions, providers asked Jonah to articulate how he did want to live. As he came to understand that being home with his friends and family was most important to him, the decisions became more clear. “We decided to go with some oral chemotherapy that would slow the leukemia down, but not keep me in the hospital,” he explained. “It took time for us to accept it, and there were times when I still couldn’t. But we kept talking about my options, my goals, what my family hoped for, what mattered to us. That helped.”
Prognostic Understanding and Communication
Several studies over the past decade have shown that there are discrepancies between physician and parent understanding of their child’s cancer prognosis, both at diagnosis and when the illness is more advanced. For example, Wolfe et al. showed that providers tend to recognize the child as having no realistic chance for cure approximately 100 days before families do and approximately 200 days prior to the patient’s death (Wolfe et al. 2000b). While this may be unsurprising (health-care personnel have prior training and experience recognizing incurable cancer), the discrepancy in recognition remains a critical issue in providing appropriate psychosocial care for patients and families. It is important that providers communicate to families when cure is unlikely as it influences when discussions regarding advance care goals and “do not resuscitate” (DNR) plans occur, with earlier communication leading to earlier discussions. Likewise, patients and families are more likely to endorse goals of “lessening suffering.” Parents are then more prepared for their child’s ultimate death, and physicians perceive the child’s death as more peaceful (Wolfe et al. 2000b; Maurer et al. 2010).
In contrast, when parents are unaware of their child’s impending death, children are more likely to die in the ICU and to receive cure-directed therapy that may impair their overall quality of life (and quality of death) (Valdimarsdottir et al. 2007). Parents with less time to prepare for their child’s death are more likely to have long-term psychological morbidities (Valdimarsdottir et al. 2007; Lannen et al. 2008), poor physical health, and poor quality of life (Jalmsell et al. 2011). These findings suggest that effective parent-provider communication and promotion of concordance regarding prognosis and goals of care will improve patient and family experiences. Unfortunately, doing so is challenging.
Barriers to End-of-Life Communication
Parent Factors
Parents of children with cancer tend to be more optimistic than their providers regarding the likelihood of cure both at the time of diagnosis (Mack et al. 2007a) and when cancer progresses or recurs (Mack et al. 2008; Rosenberg et al. 2014b). Parents with less education tend to have disproportionately poorer concordance with their medical team regarding cure likelihood (Rosenberg et al. 2014b; Mack et al. 2007a). However, no studies (to date) have included sufficient numbers of participants to fully explore other demographic or cultural determinants of parent perspectives. Furthermore, evidence suggests that parents may not be willing to formally endorse their child’s impending death (Rosenberg et al. 2014a). When parents of children with advanced cancer were asked what actions supported them in good parenting, they reported that knowing “all that can be done is being done” was the most important way that health-care professionals could support them (Hinds et al. 2009). Yet, in retrospect, parents may experience some decisional regret, especially when children experience high degrees of physical or emotional suffering at the end of life (Mack et al. 2008).
Relational Factors
In retrospect, bereaved parents endorse relational aspects of care as indicators of high quality care. Specifically, higher parent ratings of physician care were associated with physicians giving clear information about what to expect in the end-of-life period, delivering information sensitively, speaking directly with the child, and preparing the parent for the child’s death (Mack et al. 2005). In contrast, parents who become aware of their child’s impending death during his last 24 hours report poorer communication and less satisfaction with their medical teams (Valdimarsdottir et al. 2007). Likewise, siblings of children with cancer are at greater risk for poor adjustment and long-term morbidities when they are not included in end-of-life discussions or preparation (Rosenberg et al. 2015). It follows that good communication is a key component of parent satisfaction and quality of care. See Chapter 2 for more information about communication.
Medical Factors
Parent-provider concordance also may be associated with specific cancer types or medical interventions. For example, parents of children with leukemia have reported shorter awareness times prior to their child’s death than parents of children with other types of cancer (Valdimarsdottir et al. 2007). Similarly, the first documentation of a child’s unlikely cure is approximately 4 days prior to death for children on hematopoietic stem cell transplant (HSCT) services, compared to 84 days prior to death for children receiving standard hematology/oncology care (Ullrich et al. 2010a). These observations provide opportunities for intervention and suggest that families of children undergoing HSCT may need additional communication and decision-making support.
