45 Arrhythmias
Although infrequent in the pediatric population, arrhythmias represent potentially significant causes of morbidity and mortality. The diagnosis and management of arrhythmias require an understanding of age-dependent normal variations in heart rate (Table 45-1). This chapter describes the etiology, clinical significance, and treatment options of common arrhythmias found in infants, children, and adolescents, including bradyarrhythmias, tachyarrhythmias, and rhythm disturbances leading to syncope and sudden death.
Table 45-1 Normal Heart Rate for Age
| Age | Heart Rate (beats/min) |
|---|---|
| Newborn | 110-160 |
| 1-6 months | 100-180 |
| 6-12 months | 95-170 |
| 1-3 years | 95-150 |
| 3-5 years | 70-130 |
| 5-8 years | 65-120 |
| 8-12 years | 65-120 |
| 12-16 years | 60-110 |
| >16 years | 60-100 |
Sinus Arrhythmias and Premature Impulses
Bradyarrhythmias
Atrioventricular Conduction Abnormalities
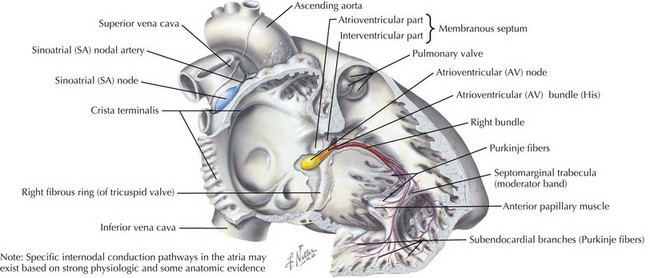
Abnormal AV conduction occurs when transmission of the normal sinus node impulses is delayed or blocked because of an abnormality in the conduction system, specifically the AV node or His-Purkinje system (Figure 45-1).
First-Degree Atrioventricular Block
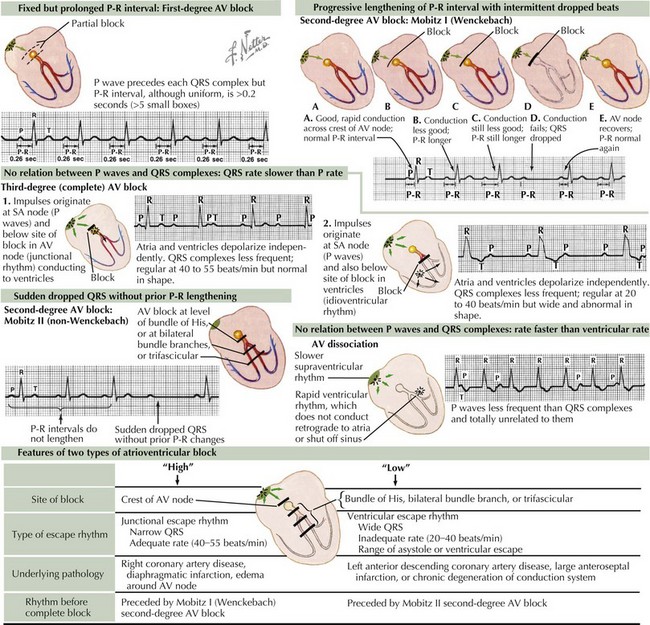
Because of an abnormal delay in conduction through the AV node, first-degree AV block results in prolongation of the PR interval above the upper limits of normal for age and heart rate (Figure 45-2). It is important to note that bradycardia does not occur because of first-degree AV block alone. This type of block can appear in otherwise healthy children as a benign phenomenon, usually related to increased vagal tone. Other causes may include cardiac surgery, rheumatic fever, Lyme disease, digoxin toxicity, and electrolyte imbalance. Isolated first-degree AV block does not require treatment unless there is progression to more advanced AV block.
Second-Degree Atrioventricular Block
Mobitz Type I (Wenckebach phenomenon) occurs at the level of the AV node, yielding progressive lengthening in the PR interval until one QRS complex or ventricular depolarization fails to occur (see Figure 45-2). This may occur in otherwise healthy children with parasympathetic dominance as well as in trained athletes and is frequently observed during monitoring of heart rates during sleep. After confirmation via surface ECG, management should focus on treating any underlying pathologic causes.
Mobitz type II occurs at the level of the bundle of His and is defined as the intermittent loss of AV conduction without preceding lengthening of the PR interval. This form of second-degree AV block is less common and suggests a more serious form of AV conduction disorder in which progression to complete heart block with hemodynamic compromise is more likely. Although similar causes exist between Mobitz type I and type II, consultation with a pediatric cardiologist is indicated (see Figure 45-2).
Third-Degree Atrioventricular Block or Complete Atrioventricular Block
Complete AV block is defined as complete interruption of atrial impulse propagation, resulting in atrial and ventricular activity that is independent of each other (AV dissociation). Surface ECG morphology will show regular P waves at a rate appropriate for age but with QRS complexes occurring at regular and slower rates than the atrial rate with no consistent relationship between P waves and QRS complexes. Both congenital and acquired forms of complete AV block occur and should be suspected in any patient with symptomatic bradycardia (see Figure 45-2).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree