Fig. 17.1
(a) After saline application. (b) After acetic acid application. (c) After Lugol’s iodine application
Answer 3 – This is an adequate colposcopy with a completely visible squamocolumnar junction (SCJ), Type 1 transformation zone (TZ) with no colposcopic abnormal finding.
Q.4 After 1 year, repeat HPV 18 was positive and LBC was negative – persistent HPV infection. How will you counsel this lady? What will be the follow-up?
Answer – The patient needs to be counseled regarding persistent infection with high-risk HPV, but she has a normal Pap test with a normal colposcopy so she will require a regular follow-up with a yearly co-testing.
Further this patient can undergo triage with E6/7mRNA depending on the facilities available. The partners of this patient should also be examined for HPV infection.
Case 2
A 32-year-old lady, P1L1, last childbirth – 5 years.
The routine cytology screening shows Atypical squamous cell of undetermined significance (ASCUS).
Q.1 What will be your next step?
Answer 1 – Women with ASCUS on cervical cytology should be triaged with the high-risk HPV DNA testing. If negative for high-risk HPV DNA, then repeat cytology at 12 months. If positive for high-risk HPV DNA, then refer for colposcopy.
Q.2 The patient underwent high-risk HPV DNA testing, which came as positive. Colposcopy was done. Describe the colposcopy findings (Fig. 17.2).

Fig. 17.2
Colposcopy after the application of acetic acid
Answer 2 – It is an adequate colposcopy with a completely visible SCJ. Many tongues of the acetowhite epithelium with ill-defined margins and flat surface are seen on the transformation zone, occupying two quadrants of the cervix, with no vascular abnormality. These findings are consistent with low-grade lesions.
Q.3 How will you manage this patient?
Answer 3 – Women with positive HPV with ASCUS are at an increased risk of Cervical intraepithelial neoplasia (CIN) 3 (11 %) within 2 years of referral for colposcopy. This patient needs excision/ Loop electrosurgical excision procedure (LEEP) rather than surveillance.
Q.4 The Histopathological examination (HPE) report shows mild dysplasia with clear margins. How will you follow up this patient?
Answer 4 – The patient should be checked in 1 month for healing. Followed by co-testing in 9–12 months. If two consecutive screens are negative, then the patient should undergo routine screening.
Case 3
A 28-year-old woman was referred to the clinic with an abnormal smear. Her two previous smears were negative. Her periods were regular with a combined oral contraceptive pill she used for contraception. She had no history of postcoital bleeding or vaginal discharge. She is in a stable relationship and has one child delivered by cesarean section (Fig. 17.3).
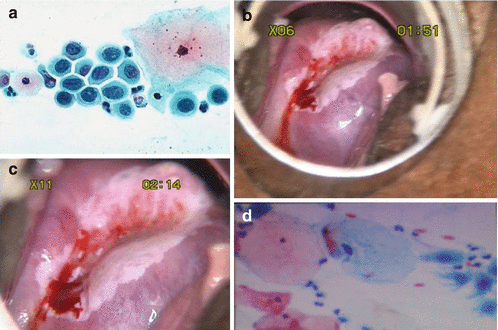

Fig. 17.3
(a) HSIL. (b) After the application of acetic acid. (c) Magnified view. (d) Normal smear
Q.1 Describe the smear.
Answer – The nuclei show a markedly increased nuclear/cytoplasmic ratio, anisocytosis (variation in size), hyperchromatism (increased intensity of staining), irregularity of nuclear chromatin, and irregular nuclear membranes. These are features of a high-grade intraepithelial lesion (HSIL).
Q.2 Colposcopy was done for this patient. Describe the findings.
Answer – Colposcopy is adequate, with SCJ not visible (Type 3 TZ). There is a dense acetowhite area with sharp borders involving all four quadrants in the TZ; the upper margin of the lesion is not visible. These findings are suggestive of a high-grade lesion.
Q.3 What is the risk of invasion in this high-grade lesion?
Answer – The risk of invasion is approximately 30 % over 5 years for CIN III.
Q.4 What will be your modality of treatment – excisional treatment (LEEP/cone biopsy) or ablative treatment?
Answer – This patient should undergo a cone biopsy going well beyond the lesion, considering that it is a high-grade lesion involving a large area whose upper margin is not visible.
Q.5 Unfortunately, a loop excision of TZ (LEEP/ Large loop excision of transformation zone (LLETZ)) confirmed CIN III, which was incompletely excised at the endocervical margin. Does she require repeat excision?
Answer – Such patients are known to have a slightly increased risk of recurrent CIN [1] but re-treatment is not required unless the cytology indicates a persistent or recurrent high-grade disease.
Q.6. Six months later, a further smear was taken at colposcopy. Describe the findings.
Answer – This is a normal smear with predominantly superficial and intermediate cells, with normal nucleic cytoplasmic ratio.
Q.7 How will you follow up this patient?
Answer – She should be kept under six monthly follow-ups by both cytology and colposcopy. After a 1-year follow-up, and with two consecutive negative reports of cytology as well as colposcopy, she can return to the routine screening program.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