Medical Provider Factors
Among oncology providers, personal distress may create a barrier to end-of-life communication. A majority of pediatric oncologists find breaking bad news highly stressful. Nearly a quarter of pediatric oncologists say it is “the worst part of the job,” and more than half feel a personal sense of failure when cure is no longer possible (Hilden et al. 2001). Another barrier may be that providers wish not to “take away hope” or contribute to additional patient and parent distress. There is no evidence that open and realistic discussions of prognosis do either (Mack and Smith 2012). Rather, parents who know their child’s anticipated trajectory are better able to cope and make decisions they feel are appropriate for their child, family, and values (Mack et al. 2007b).
High-quality prognostic communication may improve with clinician experience. Physicians who are older or more experienced tend to have higher rates of concordance with their patients’ families regarding cure likelihood and goals of care (Mack et al. 2007a; Rosenberg et al. 2014b). While most providers report learning their communication skills through trial and error (Hilden et al. 2001), recent studies suggest that effective advance care communication skills can be taught (Back et al. 2007; Bylund et al. 2010).
Overcoming Barriers
A critical component of effective communication is recognizing these barriers and understanding why they exist. The death of a child seems inherently unnatural. It is normal for parents to hold out hope for a cure, extended life, or a miracle. “Leaving no stone unturned” is an appropriate parent response (Bluebond-Langner et al. 2007). Recent evidence suggests that mild (e.g., outpatient, oral) cancer-directed therapy may be psychologically beneficial to children as well (Wolfe et al. 2015).
Providers are responsible for relaying information honestly and compassionately such that families may establish appropriate goals of care, make informed decisions, and fully support their child’s whole well-being. Interdisciplinary staff may be helpful, if not necessary, for successful communication. Wolfe et al. have previously found that involvement of a psychosocial or PPC clinician in end-of-life care is associated with alignment of physician and parent prognostic understanding and likely patient and family experiences as a whole (Wolfe et al. 2000b).
Guidelines for Effective Communication regarding Prognosis and Goals of Care
Several strategies for effective communication have been described (Von Gunten et al. 2000; Baile et al. 2000; Beale et al. 2005; Makoul 2001), all of which include similar guiding principles and efforts to make a human connection with the child and family (Table 14.1). A simple but successful outcome of effective communication regarding prognosis or goals of care is when families are able to “expect the worst” (e.g., fully understand and anticipate potentially difficult experiences, including the child’s death) while also “hoping for the best” (e.g., maintaining realistic hopes and goals while also identifying with their own good parent roles). This dual reality may, in turn, promote better patient and family coping, adjustment, and quality of life (Hill et al. 2013).
Table 14.1
Guidelines for effective communication regarding prognosis and goals of care
Step | Practice | Examples |
|---|---|---|
1. | Prepare for the discussion | Setting up the interview, planning the setting, establishing a protocol for communication, and determining who should be present (this should involve efforts to understand and respect a family’s own needs and styles for communication, including when/how to involve the child him- or herself) |
2. | Establish what the patient and family already know, as well as their objectives for the conversation | (For first-time interactions): “I have read your medical chart and learned about you, but it would help me to hear, in your own words, what is your understanding of what is happening with your child?” (For already established relationships):“I have some things I’d like to talk about today, but before I start, I’d like to know what you hope to discuss?” |
3. | Deliver information | Explaining medical information according to the child’s developmental status and the family’s needs and choosing appropriate strategies, including assessments of family’s understanding (these may also include obtaining an invitation from the patient/family) |
4. | Respond to emotions | Listening attentively, maintaining openness, providing safe silence, and affirming the love and struggle that went into particular decisions |
5. | Establish goals for care and treatment priorities | “As you think about what is ahead for your child, what is most important to you?” “What does good quality of life look like for your child?” |
6. | Establish a plan | Evaluating understanding, summarizing, and delineating next steps. This step underscores the ongoing nature of the relationship, decisions being made, and supportive care |
Decision-Making and Advance Care Planning
At more advanced stages of cancer, delineation of goals of care becomes a particularly important element of decision-making. When goals are clear, decisions regarding therapy may fall into place. For example, a parent whose goal is to “extend time with my child, without hope of cure” may decline intensive inpatient chemotherapy in favor of oral medications that can be administered at home. This alignment is especially true when clinicians apply models of shared decision-making, where exploring goals of care with patients and families may lead to discussions of how those goals may be best met (Waldman and Wolfe 2013).
