Chapter 15 Early Pregnancy
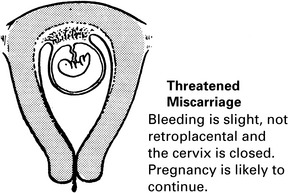
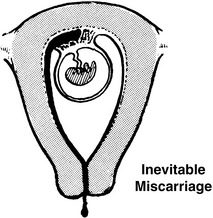
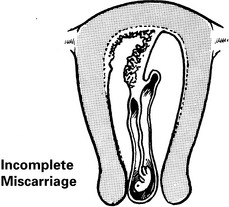
Miscarriage
Management
Early pregnancy loss (≤12Weeks’ Gestation)
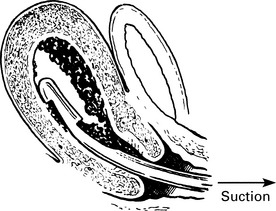
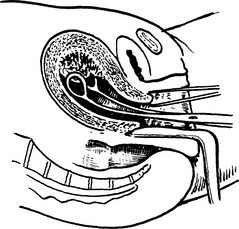
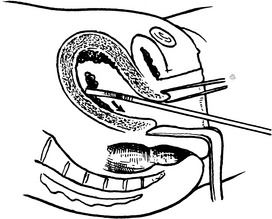
Surgical Evacuation of the Products of Conception
Complications
3. Sepsis. Broad spectrum antibiotics have been shown to minimise the risk of post-abortal infection.
4. Haemorrhage. Blood loss can be minimised by the use of prostaglandins for preoperative cervical ripening. Bleeding during or after the procedure can be reduced by oxytocic agents such as ergometrine or Syntocinon.