Fig. 13.1
The comprehensive model of pediatric adherence promotion, showing patient flow from risk assessment through triage and intervention, to yearly reassessment
Assessed Risk
Triage is based on assessed risk level. Following Kazak’s PPPHM (Kazak 2006), the model defines three risk levels or categories of need, as shown in Table 13.1. Assessed risk level then determines the type and intensity of intervention. Important risk factors include:
Low SES
Single-parent family
Caregiver unemployment
Child behavioral or psychological concerns
Parent mental health problems
Family conflict (including marital conflict)
A current history of nonadherence (established patients)
As a rough rule of thumb, having two risk factors (or one risk factor plus poor illness control) would place a patient in the moderate risk category, and three or more risk factors would place a child in the high risk category (Schwartz et al. 2014). However, problem severity and parent distress/desire for intervention should also be taken into account when making this determination. For example, a child with significant behavior problems but no other concerns would likely still warrant clinical intervention.
Table 13.1
The risk categorization model and indications for intervention
Risk level | Characterization | Indication for intervention |
|---|---|---|
High risk (Clinical) | Clinically significant concerns with child or family functioning | Individualized treatment |
Moderate risk | Risk factors for problematic adjustment or adherence Limited resources | Preventive low-level interventions designed to minimize risk and keep the child and family connected to the healthcare system |
Low risk | Good coping, good support, adequate resources | Universal educational resources and illness management tools |
Interventions
Interventions should be offered based on assessed level of risk/need to ensure efficient allocation of resources and to cover the range of needs, from universal education to clinical intervention. Below we give an overview of the type of intervention indicated at each level, according to current evidence-based practice in behavioral health. The actual interventions are described in greater detail in the sections that follow.
Importantly, patients at higher levels of assessed need should also have access to interventions at lower levels. Thus, moderate risk patients would have access to the educational materials and management tools as well as to targeted interventions, and high risk patients would have access to all of the different intervention components.
High risk. Patients assessed to have clinically-significant concerns should be seen by or referred to a pediatric psychologist or other specialist in behavioral or mental health, for individually tailored intervention. High acuity patients (e.g., with suicidal ideation) would probably need to be seen outside of the system being presented here.
Moderate risk. Moderate risk patients are characterized either by a single child or family-related risk factor (e.g., family conflict), or by one or more resource limitations. The primary goals for these patients should be to minimize risk, prevent complications, and help keep the family tied in to the system. Thus, appropriate supports at this level would be targeted interventions focused on the specific area of risk identified (e.g., child behavior problem), help obtaining resources (e.g., from a social worker), and/or support for navigating the healthcare system (via a patient navigator or Care Ambassador (see below), depending on specific needs.
Low risk patients have adequate coping and supports. The indicated intervention at this level would be universal educational materials, and access to illness management tools that could make living with and managing their disease easier.
Yearly Psychosocial Reassessment
For many patients, problems with adherence do not emerge until they have lived with the illness for a while. Some children and youth may experience management burnout (Polonsky 1996). Others may pass through the developmental transition into adolescence, a time during which illness management and control is known to be especially challenging, or may encounter other stressors that complicate management. As a result, continued monitoring of patients’ adherence and psychosocial functioning is critical.
A Web-Based System for Evidence-Based Intervention at All Levels of Risk/need
Designing and implementing this sort of comprehensive system is by no means easy. Significant resources need to be available to address each component, and the model needs to be sustainable over time. To accomplish this, we believe use of an internet-based hub could make implementation feasible. A web-based hub could house the educational materials and tools, utilize software for screening, provide a platform for eHealth and mHealth interventions, and link patients to clinical staff, care navigators, and the larger patient community (Fig. 11).
Web-based interventions have be shown to be effective in promoting health and reducing nonadherence across a wide-range of illnesses. They also have substantial ability for improving the reach, accessibility, effectiveness, and cost-effectiveness of interventions (Bennett and Glasgow 2009; Murray 2012). Internet–based programs have the potential to disseminate effective interventions to very large groups of people, making them an ideal format for large-scale efforts at health promotion. Their large reach helps ensure that even small changes across a population can have a substantial impact on public health (Murray 2012).
Internet and mobile technologies have a high level of uptake among children, teens, and young adults, having been integrated into their lives in an unprecedented fashion. As such, these technologies provide a natural way to monitor patients’ health and well-being, provide them with reminders and other contact, and keep them connected to their healthcare on weekly or even daily basis, with a relatively low “footprint” and minimal intrusiveness into their daily lives. eHealth and mHealth interventions also have the potential to be more acceptable to patients who would be reluctant to go see a psychologist or psychiatrist, thereby increasing the reach of effective services to patients who might otherwise “fall through the cracks.”
In the next section we describe how a web-based hub could be used to link and integrate the different components of a multi-level, multimodal system for promoting adherence. We sketch out a system with two access points: a public portal, freely open and available to the public; and a patient portal, accessible only to patients being treated at a specific institution (Fig. 13.2).
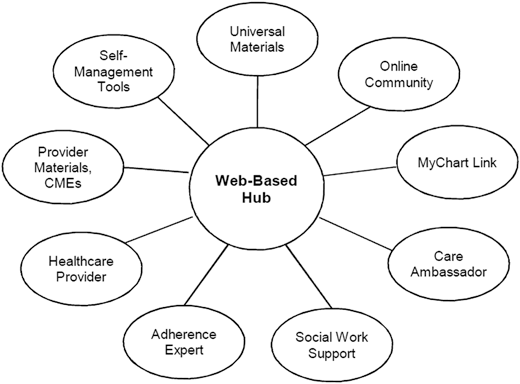
Fig. 13.2
A web-based hub linking patients to services at different levels
Universal Preventive Services
The Public Portal
Universal educational resources and tools could be provided for patients and the public at large as a primary prevention strategy to help promote treatment adherence. To be most effective, materials should be developed specifically for different age groups (children, teens, and parents), and in some cases also for specific-diseases.
Important educational resources to consider for inclusion in the public portal include:
Basic information on medical treatments for specific (targeted) medical populations, including best practice treatment guidelines abstracted from the current literature and written in a patient-friendly format
Disease-specific information on high risk behaviors—e.g., insulin omission in diabetes
Adherence “tips” and informational pages on topics such as problem-solving, stress management, and managing family conflict
Patient essays and videos presenting personal stories about challenges and successes in managing different chronic illnesses
Links to local, regional, and national resources
Important web-based tools to help with illness management include:
Customizable medication reminders linked to the patient’s phone
Customizable appointment reminders
An interactive problem-solver program to help patients develop possible solutions to common adherence problems and barriers
A nonadherence risk assessment tool (e.g., the RI-PGC; Schwartz et al. 2014, in which the user answers a few questions and receives a computer-generated risk estimate for possible nonadherence with linked suggestions for seeking further care.
The website could also be used to house professionally monitored discussion forum(s), to provide access to a patient community. It would be important for these forums to have lower age limits (e.g., 12 and older), to be disease-specific, and to be carefully monitored for potentially harmful information (e.g., diabetic teens sharing the information that omitting insulin can be an effective way to control weight).
The Patient Portal
In addition to the universal materials and tools suggested above, patients in participating clinics could also be given access to tools and supports linked to their medical chart and to the hospital/clinic where they receive their treatment. Of course, security concerns in designing this system would be paramount, to ensure that only the patient (and his/her legal guardians) would have access to the information. The following elements would be important to include:
1.
Patient-specific health information
A link to the patient’s medical chart
A downloadable summary of the patient’s current treatment regimen (prepared by his/her healthcare provider), formatted to be maximally useful and easy to read
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