Box 14.2: Phrases and Questions That May Elicit Goals of Care
Words that work: common phrases and questions used to elicit goals of care |
Tell me about you (your child) as a person. |
What is your understanding of your (your child’s) illness? |
In light of your understanding, what is most important to you? |
What are you hoping for? What are your worries? |
In times of difficulty, where do you find your strength? How well is that working for you? |
What do you think has caused you (your child) to suffer the most? |
What makes you (your child) most joyful? |
Advance care planning (ACP) refers to the process of thinking about, talking about, and planning for future health care and end-of-life care. Engaging in ACP may be challenging for the same reasons it is difficult for patients, parents, and providers to discuss poor prognosis. In essence, preparing for a child’s death may feel inherently unnatural and be plagued by emotional distress, avoidance, and uncertainty. Determining if, when, and to what extent pediatric and adolescent patients are included in ACP discussions may be an additional challenge. Parents and providers may want to protect their children and therefore deliberately shield them from difficult conversations (de Vries et al. 2010). However, children ages 14 years and older often have adult-level comprehension of their situation and the consequences of their decisions. Patients between 10 and 20 years old report that “thinking about their relationships with others” is the single most important factor in their choices regarding continued cancer treatment and goals of care (Hinds et al. 2005). Nearly all adolescents and young adults living with life-threatening illness report wanting to be able to choose and record the kind of treatment they do (and do not) want, how they want to be cared for, what they want to share with others, and how they want to be remembered (Wiener et al. 2012).
Evidence suggests patients as young as 3 years old are aware of their prognosis without being told (Bluebond-Langner 1978). Patients of all ages who are unaware or shielded may paradoxically feel greater distress or anxiety by “not knowing;” providing age-appropriate honest information may alleviate some patients’ fears. When patients are present for initial discussions about diagnosis and prognosis, parent distress is significantly decreased (Mack et al. 2006). Likewise, among over 400 bereaved parents, none of those who talked to their child about death regretted having done so, but 27 % of those who avoided the topic regretted the lost opportunity (Kreicbergs et al. 2004b). The corollary is also true; nearly three quarters of parents did not experience regret. Most important, therefore, is to uncover and respect the family communication style.
One approach to gauge readiness for advance care planning is to ask patients and families: (1) whether talking about what would happen if treatment was no longer effective would be helpful, (2) whether talking about medical care plans ahead of time would be upsetting, and (3) whether they would be comfortable writing down/discussing what would happen if treatments were no longer effective (Wiener et al. 2008). Other more specific and age-appropriate instruments have also been developed and can help guide conversations and address critical elements of patient and family values, beliefs, goals, hopes, and worries (Table 14.2) (Zadeh et al. 2014; agingwithdignity.org).
Table 14.2
Examples of advance care planning tools
Age group | Tool name | Included concepts | Examples of activities |
|---|---|---|---|
Pediatric | “My wishes” | How I want people to treat me How comfortable I want to be What I want my loved ones to know What I want my doctors and nurses to know | Drawing, storytelling, journaling |
Adolescent and young adult | “Voicing my CHOiCES” | How I want to be comforted How I would like to be supported (so I don’t feel so alone) Who I want to make my medical care decisions if I cannot make them on my own Types of life support I want or do not want What I would like my family and friends to know about me My spiritual thoughts and wishes How I wish to be remembered | Detailed checklists of advance directives including delegated decision-makers and requests for “do not resuscitate” discussions, as well as open-ended storytelling, journaling, and directed writings |
Adults (>18 years old) | “5 Wishes” | The person I want to make health-care decisions when I can’t The kind of medical treatment I want (or don’t want) How comfortable I want to be How I want people to treat me What I want my loved ones to know | Detailed checklists of advanced directives, legally binding in 42 states in the United States. Also includes open space for free writing and individual requests |
Other types of anticipatory guidance should include discussions about the child’s resuscitation status, preferred location of death, organ and/or tissue donation and autopsy, and funeral planning. Of note, many children who die from advanced cancer will not be candidates for organ donation due to concerns for disseminated cancer in body tissues. Other children only have isolated eligible tissues (e.g., their corneas). It is important to communicate to families who wish to donate that their preference is heard and honored, even if it cannot be met. Autopsy should be offered to every family. In a study of 30 bereaved parents, only 37 % recalled a conversation about autopsy, and 90 % of those who did not recall such conversations suggested they would have considered the procedure. The majority of parents indicated that discussions about autopsy would be appropriate when it is clear that cure is no longer possible, rather than at the time of their child’s death. Furthermore, educating parents about the potential research, emotional, and clinical benefits of autopsy would enable their informed decision-making (Wiener et al. 2014). Parents who choose autopsy for their children often do so to advance medical knowledge and/or respect their child’s wishes. Among 33 bereaved parents of children with brain tumors, none who requested autopsy regretted it, and 91 % stated they would make the same choice again (Baker et al. 2013). We have found that some parents may also find peace in knowing the definitive cause of their child’s death, while others may decline because they feel that they “know” the cause. Either choice is appropriate.
PPC care team involvement can help facilitate ACP. If PPC providers were involved early in the cancer experience, they may have joined the primary psychosocial oncology team in helping the family with initial adjustments to cancer and to challenges that develop over time. Later PPC involvement may then feel more seamless in advanced stages of the illness (Waldman and Wolfe 2013). Studies have shown that changes in terminology (e.g., “advanced care team” or “supportive care team”) may also lead to increased referrals, particularly later in the cancer experience (Dalal et al. 2011). Better description of palliative care as ‘an added layer of support’ may also enable its involvement. PPC expertise can help guide communication, enabling medical personnel to effectively and compassionately relay difficult concepts, thereby facilitating family understanding and, in turn, realistic expectations. Furthermore, PPC can assist with very difficult decision-making for parents, providers, and patients alike. Combined, PPC involvement may alleviate patient, parent, and provider suffering.
Continued Cancer-Directed Therapy and Phase I Clinical Trials
In advanced pediatric cancer, it is often unclear to what extent cancer-directed treatment will be effective. And as described above, it is natural for parents (and providers) to hold out hope for a cure and leave no stone unturned. This continued search for treatment options often includes consideration of enrollment in phase I clinical trials. Few studies, however, have described how parents or providers make decisions about experimental therapies. The goal of phase I research is to identify appropriate dosage and safety data for new drugs, not to demonstrate efficacy or to impact curability. It is unclear how many patients or parents are aware of this fact (Agrawal and Emanuel 2003). For example, the most common reason parents enroll in clinical research studies is to receive some direct medical benefit for their child; only 20 % report wanting to help future patients (Truong et al. 2011). Most adolescent patients hope enrolling in phase I studies will extend their lives (Miller et al. 2013), but many also endorse wanting to help other patients (Wendler et al. 2012). It is the responsibility of the interdisciplinary team to explore patients’ and families’ understanding of phase I research, their reasons for enrolling, and their hopes and other goals of care. Often, these conversations can be easily integrated into other decision-making and ACP discussions.
Patients with advanced cancer may also request continued, nonexperimental cancer-directed therapy, even when its efficacy is limited. This request may align with goals of care and parenting roles, as well as alleviate patient suffering and prolong time with family. Sometimes, however, cancer-directed therapy can directly impede quality of life, due to side effects, the need to be proximal to the hospital, restrictions in activities, and other clinical (or investigational study) requirements. Understanding patients’ and/or families’ specific values and goals of cancer-directed therapy therefore becomes more important over time. Eventually, quality of life may become a major factor in patient, parent, and provider decision-making, and providers must enable families to support the child’s quality of life, perhaps by giving them permission to reframe their goals and responsibilities.
Concurrent Care Models
The integration of palliative care has never necessitated forgoing other forms of treatment; however, because families and providers may link palliative care and hospice with the cessation of cancer-directed therapy, referrals to palliative care may occur late. In the United States, this bias may extend from legislation passed in the 1980s, defining hospice as a Medicare benefit that required patients to have a prognosis of 6 months or less and because of limited reimbursement mechanisms also required patients to forgo continued cancer-directed therapy. Outside of the United States, hospice is a term used to describe a philosophy of care that focuses on alleviating the suffering of patients with advanced illness. It may also be used in association with a specific location for end-of-life services.
Hospice care for pediatric cancer patients remains largely underutilized in the United States, perhaps because it is associated with similar barriers to palliative care services (Fowler et al. 2006). One approach to promoting early and ongoing PPC involvement is the relatively new provision of palliative and hospice care concurrently with cancer-related therapies. In 2010, the United States implemented the Affordable Care Act (ACA) in an effort to expand population access to multiple medical services. Included in this program was a provision, Section 2303, termed the “Concurrent Care for Children” Requirement (CCCR), allowing publicly insured children with life-limiting illness to receive “curative” treatments like chemotherapy or dialysis concurrently with hospice care. The program has several notable limitations, including a stipulation that children receiving this benefit have a life expectancy of fewer than 6 months. While the program has the potential to allow children with high needs to receive complete end-of-life care at home, few states have successfully implemented models of concurrent care for pediatric cancer patients to date. The long-term effect of this critical change has yet to be measured (Bona et al. 2014).
Location of Death
As research and clinical efforts have focused on improving quality of palliative and end-of-life care for children with cancer, the location of their deaths has also received attention. In the United States, most children and families may choose between death at home (with or without hospice) and death in the hospital. Very few states offer free-standing hospice facilities. In contrast, the latter are more standard in the United Kingdom and Canada. In Canada, parents of children with cancer and their health-care providers tend to prefer home as their first choice for end-of-life care and for the location of their child’s death (Kassam et al. 2014). Most importantly, however, is that families have the opportunity to plan the location of their child’s death, because in doing so, they experience less decisional regret (Dussel et al. 2009).
One challenge in enabling children to die at home is concurrently meeting their pain and symptom management needs. Children may often return to the hospital for intractable symptom control or because parents become overwhelmed or exhausted while caring for them. Children who receive PPC services, however, are more likely to die in their or their parents’ preferred location, providing another testament to the value of palliative care team integration in pediatric cancer care (Postier et al. 2014; Friedrichsdorf et al. 2015). Comprehensive end-of-life care should therefore address these preferences early, in order to plan and accommodate patient and/or family wishes.
Pain and Symptom Management
Pain and symptom management is often the initial or primary reason for a palliative care referral. Parents of children with cancer report that pain, emotional distress, fatigue, and nutrition “cause the most problems” during cancer treatment, and these problems are associated with parent and survivor distress (Heden et al. 2013; Poder et al. 2010; Rosenberg et al. 2013). The most commonly reported symptoms are fatigue, reduced mobility, pain, anorexia, nausea, vomiting, and disordered mood, and these are often intertwined (Jalmsell et al. 2006). Many physical symptoms have psychosocial components and vice versa (Wolfe et al. 2015). For example, 96 % of children experience fatigue in the last month of life, and suffering from fatigue is associated with additional suffering from pain, dyspnea, anxiety, sadness, fear, diarrhea, nausea, vomiting, and anorexia (Ullrich et al. 2010b).
Certain cancer types, treatment regimens, and patient-ages may be related to symptom complaints and their management. For example, patients with central nervous system (CNS) tumors have higher prevalence of neurocognitive deficits, impaired speech, or other motor dysfunctions (Jalmsell et al. 2006). Some studies suggest patients with leukemia or lymphoma report worse physical and psychosocial quality of life compared to those with solid non-CNS and CNS tumors, and recent HSCT is associated with worse psychosocial health (Tomlinson et al. 2011). Other studies suggest that patients with bone sarcoma have greater disability and inferior quality of life (Nagarajan et al. 2004; Barrera et al. 2012). Finally, patients diagnosed as adolescents and young adults may be at higher risk of depression, anxiety, and fatigue (Poder et al. 2010).
At the end of life, the prevalence of troubling symptoms is particularly high; 89 % of bereaved parents believe their children suffered “a lot” or “a great deal” in the last month of life (Wolfe et al. 2000b). Unfortunately, treatment of specific symptoms is frequently inadequate. For example, bereaved parents report their child received treatment for pain (80 %), dyspnea (70 %), or fatigue (20 %), but these treatments were successful in only 27, 16, and 5 % of cases, respectively (Wolfe et al. 2000a). Additionally, the symptoms that become the most distressing to parents are those which are persistently unrelieved (Pritchard et al. 2010), and parents are more likely to consider hastening their child’s death if they believe their child is suffering (Dussel et al. 2010).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


